Stages and Treatments for Diffuse Large B-Cell Lymphoma

Staging Diffuse Large B-Cell Lymphoma
After doctors diagnose diffuse large B-cell lymphoma (DLBCL), they’ll do more tests to find out where the cancer is in your body and how far it has spread. This process is called staging. You might get these tests:
- Physical exam
- Blood tests
- Bone marrow biopsy
- Imaging tests
These test results and the stage of the cancer help doctors to decide the best way to treat your cancer.
Understand Your Stage
Doctors divide DLBCL into four stages. Here’s what they mean:
- Stage I: The cancer is in one lymph node area, lymph structure, or other site.
- Stage II: The cancer is in two or more lymph node areas or structures on one side of the diaphragm, the large muscle that separates the belly from the chest.
- Stage III: The cancer is in lymph node areas or structures on both sides of the diaphragm.
- Stage IV: The cancer has spread to other organs and tissues. This may include the liver, lungs, or bone marrow.
Staging and Treatment
It’s best when the cancer is in an earlier stage. But the stage can’t tell you how well your treatment will work or what the future will hold. Your doctor will use the stage along with other things like your general health and age to set your treatment plan. Treatment for DLBCL may include:
- Chemotherapy
- Immunotherapy
- Steroids
- Radiation therapy
- Targeted therapy
- Stem cell transplant
- CAR T-cell therapy

Treating Advanced DLBCL
The most common treatment for advanced DLBCL is called R-CHOP. This treatment combines three chemotherapy drugs with an antibody and a steroid. They are:
- Rituximab (Rituxan)
- Cyclophosphamide (Cytoxan)
- Hydroxydaunorubicin (Doxorubicin)
- Vincristine (Oncovin)
- Prednisone
Doctors often give R-CHOP every 3 weeks for six to eight cycles. Most people will have side effects, which may include fever, low blood counts, and nausea. For people with certain health conditions, doctors may recommend other treatment combinations.
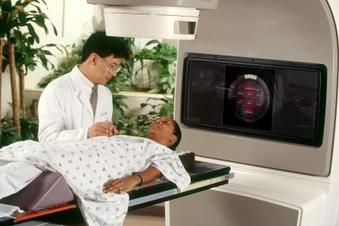
Treating Early-Stage DLBCL
Doctors also use R-CHOP to treat early-stage DLBCL. They may use fewer cycles – four instead of six or eight – together with radiation therapy. Doctors most often give radiation therapy five times a week over 3 or 4 weeks. Immediate side effects of radiation may include tiredness, skin changes or pain, and hair loss.

Measuring Treatment Response
Several weeks after treatment ends, you’ll go through another round of tests. These tests will find out how well the treatment worked. If doctors find no sign of cancer with a physical exam, imaging tests, or bone marrow biopsy, it’s called a complete response. Your doctor will continue to monitor you to make sure the cancer doesn’t come back. Most relapses happen in the first 2 years after treatment.
When Cancer Comes Back
If the cancer didn’t go away completely or comes back, you’ll likely have more treatment options. They may include chemotherapy. But there are also several treatments approved for people with DLBCL that has come back after two or more treatments. These include:
- Axicabtagene ciloleucel (Yescarta)
- Lisocabtagene maraleucel (Breyanzi)
- Pembrolizumab (Keytruda)
- Polatuzumab vedotin-piiq (Polivy)
- Selinexor (Xpovio)
- Tisagenlecleucel (Kymriah)
Exploring New Treatment Options
These newer treatment options for relapsed DLBCL include immunotherapies that work to unleash the immune system against cancer. They also include an approach called CAR T-cell therapy. In CAR T, doctors modify a patient’s cells to fight cancer, grow them in the lab, and put them back in large numbers.

Blood Stem Cell Transplant
When cancer comes back, a bone marrow transplant or blood stem cell transplant may be an option. Doctors can use your own cells or donor cells. Before receiving the healthy cells, you’ll receive high doses of chemotherapy to knock out any cancer cells and make room for the healthy cells. The transplanted cells reach the bone marrow and new, healthy blood cells are made after a couple of weeks. Sometimes this may be the best option to get rid of the cancer, but it also can have severe side effects.

Consider a Clinical Trial
Especially if approved treatments don’t work, ask your doctor if there’s a clinical trial you could join. Clinical trials test new treatments and new treatment combinations to see if they are safe and effective. Trials can help to expand your treatment options and get access to the newest treatments. But you need to know what the risks are and exactly what’s involved. Ask your doctor to help you with that.

Weighing Your Options
Always feel free to ask your doctor questions about your cancer and treatment options. In some cases, it may be hard to decide what to do. It’s often possible to take some time to think about it. You may want to consider having another doctor review your records for a second opinion before you start treatment. Talking to people who have been through this before or are in the same situation, either online or in a support group, also may be helpful.
Show Sources
Photo Credits:
1) Jovanmandic / Getty Images
2) didesign021 / Getty Images
3) PHILIPPE PLAILLY / Science Source
4) katleho Seisa / Getty Images
5) Will & Deni McIntyre / Science Source
6) Kwangmoozaa / Getty Images
7) Chainarong Prasertthai / Getty Images
8) STEVE GSCHMEISSNER / Science Source
9) Jose Oto / Science Source
10) stockstudioX / Getty Images
11) SDI Productions / Getty Images
SOURCES:
UpToDate: "Patient education: Diffuse large B cell lymphoma in adults (Beyond the Basics)."
National Comprehensive Cancer Network: “Guidelines for Patients: Diffuse Large B-Cell Lymphoma.”
Lymphoma Research Foundation: “Diffuse Large B-Cell Lymphoma: FDA Updates.”
American Journal of Hematology: "2021 Update on Diffuse large B cell lymphoma: A review of current data and potential applications on risk stratification and management."