Parkinson's disease is a chronic progressive neurological disease that affects a small area of nerve cells (neurons) in an area of the brain known as the substantia nigra. These cells normally produce dopamine, a chemical (neurotransmitter) that transmits signals between areas in the brain that, when working normally, coordinate smooth and balanced muscle movement. Parkinson's disease causes these nerve cells to die, and as a result, body movements are affected.
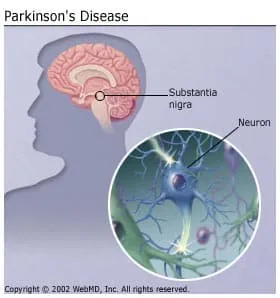
"Parkinsonism" is a term that is often used interchangeably with Parkinson's disease. Medically, parkinsonism refers to any condition that causes symptoms similar to Parkinson's disease tremors at rest, muscle rigidity, slow movement, and changes in walking. Parkinson's disease is probably the most common form of parkinsonism. Other conditions that cause it include:
- Medications such as reserpine, Thorazine
- Toxic exposures to carbon monoxide, cyanide
- Hypothyroidism
- Hypoparathyroidism
- A variety of other neurologic conditions affecting the nerves in the substantia nigra such as Wilson's disease (a condition causing abnormal deposition of copper in the brain) and progressive supranuclear palsy
Learn more about other causes of Parkinson's.
What Are the Symptoms of Parkinson's Disease?
Common symptoms of Parkinson's disease include:
- Muscle rigidity
- Tremors
- Bradykinesia (the slowing down of movement and the gradual loss of spontaneous activity)
- Changes in walking pattern and posture
- Changes in speech and handwriting
- Loss of balance and increased falls
- Orthostatic hypotension (a drop in blood pressure when standing, resulting in lightheadedness or fainting)
Who Gets Parkinson's Disease?
Approximately one million Americans have Parkinson's disease, including three out of every 100 people over the age of 60. Over 50,000 Americans are diagnosed with Parkinson's disease each year. There is increasing evidence that Parkinson's disease may be inherited (genetically passed on between family members). Men are slightly more likely to develop the disease than women.
The average age at which it is diagnosed is 60. However, about 4% of those with Parkinson's disease are diagnosed before age 50, and about half of those are diagnosed before age 40. When the diagnosis is made early, it is referred to as "young-onset" Parkinson's disease.
Young-Onset Parkinson's Disease
While the disease presents in much the same way among people in the older age groups, people with young-onset Parkinson's disease will have special concerns because they will be dealing with the disease at a younger age and for a potentially longer period. Potential changes needed may involve making career adjustments and family concerns.
However, there is good news for people with young-onset Parkinson's disease. Young-onset Parkinson's disease is different from older onset Parkinson's disease. In general, younger people have a smoother, longer-term course of the illness. While this may, in part, be a reflection that the younger people have fewer other health problems than older people with the disease; the rate of progression is still significantly slower. Associated problems, such as memory loss, confusion, and balance difficulties, are also less frequent in young people with the disease.
On the other hand, people with young-onset Parkinson's disease often have more movement problems due to the most commonly prescribed medication, levodopa, than older people with the disease. For this reason, young-onset patients are often treated with alternatives to levodopa.
Young-onset patients are also better candidates for many of the new surgical procedures and medical innovations that are used to treat and reduce the symptoms of Parkinson's disease.
Is There a Cure for Parkinson's Disease?
Although research is ongoing, to date there is no known cure or way to prevent Parkinson's disease. But, research has made remarkable progress. There is very real hope that the causes, whether genetic or environmental, will be identified and the precise effects of these causes on brain function will be understood. These remarkable achievements give real hope for the future.
Still, even though there is no cure for Parkinson's disease, by identifying individual symptoms and determining a proper course of treatment, most people with the disease can live enjoyable, fulfilling lives.