What Is Frostbite?
Frostbite refers to the freezing of body tissue (usually skin) that results when the blood vessels contract, reducing blood flow and oxygen to the affected body parts.
Normal sensation is lost, and these tissues change color.
Frostbite is most likely to affect body parts that are farther away from the body core and, therefore, have less blood flow. These include your feet, toes, hands, fingers, nose, and ears.
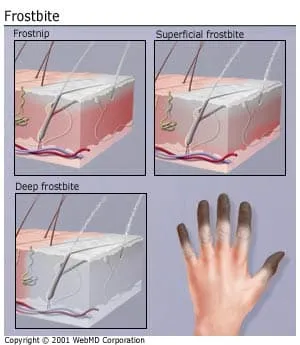
There are three degrees of cold injury: frostnip, superficial frostbite, and deep frostbite. Although children, older people, and those with circulatory problems are at greater risk for frostbite, most cases happen in adults between 30 and 49.
If you develop frostbite, you may not realize at first that anything is wrong, because the affected area may be numb. With prompt medical attention, most people recover fully from frostbite. However, if severe frostbite happens, permanent damage is possible depending on how long and how deeply the tissue was frozen. In severe cases, blood flow to the area may stop, and blood vessels, muscles, nerves, tendons, and bones may be permanently damaged. If the frozen tissue dies, the affected area may need to be amputated.
What Causes Frostbite?
Frostbite is usually caused by long exposure to cold temperatures, particularly if they are accompanied by a low wind-chill factor. It may also happen following more brief exposure to very cold temperatures.
What Are the Symptoms of Frostbite?
For frostnip:
- White patches of skin that are numb.
For frostbite (superficial or deep):
- Skin that is white or grayish-yellow and feels hard, waxy, or numb, or is blistering or becoming darkened or black.
- Other symptoms include swelling, itching, burning, and deep pain during the rewarming/healing process.
How Is Frostbite Diagnosed?
Frostbite is initially diagnosed based on symptoms and a physical exam.
Three to 5 days after rewarming, doctors will use imaging tests to determine how badly the tissue is damaged.
After 1 to 3 weeks, imaging will help find any damaged tissue or blood vessels and identify areas that may need to be amputated.
What Are the Treatments for Frostbite?
Most people recover completely from frostbite, though the affected area may be more sensitive to cold and sun damage and more likely to get frostbitten again. The first goal of treatment is to rewarm the affected area.
Frostnip can be treated at home.
- If you think you may have frostnip, get out of the cold as soon as possible.
- If your clothes are wet, change into dry clothing.
- Soak the affected area in warm water (100 to 105 F) to thaw the frozen tissue. Don’t use hotter water because it may burn your skin.
- If warm water isn’t available, use your own body heat by, for instance, tucking your hands into your armpits or covering your nose, ears, or face with dry hands.
CAUTION: Don’t rub the affected area because this may increase damage to the tissue. Don’t use a heating pad, heat lamp, stove, fireplace, or radiator to rewarm the affected area. These methods may warm your skin unevenly or may burn your skin, particularly if it’s numb and you can’t tell how hot it’s getting.
If the skin tingles and burns as it warms, your circulation is returning. The skin may turn red, but shouldn’t blister or swell. If the skin doesn’t seem to warm, if it remains numb, or if it does blister or swell, seek immediate medical attention.
Frostbite requires emergency medical care.
- If you think you may have frostbite, get out of the cold as soon as possible.
- If you can’t get medical help immediately and there's no risk that the area might be refrozen before you get help, warm the affected area as you would for frostnip.
CAUTION: If the affected area might be refrozen before you get medical help, don’t warm it; this greatly increases the risk of damage. Also, don’t walk on frostbitten feet or toes unless it's absolutely necessary.
At the hospital, frostbite is usually treated comprehensively because you can’t tell how bad it is in the first few days. Usually, patients need to be admitted for observation. Initially, the hospital staff will probably do the following:
- Rapidly warm the affected area in water for 15 to 30 minutes.
- Remove blisters that contain clear or milky fluid and cover them with a topical antibiotic, petroleum jelly, or aloe vera gel. Blisters that contain blood may not be removed.
- Splint and elevate the affected area and wrap it in a loose bandage.
- Administer ibuprofen to limit inflammation, tetanus toxoid to prevent tetanus infection, and antibiotics to prevent or treat infection. Narcotic drugs may be needed to treat pain as sensation returns.
Later hospital treatment may include whirlpool therapy and physical therapy to promote circulation. Surgery, including amputation of the affected area, is sometimes necessary if the tissues are dead. That’s typically decided between 3 and 6 weeks after the injury.
How Is Frostbite Prevented?
The only way to prevent frostbite is to limit the amount of time you spend outdoors in extremely cold weather. But if you do go out, dressing right is a must:
- Layer up. Wear a synthetic fabric next to your skin. Cover that with a fleece and wool layer. Flowy layers keep warm air in, close to your body. Top it off with outerwear that wards off wind and water.
- Tuck in your toes. You’ll need two pairs of socks -- a synthetic pair underneath to wick moisture from your skin, topped by a pair made of wool or wool-blend. Foot warmers can work well, too. Make sure your footwear is waterproof and covers your ankles to keep snow and dampness out.
- Don’t forget your fingers. Mittens are your best bet to protect your digits from frostbite. If you prefer gloves, choose a cozy pair and try moisture-wicking glove liners under them.
- Heading out. A hat or headband made of fleece, heavy wool, or windproofing fabric is your best choice. Make sure it covers your ears. Add a face mask or scarf if the cold is extreme. It’ll protect your face and nose. It’ll warm the air you breathe in, too.
You have a greater chance of getting frostbite if your clothes and footwear get wet. Make sure your layers stay dry.
Here are some other frostbite prevention tips:
- H2O to go. Drink lots of water. Down at least a whole glass and eat a good meal before you venture out. Avoid alcohol. It makes you lose heat more quickly.
- Mind the clime. Trust your weather forecast, and note those wind-chill readings. Frostbite can attack exposed skin within minutes. Take along emergency supplies in case you can’t get back as quickly as you plan.
- Check in with friends. It’s best to be prepared, whether or not you think you’ll need help. Let people know where you’re headed and when you’ll be back.
- Keep it moving. Staying in motion while you’re out keeps your blood flow up and helps you stay warm. Don’t overdo it, though. You’ll need your energy in the cold.
