A Visual Guide to Deep Vein Thrombosis

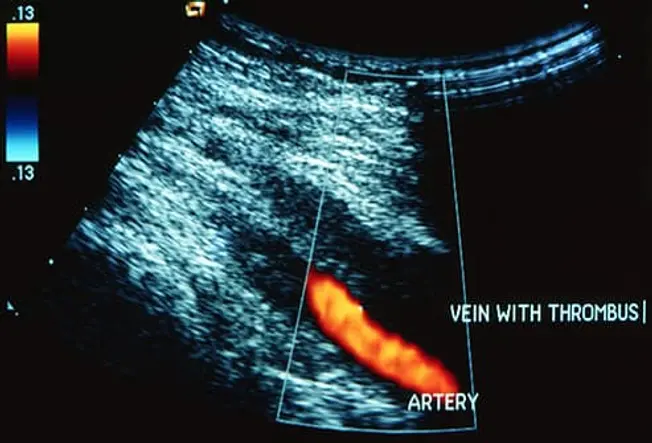
What Is DVT?
Deep vein thrombosis is a blood clot that forms inside a vein, usually deep within your leg. As many as 900,000 Americans a year get one, and up to 100,000 die because of it. The danger is that part of the clot can break off and travel through your bloodstream. It could get stuck in your lungs and block blood flow, causing organ damage or death.
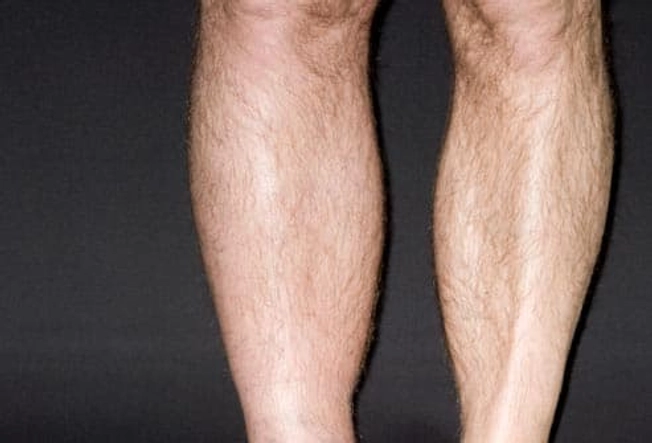
Symptoms
A common symptom of DVT is a leg swollen below the knee. You may have redness and tenderness or pain in the area of the clot.
But you won't always have these. About half of people with DVT get no warning signs.
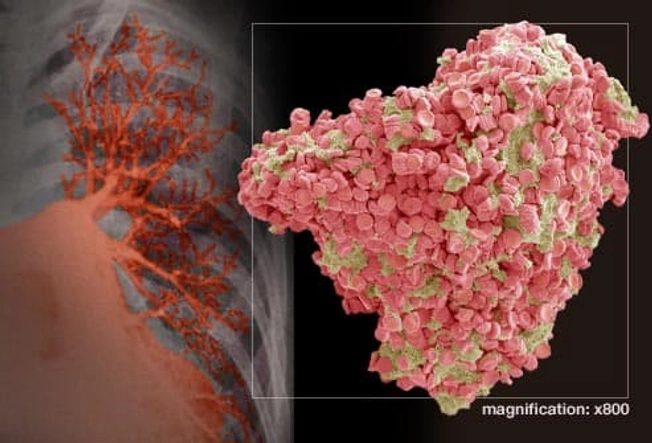
Pulmonary Embolism
This is a clot that moves into your lungs and blocks the blood supply. It can cause trouble breathing, low blood pressure, fainting, a faster heart rate, chest pain, and coughing up blood. If you have any of these, call 911 and get medical care right away.
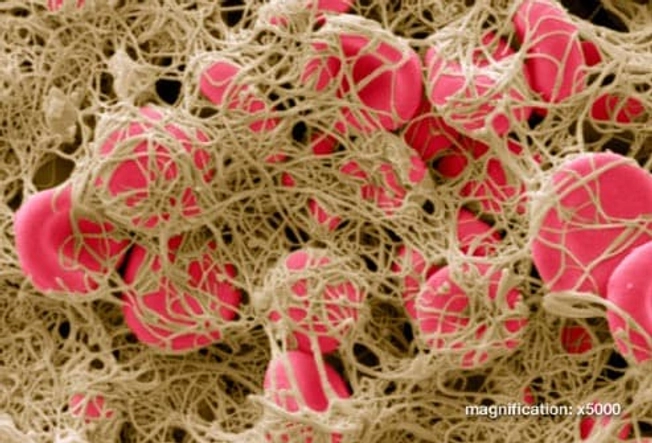
What Causes DVT?
Anything that damages the inner lining of a vein may cause DVT -- surgery, an injury, or your immune system. If your blood is thick or flows slowly, it's more likely to form a clot, especially in a vein that's already damaged. People who have certain genetic disorders or more estrogen in their system are more likely to have blood clots, too.

