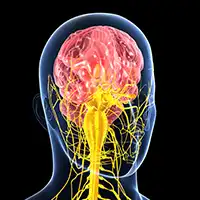
Understanding Hereditary Transthyretin Amyloidosis With Polyneuropathy
The protein transthyretin can change shape and clump together. Drugs for hATTR with polyneuropathy target this troublemaker.
You can also search by physician, practice, or hospital name