- Overview
- Flares & Triggers
- Causes & Risks
- Types
- Locations on the Body
- Tests & Diagnosis
- Treatment
- Living With
- Complications
- Appointment Prep
- View Full Guide
Types of Psoriasis

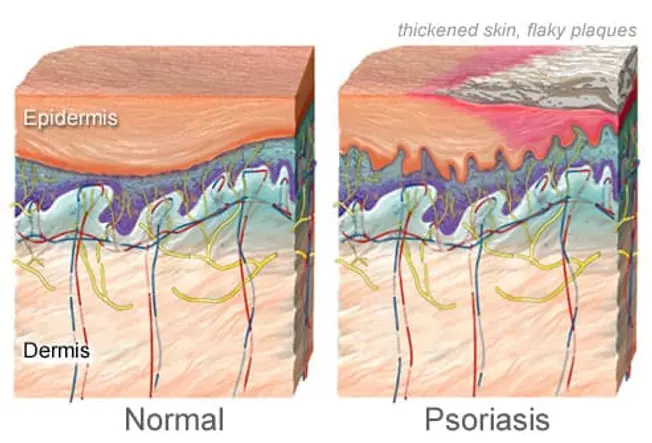
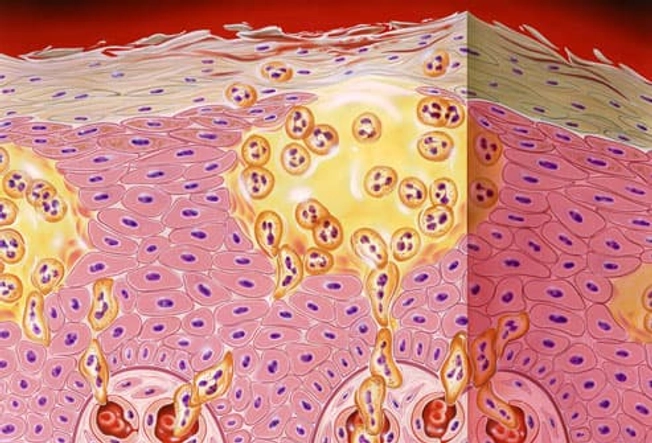
Psoriasis: Too Many Skin Cells
In psoriasis, new cells build up in the top layer of your skin. They grow faster than your body can remove, or shed, them. Blood vessels below become swollen. This causes thick, red patches, or plaques. What they look and feel like depends on what type of psoriasis you have. Doctors aren't sure what causes it. They think problems with genes and the immune system play a role.
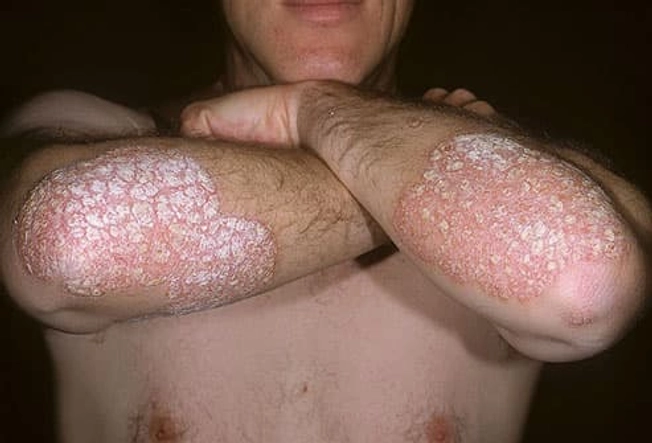
Plaque Psoriasis
This is the most common type. Patches of skin are red, raised and have silvery-white flakes, called scales. They usually show up on your scalp, elbows, knees, and lower back. They may crack and bleed and they feel sore and itchy. The more you scratch, the thicker they can get. A patch can be as wide as 4 inches; sometimes more. You can get it at any age, but it's more common in adults.
