- Overview
- Symptoms
- Causes & Risks
- Types of Eczema
- Locations on the Body
- Tests & Diagnosis
- Treatment
- Complications
- Living With
- View Full Guide
A Visual Guide to Eczema

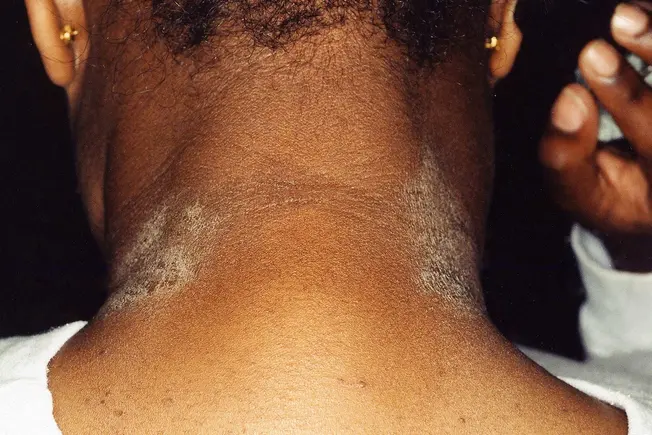
What Is Eczema?
It’s sometimes called "the itch that rashes," because the itching usually comes first. This group of skin rashes is very common in babies and toddlers. Adults can have it too, often as scaly, leathery patches or on their hands. Atopic dermatitis is a common, often inherited form of eczema, but there are other types and many treatments.
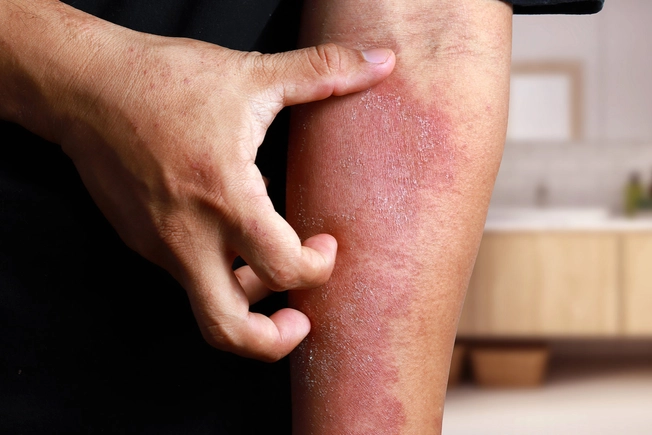
Symptoms
Itching is the main one. Scratching makes your skin inflamed and itchier, and it can look different. You may notice:
- Affected areas may be red (light skin) or darker brown, purple, or ash gray (brown skin).
- Dry, scaly areas
- Warmth, possibly also with some swelling
- Small, rough bumps
- Thick leathery patches
- Bumps that leak and crust over
- After healing, the affected area might look lighter or darker than the rest of your skin.

