Slideshow: A Visual Guide to Postpartum Depression


What Is Postpartum Depression?
Postpartum depression is a treatable medical illness that affects as many as 1 in 5 women after giving birth. It can develop anywhere from a few weeks to a year after delivery, but it's most common in the first three months postpartum. Postpartum depression can be hard to spot, because the moodiness and other symptoms are similar to the "baby blues" -- a short-lived state that affects up to 80% of new mothers, according to the NIH.

Symptom: Depressed Mood
It's normal to feel emotional when you've just had a baby. Hormone shifts, lack of sleep, and adjusting to life with a newborn can seem overwhelming. But if you've been feeling sad, moody, guilty, or hopeless for more than a couple of weeks, it could be postpartum depression. Some women also report that they don't feel any joy or excitement about their new baby, and they get no pleasure from things they once enjoyed.

Symptom: Sleep Problems
Tending to a newborn disturbs every new mother's sleep, but postpartum depression can cause larger sleep issues. It may be hard to sleep when you get the chance. Or you may sleep too much. Not getting enough sleep can turn into a vicious cycle -- poor sleep can contribute to depression, and then depression can interfere with sleep.

Symptom: Appetite Changes
A common symptom of depression is eating less or more than usual. While some women turn to food for comfort when they're depressed, others lose interest in it completely. Good nutrition is especially important if you're breastfeeding, and nursing a baby does make you more hungry than usual. But if your appetite changes dramatically -- up or down -- and you feel sad or overwhelmed, talk to your doctor about it.
Symptom: Anxiety
Not all women experience anxiety as a symptom of postpartum depression, but some do. You may feel nervous, frightened, restless, or stressed. Some women have intense worry about their baby's health or safety. If you constantly feel overwhelmed by the responsibility of caring for your newborn, or if nerves interfere with your ability to handle everyday tasks, it could be a sign of postpartum depression.

Symptom: Frequent Ups and Downs
Mood swings are a normal part of life after a baby arrives, especially in the first two weeks after delivery. Don't be surprised if you find yourself laughing one minute and crying the next. But if these emotional highs and lows continue for more than two weeks or start to get worse, they may be a sign of postpartum depression.

Depression or Baby Blues?
What sets postpartum depression apart is how long it lasts and severity of symptoms. The baby blues -- having mood swings, feeling sad or anxious, crying for no reason -- usually goes away on its own after 1 to 2 weeks. If your symptoms persist or get worse over time, you should seek help. In some cases, postpartum depression can start one to two months after childbirth, with strong feelings of depression or thoughts of hurting yourself or your baby.

When to Seek Help
Call your doctor if:
- Baby blues last longer than two weeks
- Your symptoms get worse
- You're having trouble caring for yourself or your baby
- You're having thoughts of harming yourself or your baby
If you are thinking about hurting yourself, call the national suicide hotline at 1-800-273-TALK.
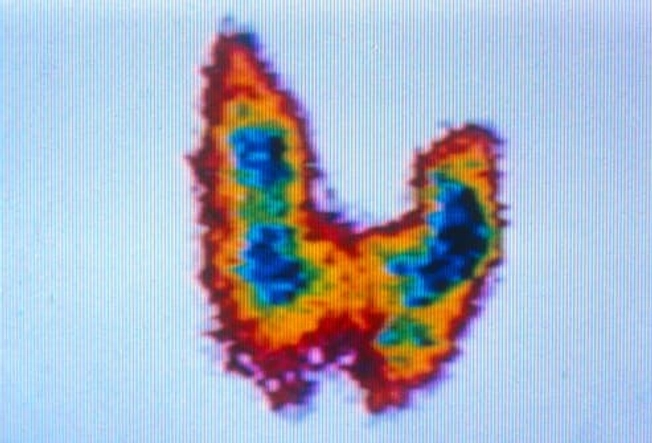
Depression or Thyroid Disorder?
In some women, the butterfly-shaped thyroid gland becomes temporarily underactive during the postpartum period. Symptoms of an underactive thyroid (hypothyroidism) include depression, fatigue, weight gain, dry skin, forgetfulness, and constipation. If you notice any of these symptoms, have your doctor do a blood test to check your hormone levels. If it's an underactive thyroid, medications can help.
What Causes Postpartum Depression?
No one knows for sure why some women get postpartum depression and others don't. The sharp drop in the hormones estrogen and progesterone after childbirth may trigger the illness, and lack of sleep can contribute as well. Some women feel conflicted about their changing identity and new responsibilities, and this can factor in. If you've had depression in the past, you're more likely to develop postpartum depression.
What Is Postpartum Psychosis?
Postpartum psychosis is a rare, serious mental illness. It's more common in women with a personal or family history of bipolar disorder or schizophrenia. Symptoms include irritability, restlessness, rapidly changing moods, confusion, erratic behavior, and delusional thoughts. A woman with postpartum psychosis is at risk of harming themselves or their baby, so it's important to seek help right away if a new mother is experiencing any of these symptoms.
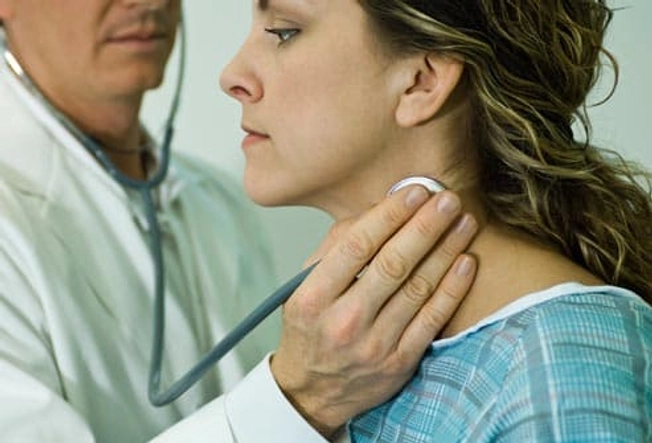
How Is PPD Diagnosed?
If you're having trouble coping with all the changes that new motherhood brings, see your doctor. They can determine if you're experiencing postpartum depression or refer you to a mental health professional. Many new mothers feel embarrassed or ashamed and keep it to themselves, but having postpartum depression doesn't make you a bad mother. Help is available, and there's no reason to suffer.