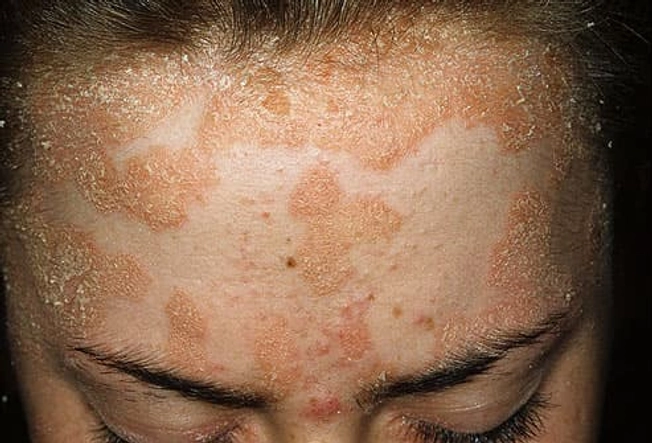
Scalp Psoriasis
About half the people with psoriasis have this type. It looks like dandruff, but it's not the same thing. Dandruff flakes are yellow and greasy. Scalp psoriasis is powdery and silver or white. Sometimes, the skin on the scalp is just a little bit crusty or flaky. This type can cover the whole head. It can also appear on your forehead, the back of your neck, and around your ears.
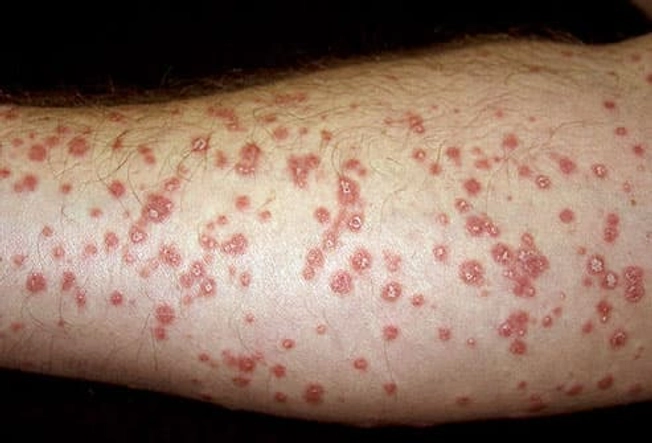
Guttate Psoriasis
Kids and young adults are more likely to get this type. Small red dots with raised edges appear suddenly, usually on the middle of your body. Other common sites are the arms, legs, scalp, ears, and face. Things that trigger this kind of psoriasis include strep throat, the flu, a cold, and other upper respiratory infections. Up to 10% of people with psoriasis has it.
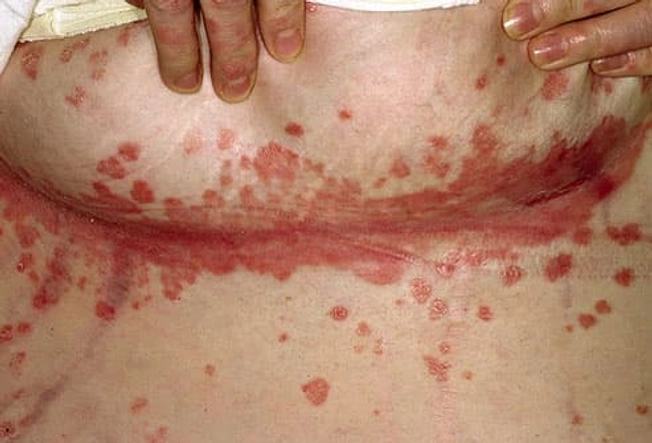
Inverse Psoriasis
These patches are shiny, bright red, and very sore. The area around them is usually smooth and doesn’t have silver scales. They appear only where skin touches skin, places called folds. Common areas are the armpits, groin, genitals, buttocks, under the breasts, and behind the knee. Rubbing and sweating can make the condition worse. Many people who have it also have another type of psoriasis.
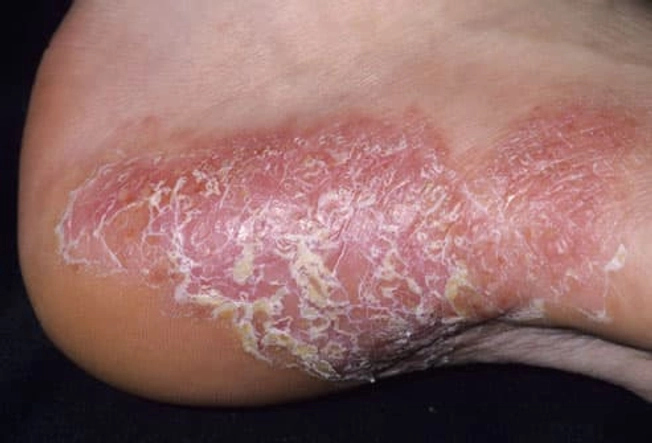
Pustular Psoriasis
This rare type might be a reaction to an infection, stress, medications, or contact with certain chemicals. It causes red, swollen patches of skin with pus-filled bumps (called pustules). When these dry out, they turn yellow-brown and scaly. The blisters may break open, leaving skin cracked and painful. They can show up anywhere on the bottom.