Who Is Likely to Get DVT?
Some people with a higher risk are those who:
- Have cancer
- Have had surgery
- Are on extended bed rest
- Are older
- Smoke
- Are overweight or obese
- Sit for long times, like on a long airplane flight
Pregnancy
Women are more likely to develop DVT during pregnancy and in the 4 to 6 weeks after giving birth. That's when they have higher levels of estrogen, which may make blood clot more easily. The pressure of their expanding uterus can slow blood flow in the veins as well. Certain blood disorders can boost their chances of having DVT even more.

Hormone Therapy
Like pregnancy, birth control pills and some treatments for postmenopausal symptoms raise the amount of estrogen in a woman's blood. That can increase the odds of getting DVT.

Trapped in Your Seat
Travel to new and faraway places can be exciting! Squishing into a coach seat for a long international flight is not. Studies show long-distance travel -- a trip that lasts more than 4 hours -- doubles the chance of developing DVT. It doesn't matter if you go by air, bus, train, or car. When you're in a cramped seat and don't move around, your blood flow slows.
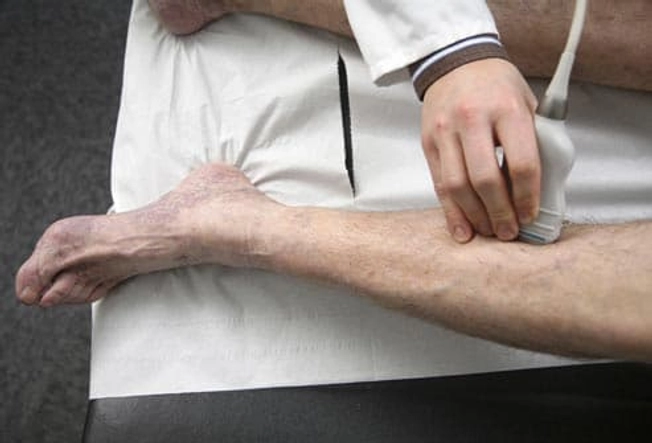
Diagnosis
Your doctor will check you for signs of DVT. They may also ask about your medical history, medications you're taking, medical problems of close relatives, and things that raise your chances of having this condition. An ultrasound is the most common way to confirm you have it. The test uses sound waves to "see" the blood flow and reveal a clot. You might also need other tests, such as a blood test called a d-dimer.
Blood Thinners
Drugs called anticoagulants are the most common way to treat DVT. Although they're known as blood thinners, they don't really thin your blood. They make it less "sticky" to prevent new blood clots from forming. They can't break up a clot you already have, but they will give your body time to dissolve one on its own. You take these medications in a pill or by needle.
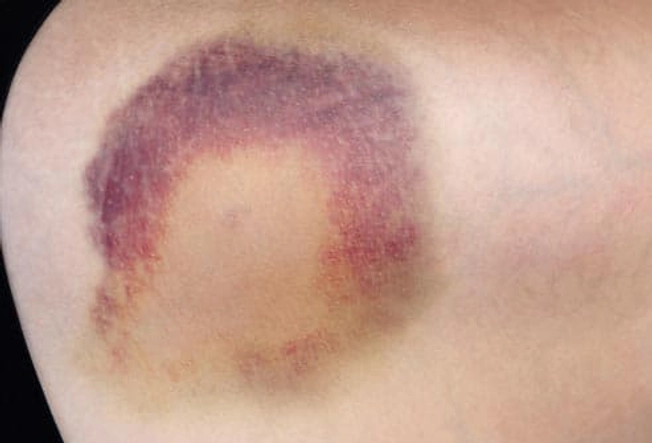
Side Effects of Blood Thinners
People who take these medications may get bruises often or bleed more easily. When you take certain ones, you'll need to watch what you eat. And you may need to go to a lab regularly to get your blood checked. Newer medications make it harder to stop bleeding if you have an accident.
Let your doctor know if you bleed a lot from minor injuries.

