1 of 5 / Acute Skin Conditions
View All
Cold Sores
Cold sores -- also called fever blisters -- are a painful infection caused by the herpes simplex virus (HSV).
Plantar Warts and Palmar Warts
Plantar warts and palmar warts are common, especially in children. These warts are named for where they appear on the body.
Blisters
A single blister is usually the result of friction or a minor burn, typically on the hands or feet.
Chafing
Chafing can occur anywhere on your body, but the thighs, groin, underarms, and nipples are particularly vulnerable.
2 of 5 / Chronic Skin Conditions
View All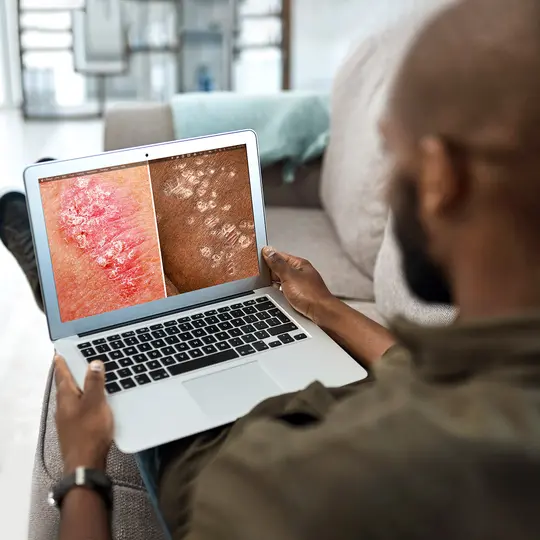
Psoriasis
Psoriasis is a common skin disorder that produces thick red plaques covered with silvery scales.
Rosacea
Rosacea is a common disorder that mainly affects skin on the face. It causes redness on the nose, chin, cheeks, and forehead.
Vitiligo
Vitiligo is a condition in which white patches develop on the skin. Any location on the body can be affected.
3 of 5 / Skin Infections
View All
Leprosy
Leprosy is caused by a slow-growing type of bacteria called Mycobacteriumleprae (M. leprae).
Carbuncles
A carbuncle is a red, swollen, and painful cluster of boils that are connected to each other under the skin.
Staph Infection
A staph infection often begins with a little cut, which gets infected with bacteria.
Cellulitis
Cellulitis is a common infection of the skin and the soft tissues underneath.
4 of 5 / Skin Discolorations
View All
Red Birthmarks, Hemangiomas, and Your Skin
Birthmarks are colored skin spots that either are present at birth or develop shortly after birth. They can be different colors.
Moles, Freckles, and Skin Tags
There are many skin lesions that are common and benign. These include moles, freckles, skin tags, and many more.
5 of 5 / Appointment Prep
View AllSuggested Reads about Skin Problems and Treatments
Elaborate Skin Care Routines Can Cause Teens More Harm Than Good
Experts say skin care is important, but teens are using too many products.
What You Eat Can Lead to Acne and Other Skin Problems
Dairy, red meat, and carbohydrates can break down into compounds that may lead to skin problems like acne, dermatitis, rosacea and other common problems.
Common Bacteria May Be Cause of Itchy Skin: Study
Scientists have a promising new theory of what causes the sensation of itching, and their latest laboratory experiments point toward potentially effective treatments for people who havem itchy skin due to eczema or dermatitis.
Biting Sand Flies Are Spreading a Skin-Scarring Parasite in U.S.
A parasitic skin disease spread by sand flies that was once only linked to international travel is no longer considered an “imported” disease in the U.S.
Top Search Terms for Skin Problems
8 million+ Physician Ratings & Reviews
Find Doctors and Dentists Near You
You can also search by physician, practice, or hospital name