1 of 5 / Screening & Tests
View All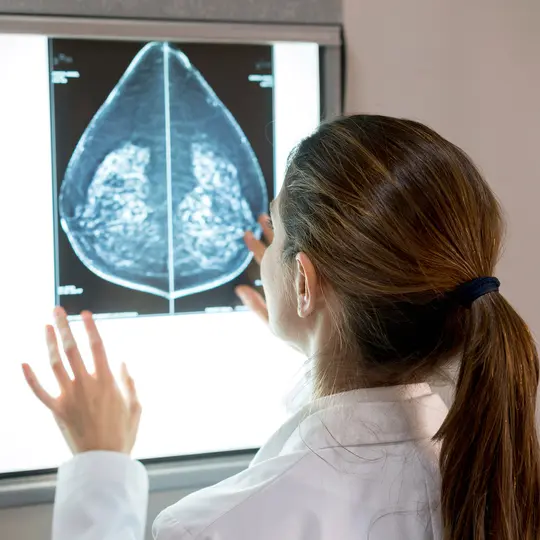
Health Checklist for Women Over 40
Keep track of tests and procedures you need after the age of 40 and take it with you to your next doctor appointment.
Testosterone and Estrogen Levels in Women
The ovaries produce both testosterone and estrogen. These sex hormones help grow, maintain, and repair reproductive tissues.
Estrogen Test
Doctors may use estrogen tests to help check on concerns with puberty, fertility, menopause, and other conditions.
Progesterone Test
A progesterone test can help your doctor check on ovulation or possible fertility problems.
2 of 5 / Diet & Exercise
View All
Healthy Eating for Weight Loss
What is a healthy diet? Get basic nutrition facts in this article.
Essential Vitamins for Women
Except for vitamin D, the human body cannot make vitamins. You need to get vitamins from the foods you eat or from supplements.
Keeping Fit After 50
If you were physically active regularly before age 50, you're at an advantage: You probably already follow these exercise tips.
Maintaining Weight Loss
This article explains why modest portions, healthy foods, and regular weigh-ins may help maintain weight loss.
3 of 5 / Rest & Relaxation
View All
Why Am I So Tired?
When it's time to see a doctor about your exhaustion -- and what to try first.
How to Beat Insomnia
Can’t sleep? Try these 10 insomnia tips.
Tips to Reduce Stress in Women Over 50
Navigating the changes of midlife causes stress, there's no doubt about it, and we'd all like to reduce stress in our lives.
Estrogen and Emotions
Differences in estrogen levels are typical in a woman on different days, or between two women on the same day of their cycles.
4 of 5 / Reproductive Health
View All
Why Do I Have Cramps but No Period?
Lots of women get pelvic pain and cramping, but your period isn't always to blame.
Your Period: 5 Things You Didn’t Know
Women have about 450 periods during their lifetimes. Even so, your period can still manage to surprise you.
Menstrual Pain
Menstrual cramps are the leading cause of absenteeism in women younger than 30 years.
Heavy Periods (Menorrhagia)
Heavy or prolonged menstrual periods, or menorrhagia, are the most common type of abnormal bleeding from the uterus.
5 of 5 / Head to Toe
View All
Thyroid Problems
Thyroid disorders can range from a small, harmless goiter (enlarged gland) that needs no treatment to life-threatening cancer.
Fatigued or Full Throttle: Is Your Thyroid to Blame?
Feeling all revved up? Or maybe your throttle's on idle with symptoms of fatigue and weight gain. The cause may be your thyroid.
Symptoms of Hypothyroidism
You might not realize you have hypothyroidism. The symptoms come on slowly, and some of them are similar to other conditions.
Hypothyroidism and Depression
Although they're two separate diseases, depression is sometimes a symptom of hypothyroidism.
Suggested Reads about Women's Health
What Are Vaginal Gummies? Debunking the Latest Health Craze
Vaginal health gummies are all the rage for their supposed ability to get your vagina in optimal shape by improving its pH balance, taste, odor, and freshness. But experts say the vagina is naturally self-cleaning.
Study: Counseling, Other Therapies Can Treat Menopause Symptoms
Therapies such as group counseling, marital support and mindfulness can treat some symptoms of menopause like anxiety and poor mood, according to a new analysis.
Women With PCOS at Higher Risk of Suicide Attempts
A PCOS diagnosis should alert doctors that their patient may need a mental health screening and referrals to further care.
Researchers Find Link Between PCOS and Midlife Cognitive Decline
A common condition called polycystic ovary syndrome that causes irregular menstrual cycles has been linked to signs of early cognitive decline.
8 million+ Physician Ratings & Reviews
Find Doctors and Dentists Near You
You can also search by physician, practice, or hospital name
