Why Breast Cancer Screening Matters
The sooner breast cancer gets diagnosed, the better your odds of getting successful treatment.
That's why it’s important to get mammograms as recommended, to be familiar with how your breasts usually look, and to report any changes to your doctor ASAP. Why?
- Breast cancer risk is up: The lifetime risk of a woman getting breast cancer in the U.S. was around 5%, or 1 in 20, in 1940. Now it’s 12%, or more than 1 in 8.
- Finding breast cancer earlier boosts your survival odds: Women who have breast cancer screening mammograms are much less likely to die from the disease. This depends on:
- The quality of the test
- Getting screened as often as you need to
- Following your treatment plan if you get diagnosed
Self-Exams, Doctor’s Clinical Breast Exams
It's a good idea to know how your breasts normally look and feel so you can notice any changes.
Medical organizations have different recommendations for breast self-exams, though. The American Cancer Society, for example, states that research has not shown a clear benefit of doing regular breast self-exams. Talk with your doctor to get a better sense of what's right for you.
Learn more about how to do a breast self-exam.
A clinical breast exam is done by your doctor, to feel for lumps or other changes. It’s part of your regular checkup. Your doctor will feel both breasts, one at a time. They’ll also check the underarm and collarbone areas. If they notice suspicious lumps, they may say you should get other tests. Your doctor will also examine the breasts visually for any rashes or anything else that looks unusual. And they may lightly squeeze your nipples to see if any fluid comes out.
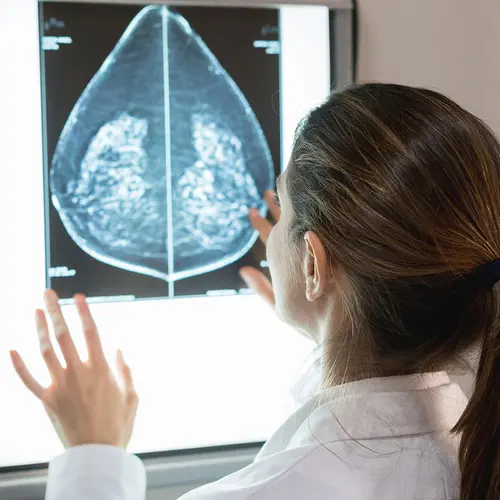
Mammograms
A mammogram is an X-ray of the breast. It can show breast lumps up to 2 years before they can be felt. Different tests help determine if a lump may be cancer. Ones that aren’t cancerous tend to have different physical features than ones that are. Imaging tests such as mammograms and ultrasounds can often see the difference.
Screening mammograms are those that are looking at your breasts when you don’t have a specific lump or other concern.
Diagnostic mammograms focus on a specific area or areas that you or your doctor is concerned about, such as where you have a suspicious lump, breast pain, discharge from a nipple, changes in size or shape of the breasts, or certain skin changes on the breast.
When and if you need screening mammograms is a personal decision between you and your doctor. Most women don’t start having screening mammograms until they’re at least 40. If you’re at higher risk for breast cancer, your doctor may want you to start at a younger age.
Read about how digital mammograms can give a clearer picture.
Breast MRI
This test combines several images of your breast into one to create a detailed picture. It’s more often used after you’re diagnosed to see how far cancer has spread, but your doctor might combine it with a mammogram as a screening test if:
- You’re at a high risk for breast cancer.
- You have a family history of breast or ovarian cancer.
- Your breasts are dense (there are a lot of ducts, glands, and fibrous tissue, but little fat) and mammograms didn't find a previous breast cancer.
- You have dense breasts, a strong family history of breast cancer, and you’ve had precancerous breast changes like atypical hyperplasia or lobular carcinoma in situ.
- You have the BRCA1 or BRCA2 gene mutation.
- You had radiation treatments to your chest area before you were 30.
Know more about MRI to diagnose breast cancer.
Breast Ultrasound
Your doctor is most likely to use this if you have dense breasts. It’s also an option if you’re at high risk for breast cancer and you can’t have an MRI or if you’re pregnant so you aren’t exposed to X-rays from a mammogram.
Get more details on what happens during a breast ultrasound.
Screening Recommendations
For women at average risk, the American Cancer Society recommends that women ages:
- 45 to 54: Get yearly mammograms
- 55 and older: Can switch to getting a mammogram every other year or continue getting yearly mammograms
- 40 to 44: It’s OK to start a yearly mammogram.
The U.S. Preventive Services Task Force recommends screening mammograms every other year for women ages 50-74. The decision to get a mammogram every other year from age 40 to 49 is up to you and your doctor.
How Do Doctors Diagnose Breast Cancer?
The only way to confirm cancer is for a doctor to do a needle aspiration or surgical breast biopsy to collect and test tissue for cancer cells.
Find out what to expect with a breast biopsy.
If It’s Cancer
If you’re diagnosed with breast cancer, you and your doctor will need to know what type it is and how advanced it is. A check of your lymph nodes can tell if the disease has spread. Other tests give an idea of what treatments may work best for you, and still others predict how likely it is that your cancer will come back after treatment.
Your doctor can help you understand all of these tests, and together you’ll decide on the best treatment plan for you.
Get more information on what to do after a breast cancer diagnosis.