PPD Treatment: Therapy
Many women with postpartum depression find relief through talk therapy. A therapist is there to listen and give you strategies to cope with the negative thoughts and feelings you're having. One type, called cognitive behavioral therapy (CBT), has been tested and compared with the use of an antidepressant medicine. A short course of CBT worked as well as medicine in easing symptoms of postpartum depression.
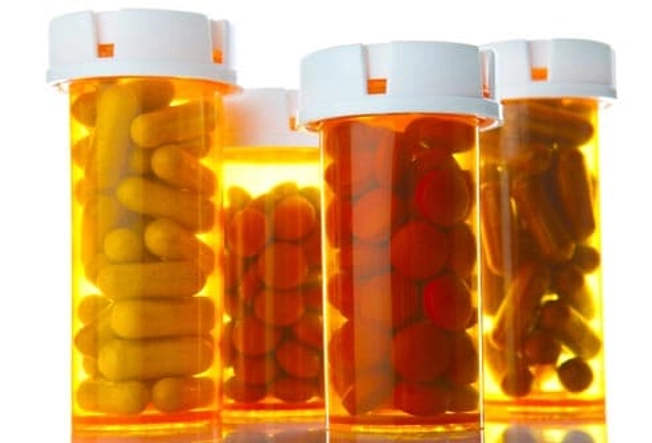
PPD Treatment: Medicine
Your doctor may recommend one of the antidepressant drugs to help lift postpartum depression. These drugs can be very effective, but they don't work overnight, and they may have unwanted side effects or react badly with other medications you may be taking. Ask your doctor how long it will take before you feel better, what side effects you might experience, how long you'll need to take the medication, and how to taper off when you're ready. For severe cases, the drug brexanolone (Zulresso) has been shown to bring dramatic and almost immediate improvement in postpartum depression. It is administered via infusion over a course of 3 days.
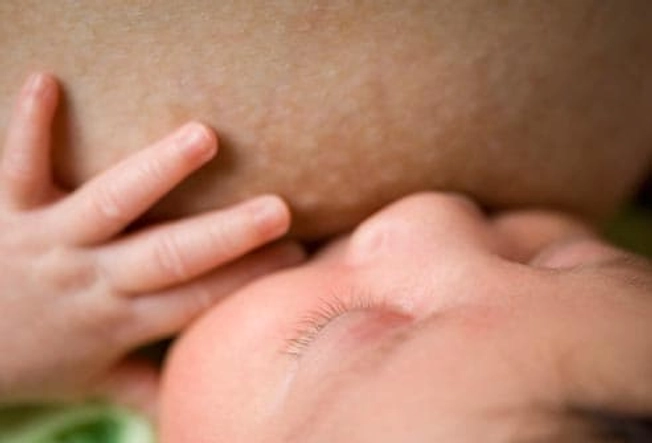
Antidepressants and Breastfeeding
If you're breastfeeding, it's important to know that antidepressants can be passed to your baby through your breast milk. Although this is shown to be safe for many drugs, it's best to talk to your doctor if you have safety concerns. Postpartum depression itself poses risks to an infant, if a new mom goes without needed treatment.

Complications
Swift action to lift postpartum depression is important for a healthy mother and child. Without treatment, depression can last for many months and may have long-term consequences for you and your baby. Research suggests that postpartum depression can interfere with bonding between mother and child, which can lead to behavior problems and developmental delays when your child gets older.

Tips to Feel Better
If you're feeling depressed, the following strategies may help you feel better.
- Accept help from family and friends.
- Rest when you can.
- Spend time with other new mothers who can relate to what you're going through.
- Hire a babysitter and take time for yourself.

Diet and Exercise Can Help
Make an effort to get a little exercise every day. Even something as simple as pushing the stroller around the block can improve your mood. Eating a healthy, balanced diet, and drinking plenty of water can also help you start to feel more like yourself again. Another benefit of eating right and exercising: You'll get your pre-baby body back quicker, and that will give your self-esteem a boost.

Note to Family Members
Lack of support is a major factor in postpartum depression. There are several ways family members can help.
- Check in regularly to see how they're doing.
- Make their a nutritious meal.
- Watch the baby so they can nap or take a shower.
- Help out with housework.

Outlook
When you're depressed, it can feel like things will never get better. Adjusting to new motherhood is one of the biggest challenges a woman will face in their life -- it's normal to feel overwhelmed. But with the right help, you can feel better. Without the cloud of depression hanging over your head, you'll be able to enjoy your new baby and take the challenges in stride.