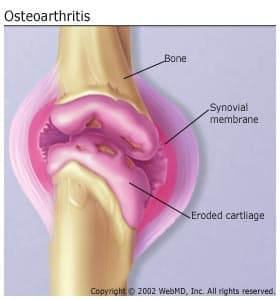
Osteoarthritis, or degenerative joint disease, is the most common type of arthritis. It is associated with the breakdown of a joint's cartilage. Cartilage is a firm, rubbery material that covers and cushions the ends of bones in normal joints. Its main function is to reduce friction in the joints and serve as a "shock absorber."
Osteoarthritis causes the cartilage in a joint to become stiff and lose its elasticity, making it more susceptible to damage. Over time, the cartilage may wear away in some areas, greatly decreasing its ability to act as a shock absorber. As the cartilage wears away, tendons and ligaments stretch, causing pain. If the condition worsens, the bones could rub against each other, causing even more pain and loss of movement.
OA is most common in middle-aged and older people, and its symptoms can range from very mild to very severe. The disorder most often affects hands and weight-bearing joints such as knees, hips, feet and the back, but can affect almost any joint in the body. Women are more commonly affected than men.
Symptoms of Osteoarthritis
Symptoms of osteoarthritis include:
- Joint aching and soreness, especially with movement
- Pain after overuse or after long periods of inactivity
- Bony enlargements in the middle and end joints of the fingers. These enlargements may or may not be painful.
What Causes Osteoarthritis?
There are many factors that can increase a person's chance of developing OA, including:
- Obesity. Maintaining an ideal weight or losing excess weight may help prevent osteoarthritis of the knees, hips, and back. Weight loss can also decrease the progression of OA.
- Injury. People with joint injuries due to sports, work-related activity, or accidents may be at increased risk of developing OA. For example, athletes with knee-related injuries may be at higher risk of developing osteoarthritis of the knee. In addition, people who have had a severe back injury may be predisposed to develop osteoarthritis of the spine. People who have had a broken bone near a joint are prone to develop osteoarthritis in that joint.
- Heredity. Some people have an inherited defect in one of the genes responsible for making cartilage. This can cause defective cartilage, which leads to more rapid deterioration of joints. People born with joint abnormalities are more likely to develop osteoarthritis, and those born with an abnormality of the spine (such as scoliosis, a curvature of the spine) are more likely to develop osteoarthritis of the spine.
- Joint Overuse. Overuse of certain joints increases the risk of developing OA. For example, people in jobs requiring repeated bending of the knee are at increased risk for developing OA of the knee.
- Age. Although age is a risk factor, research has shown that OA is not an inevitable part of aging.
Diagnosing Osteoarthritis
Doctors make a diagnosis of OA based on a physical exam and history of symptoms. The diagnosis of osteoarthritis is based on a combination of the following factors:
- A description of symptoms
- The location and pattern of pain
- Certain findings in a physical examination
X-rays may be used to confirm a diagnosis and to make sure that no other type of arthritis is present.
Sometimes, blood tests are done. While blood tests cannot point to anything in particular that can help a doctor confirm the presence of OA, the tests can help the doctor rule out a different type of arthritis.
If fluid has accumulated in the body's joints, the doctor may remove some of the fluid with a process called joint aspiration and may examine the fluid under a microscope to rule out other diseases.
Treatment Options for Osteoarthritis
The treatment of OA focuses on decreasing pain and improving joint movement. The following treatments are available:
- Over-the-counter pain-relieving and/or anti-inflammatory medications: These include acetaminophen (Tylenol, for example), aspirin, ibuprofen (Advil and Motrin), or naproxen (Aleve).
- Topical treatments. Some medications in the form of creams, rubs, or sprays may be applied to the skin of affected areas to relieve pain and inflammation.
- Exercise: Physical activity can improve joint movement and strengthen the muscles that surround the joints. Gentle exercises, such as swimming or walking on flat surfaces, are recommended because they create less stress on joints. Activities that increase joint pain (jogging, high-impact aerobics, etc.) should be avoided. If you have arthritis, talk to your doctor to find out the best exercise routine for you.
- Weight control: Losing weight can prevent extra stress on weight-bearing joints.
- Prescription anti-inflammatory pain relievers: These help reduce pain and swelling in the joints.
- Hyaluronic Acid Injections: These medications can be given as injections to relieve pain in some people with osteoarthritis. Medications include Euflexxa, Hyalgan, Orthovisc, Supartz, Synvisc, and Synvisc-One.
- Cymbalta(duloxetine): Originally approved as an antidepressant, Cymbalta is also used to fight various forms of pain, including osteoarthritis pain.
- Hot or cold compresses: These treatments may be given in the form of a hot shower or bath, or by applying heating pads or cold compresses.
- Joint protection devices: These can help prevent strain or stress on painful joints.
- Integrative therapy: Acupuncture has been shown to help relieve pain. While research is conflicting, there is some evidence that the supplement glucosamine and chondroitin may relieve some pain in some people with osteoarthritis, especially in the knee. Several studies have shown that SAMe may work better than prescription anti-inflammatory pain relievers in some people. Several other dietary supplements (including herbals) sometimes help OA pain. Check with your doctor before using these to see if they are right for you.
- Steroid injections. Your doctor can inject these potent medicines directly into your joint to help relieve pain. Using them too frequently can cause joint damage.
- Narcotics: Stronger pain pills, such as narcotics, may be prescribed when osteoarthritis pain is severe and other treatments are not working.
- Surgery: When other treatment options have failed, some people may need surgery to relieve chronic pain in damaged joints.

