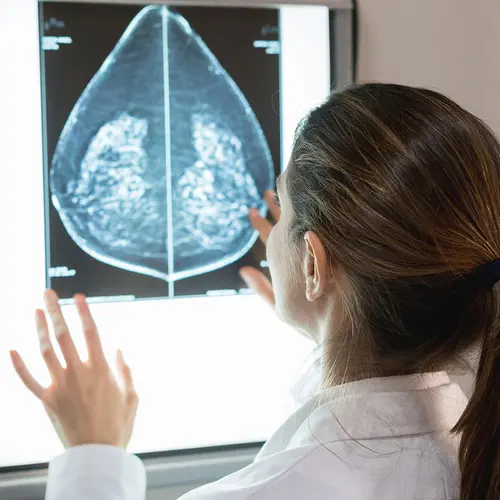
How Can I Prevent Breast Cancer?
Doctors still are not certain how to prevent breast cancer.
Regular aerobic exercise may offer some protection. Studies have found that women who exercised vigorously and often were half as likely as non-exercisers to get breast cancer. This has been demonstrated primarily in younger, pre-menopausal women. Exercise also can help women with breast cancer better tolerate the side effects of treatment and recover faster after surgery. It can also have a better impact on survival.
Nutrition and Diet to Prevent Breast Cancer
Diet plays a very small but measurable role in breast cancer prevention. Dietary fats may increase your risk of developing breast cancer, and fruits, vegetables, and grains may help to reduce the risk. This has been seen in countries other than the United States. In the U.S., low-fat diets have not been seen to reduce breast cancer risk.
Alcohol consumption has been associated with an increased risk of breast cancer. So does smoking. Women who drink two and a third to four and a half bottles of beer per day, two and a half to more than five and a half glasses of wine per day, or two to four shots of liquor per day, have a 41% increased incidence of breast cancer. So the recommendation is to limit alcohol consumption.
It's important to keep in mind that dietary measures are not proven to overcome other risk factors for breast cancer. Women who adhere to a healthy diet should still take other preventive measures such as having regular mammograms.
Early detection and treatment is still the best strategy for a better cancer outcome. The following is a common strategy, but ask your doctor exactly what you should do to help prevent breast cancer or find it early:
- Have a medical checkup and mammogram on a regular basis. The American Cancer Society recommends women ages 40 to 44 should have a choice to start yearly screening mammograms if they would like. Women ages 45 to 54 should have a mammogram each year, and those 55 years and over should continue getting mammograms every 1 to 2 years. The U.S. Preventive Services Task Force recommends every-other-year mammograms beginning at age 40 through age 74. Talk to your doctor about when you should have your first mammogram.
- If you use contraception, ask your doctor about the pros and cons of birth control pills.
- If you are near or in menopause, ask your doctor if you should use hormone replacement therapy to treat menopause symptoms. Studies suggest that hormone replacement, especially therapies with a combination of estrogens and progestins, can increase the risk of breast cancer. You and your doctor can make this decision based on your risk of breast cancer.
- If you are at high risk for breast cancer, certain drugs that block the effects of estrogen, such as raloxifene and tamoxifen, have been shown to reduce the risk of breast cancer. Drugs called aromatase inhibitors, including anastrozole (Arimidex) and exemestane (Aromasin), have also been shown to lower breast cancer risk in post-menopausal women. The risks and benefits of using these medications should be discussed with your doctor.