- Overview & Types
- Symptoms & Diagnosis
- Treatment
- Living With
- Related Conditions
- Type 2 Diabetes
- Type 1 Diabetes
- Gestational Diabetes
- Appointment Prep
- View Full Guide
Slideshow: A Visual Guide to Type 2 Diabetes


What Is It?
When you have this disease, your body does a poor job turning the carbohydrates in food into energy. This causes sugar to build up in your blood. Over time it raises your risk for heart disease, blindness, nerve and organ damage, and other serious conditions. It strikes people of all ages, and early symptoms are mild. About 1 out of 3 people with type 2 diabetes don't know they have it.

What Will You Notice First?
People with type 2 diabetes often have no symptoms. When they do appear, one of the first may be being thirsty a lot. Others include dry mouth, bigger appetite, peeing a lot -- sometimes as often as every hour -- and unusual weight loss or gain.

Later Symptoms
As your blood sugar levels get higher, you may have other problems like headaches, blurred vision, and fatigue.
Signs of Serious Problems
In many cases, type 2 diabetes isn't discovered until it takes a serious toll on your health. Some red flags include:
- Cuts or sores that are slow to heal
- Frequent yeast infections or urinary tract infections
- Itchy skin, especially in the groin area

It Can Affect Your Sex Life
Diabetes can damage blood vessels and nerves in your genitals. This could lead to a loss of feeling and make it hard to have an orgasm. Women are also prone to vaginal dryness. About 1 in 3 who have diabetes will have some form of sexual trouble. Between 35% and 70% of men who have the disease will have at least some degree of impotence in their lifetime.

Risk Factors You Can Control
Some health habits and medical conditions related to your lifestyle can raise your odds of having type 2 diabetes, including:
- Being overweight, especially at the waist
- A couch potato lifestyle
- Smoking
- Eating a lot of red meat, processed meat, high-fat dairy products, and sweets
- Unhealthy cholesterol and triglyceride levels

Risk Factors You Can't Control
Other risk factors are out of your control, including:
- Race or ethnicity: Hispanics, African-Americans, Native Americans, and Asians are more likely to get it
- Family history of diabetes: Having a parent or sibling with diabetes boosts your odds.
- Age: Being 45 and older raises your risk of type 2 diabetes.
The more risk factors you have, the more likely you'll get type 2 diabetes.

Risk Factors for Women
You're more likely to get type 2 diabetes later on if you:
- Had gestational diabetes when you were pregnant
- Delivered a baby that weighed over 9 pounds
- Had polycystic ovary syndrome
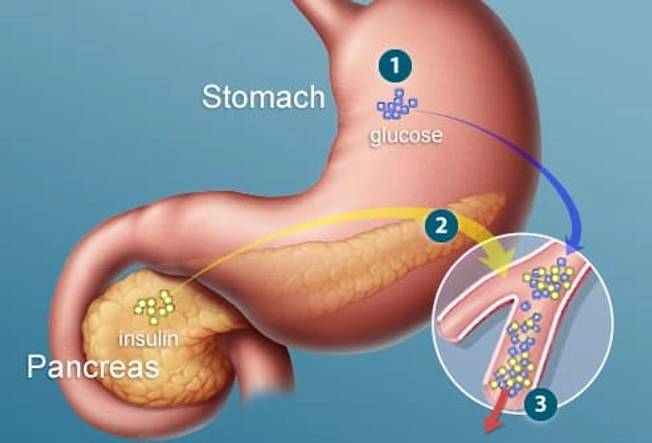
How Does Insulin Work?
In a healthy person, insulin helps turn food into energy. Your stomach breaks down carbohydrates into sugars. They enter the bloodstream, prompting your pancreas to release the hormone insulin in just the right amount. It helps your cells use the sugar for fuel.
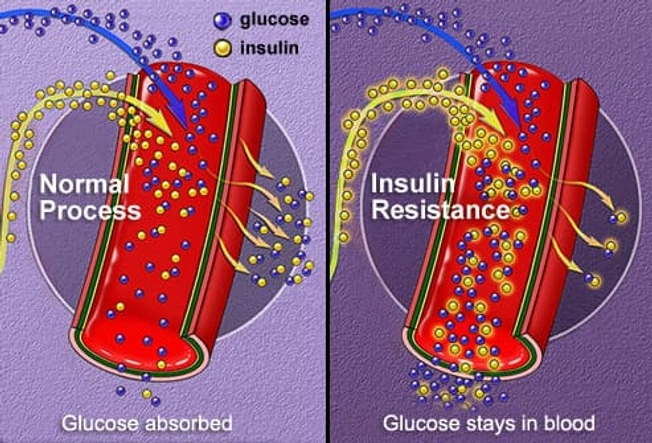
Metabolism Mishaps
In type 2 diabetes, your cells can’t use sugar properly. That means there's a lot of it in your blood. If you have a condition called insulin resistance, your body makes the hormone, but your cells don’t use it or respond to it like they should. If you’ve had type 2 diabetes for a while but haven’t treated it, your pancreas will make less insulin.
How Is It Diagnosed?
Your doctor will take some blood and do an A1c test. It shows your average blood sugar level over the past 2-3 months. If you already have symptoms, they might give you a random blood glucose test, which shows what your current level is.