Pustular Psoriasis: Emergency Symptoms
This type can sometimes be life-threatening. Go to the hospital immediately if the bumps spread quickly all over your body. Other emergency symptoms are severe itching, rapid pulse, fever, muscle weakness, and chills. Doctors call this sudden form the von Zumbusch variant.
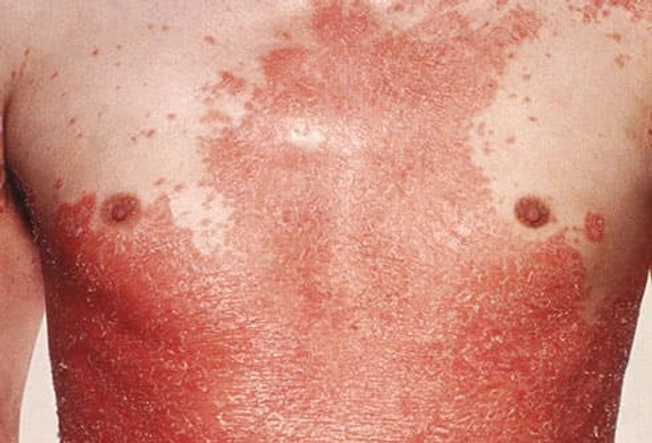
Erythrodermic, or Exfoliative
This rare form causes large areas of skin to turn bright red, like a bad sunburn, then fall off your body. Symptoms include extremely itchy and painful skin, rapid heartbeat and feeling very cold or hot. It's life-threatening, so go to the hospital. Causes include medications like corticosteroids, or untreated plaque psoriasis. It also affects people with von Zumbusch pustular psoriasis.
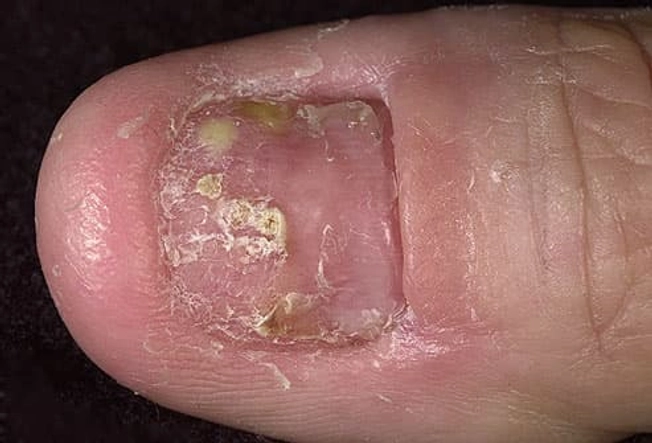
Psoriatic Nail Disease
About half of people with psoriasis also have skin cells build up under their nails, which become thick. They often split or crack. In severe cases, they could crumble or fall off. There may be brownish red or yellow spots underneath. Sometimes, the surface has tiny dents in it, like pin pricks. When they lift off the skin underneath (the nail bed), it's called onycholysis.
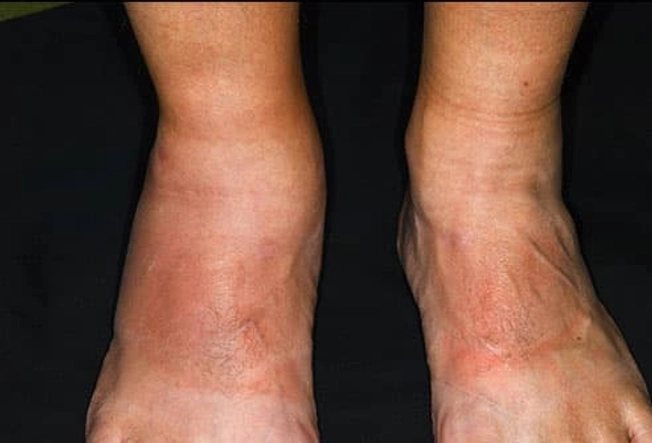
Psoriatic Arthritis
About one-third of people with psoriasis have joint pain, stiffness, and swelling. When both these problems show up, it's called psoriatic arthritis or psoriatic disease. The symptoms don't have to happen at the same time. Dry, red skin patches with silvery scales usually come first, but not always. Nail crumbling and color changes are common in people with this condition.