Internal Bleeding
Blood thinners can also make it easier to bleed inside your body, where you can't see it. Bleeding in your belly can cause pain, vomit that's red or looks like coffee grounds, and bright red or black stools. Bleeding in your brain can bring on severe headaches, vision changes, unnatural movements, and confusion. Call 911 or go to the emergency room if you notice any of these symptoms.
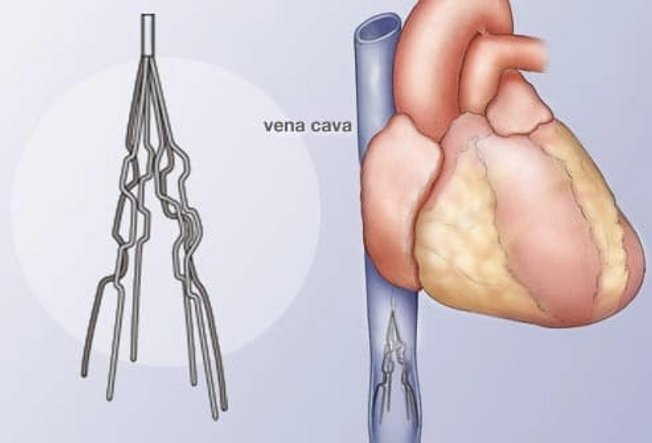
Vena Cava Filter
If you can't take blood thinners or they aren't working, your doctor may recommend putting a filter into your biggest vein, called the vena cava. This filter catches breakaway clots and stops them from getting into your lungs and heart. It won't stop new clots from forming or cure DVT, but it can help stop a dangerous pulmonary embolism.
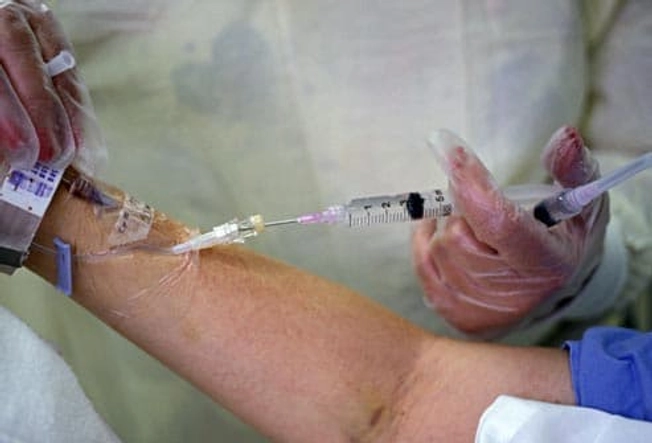
Clot Busters
Medications that dissolve blood clots are called thrombolytics. They can cause sudden, severe bleeding, so doctors use them only in emergencies -- to dissolve a life-threatening blood clot in your lung, for example. You get thrombolytics by IV in a hospital.

Compression Stockings
These special socks put gentle pressure on your legs to keep your blood moving. They help keep clots from forming as well as keep swelling down and relieve pain where a clot has formed. You can get compression stockings over the counter, but your doctor will need to write a prescription for ones with more pressure. Wear them even when you're at home.

Keep Your Feet Up
When you can, sit with your feet resting off the floor to raise your legs. You'll make it easier for the blood in your veins to flow up toward your heart. This can lessen the swelling and discomfort in the leg with DVT.

Long-Term Effects
Once a blood clot is gone, DVT sometimes leaves behind an unpleasant reminder. You may see long-term swelling or changes in skin color where the clot was. Or it could hurt. These symptoms, known as post-thrombotic syndrome, sometimes show up as much as a year after the clot.

Exercise
Use your muscles to get blood flowing. Work your lower leg muscles especially. When you're not active -- at your desk, for example -- take breaks to stretch your legs. Stand up. Step away for a bit.
Regular exercise also helps keep you at a healthy weight, and that lowers your odds of having DVT, too.

Travel Tips
When traveling will keep you seated for more than 4 hours, don't wear tight clothing, and drink plenty of water. Get up and walk around at least every couple of hours. If you have to stay in your seat, stretch and move your legs. Try clenching and releasing your calves and thighs, or lifting and lowering your heels with your toes on the floor. Do plenty of sightseeing by foot once you arrive!