Your Diet Makes a Difference
You can control blood sugar levels by changing your diet and losing extra weight. That will also cut your risk of complications. Carefully track the carbs in your diet. Keep amounts the same at every meal, watch how much fat and protein you eat, and cut calories. Ask your doctor to refer you to a dietitian to help you make healthy choices and an eating plan.

Exercise Is Important
Regular exercise, like strength training or walking, improves your body's use of insulin and can lower blood sugar levels. Being active also helps get rid of body fat, lower blood pressure, and protect you from heart disease. Try to get 30 minutes of moderate activity on most days of the week.

Relaxation Is Key
Stress can boost your blood pressure and blood sugar. Some people don't do anything for it. Others turn to food to cope with it. Instead, practice relaxation techniques like deep breathing, meditation, or visualization. Talking to a friend, family member, counselor, or a religious leader could help. If you can’t beat it, reach out to your doctor.

Oral Medications Can Help
If diet and exercise can’t get your blood sugar under control, your doctor may add medication. There are many types of diabetes pills available. They’re often combined. Some work by telling your pancreas to make more insulin. Others help your body use it better or block the digestion of starches. Some slow insulin breakdown. Newer oral drugs help your body pee out more sugar.
Insulin: It's Not Just for Type 1
Your doctor may prescribe insulin early in your treatment and combine it with pills. It can also help people with type 2 diabetes who develop "beta-cell failure." This means the cells in your pancreas no longer make insulin when blood sugar is high. If this happens, insulin will become part of your daily routine.
Non-Insulin Injectables
Drugs called non-insulin injectables are available for people with type 2 diabetes. These injectables cause your body to make insulin to control blood sugar levels.

Why Blood Sugar Testing Matters
Your doctor can show you how to use a glucose meter to check your blood sugar. This lets you know how your treatment plan is working. How often and when you test will be based on how well controlled your diabetes is, the type of treatment you use, and how stable your blood sugar is. Common testing times are when you wake up, before and after meals and exercise, and at bedtime.
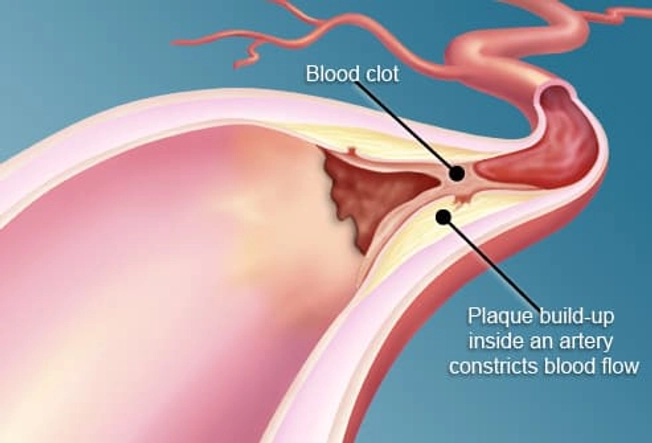
Heart and Artery Troubles
If you don't treat diabetes with a healthy diet and exercise, you're more likely to get plaque in your arteries than people who don't have it. This sticky substance slows blood flow and increases your risk of clots. It leads to hardening of the arteries (called atherosclerosis), which makes you more likely to have a heart attack or stroke. About 2 of 3 people with diabetes die of heart disease.

Kidney Complications
The longer you have diabetes, the greater the chance you’ll get chronic kidney disease. Diabetes is the leading cause of kidney failure. It's to blame for about half of new cases. Controlling your blood sugar, blood pressure, and cholesterol can lower your risk for this complication. Yearly tests and medications can slow the disease and keep your kidneys healthy.
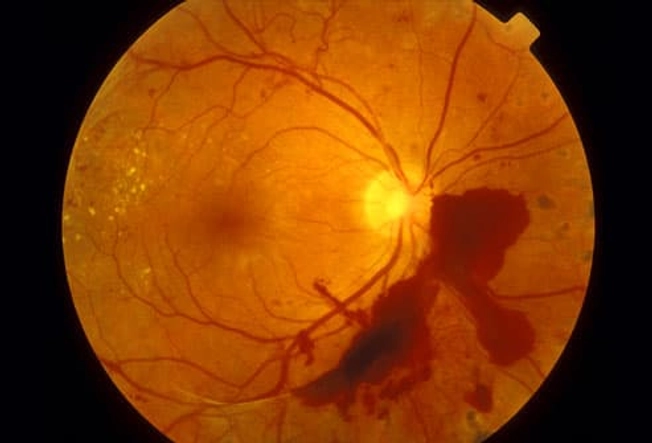
Eye Problems
High blood sugar can damage the tiny blood vessels that bring oxygen and nutrients to the retina, a critical part of your eye. This is known as diabetic retinopathy, and it can lead to vision loss. It’s the leading cause of new cases of blindness in people between the ages of 20 and 74. Pools of blood, or hemorrhages, on the retina of an eye are visible in this image.

Diabetic Nerve Pain
Over time, uncontrolled diabetes and high blood sugar can cause nerve damage. Symptoms include tingling, numbness, pain, and a pins and needles sensation -- often in your fingers, hands, toes, or feet. The damage can’t be reversed, but there are treatments. Controlling your diabetes can help prevent further harm.
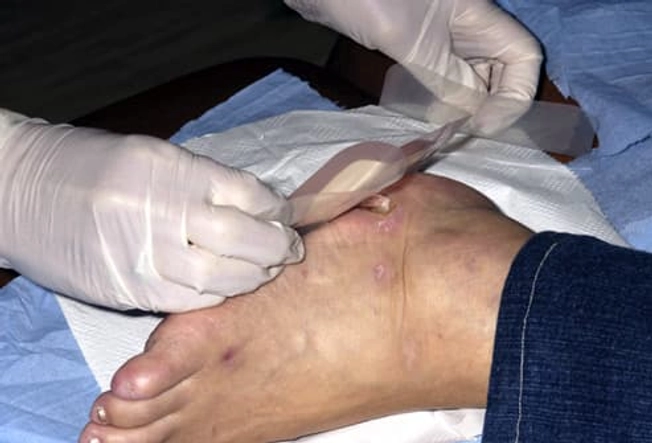
Foot Injuries Can Take a Toll
Diabetic nerve damage can make it hard to feel your feet. You might not notice wounds. At the same time, hardening of the arteries reduces blood flow to the area. Even a small injury can cause foot sores and gangrene. In severe cases, infections can result in an amputation.
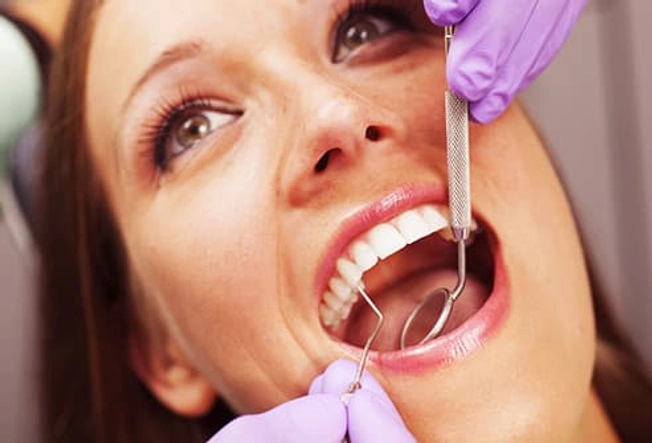
Teeth and Gums Are Targets
High blood sugar levels can feed the bacteria that make plaque. Plaque buildup leads to cavities, tooth decay, and gum disease. Severe gum disease can cause tooth loss. It weakens gums and the tissues and bones that hold teeth in place. That makes it easier to get an infection, too.

Can It Be Prevented?
One of the most surprising things about type 2 diabetes is that you can avoid it. To lower your risk, follow the same guidelines for warding off heart disease:
- Eat a healthy diet.
- Exercise for 30 minutes, 5 days a week.
- Stay at a healthy weight.
- Talk to your doctor about being tested for prediabetes.
People with prediabetes can avoid getting diabetes with lifestyle changes and medication.