Eczema in Babies
Infants who are 6-12 weeks old can get atopic dermatitis as a patchy facial rash. Moisture from drooling makes it worse. In some cases, the condition goes away by age 2. But about half of people who had atopic dermatitis as a child will have it as an adult.
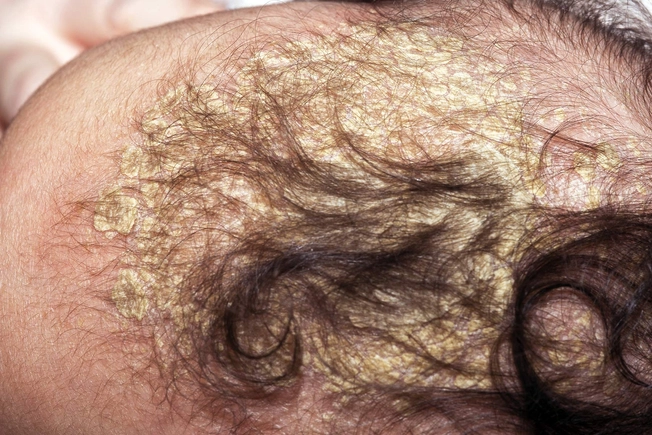
Is It Cradle Cap?
"Cradle cap" in babies is a condition that doctors call seborrheic eczema or seborrheic dermatitis. It appears as oily, scaly patches on the scalp. In contrast, atopic dermatitis is more often found on the cheeks, though it can also affect the scalp. Also unlike eczema, cradle cap typically isn’t itchy. Usually cradle cap clears up without treatment in a few weeks or months.
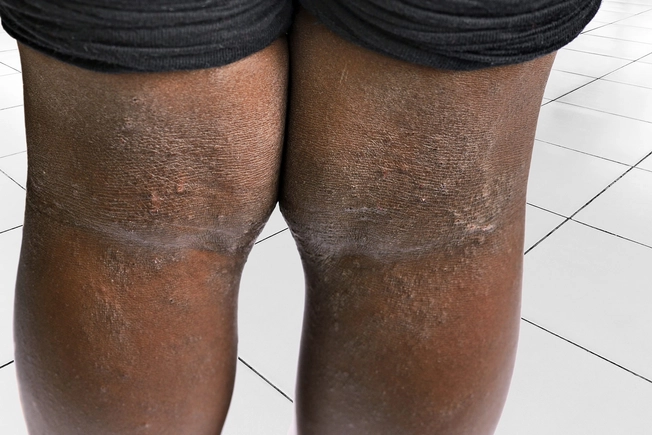
Eczema in Children
Kids can get eczema in a lot of different places: the inside of their elbows, behind the knees, on the face, on the back of their necks, or on wrists and forearms. You can’t “catch” eczema -- it’s not contagious.
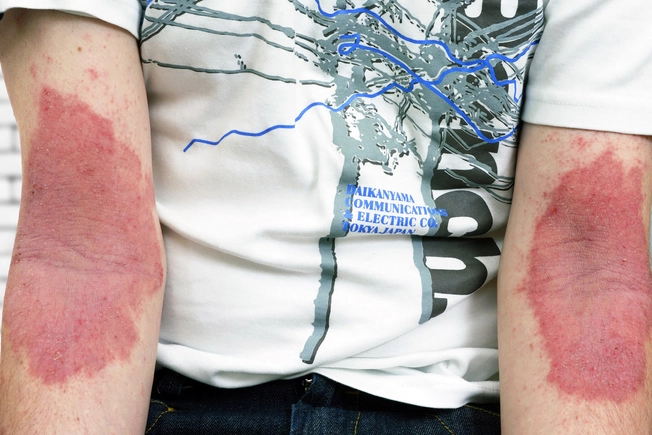
When Adults Get It
You might notice itchy patches on the hands, elbows, and in the "bending" areas of the body, such as the inside of the elbows and back of the knees. But eczema can appear anywhere, including the neck, chest, and eyelids. People who had atopic dermatitis as a child may see drier, scaly rashes as adults. The skin may be discolored or thickened.

Diagnosis
If a rash won’t go away, is uncomfortable, or gets a crust or pus-filled blister, see your doctor. They will check your medical history, symptoms, and ask you about any allergies that run in your family. You may also get allergy tests or a microscopic exam of a skin scraping (seen here) to rule out infections.

Link to Hay Fever, Asthma
There's a connection between those two conditions and atopic dermatitis. If a parent has hay fever or asthma, their children are more likely to have the skin condition. And many children with atopic dermatitis will go on to get hay fever and/or asthma.

Eczema and Allergies
Triggers that bring on an allergy attack -- such as pollen, animal dander, and dust mites -- can cause some people with atopic dermatitis to break out in a rash. These allergens cause the immune system to overreact, leading to skin inflammation.

Other Triggers
Irritants can cause inflammation and itching, bringing on eczema. Harsh chemicals can cause a rash in anyone, but people with eczema may be sensitive to mild irritants, such as wool and synthetic fabrics, detergents, soaps, perfumes, and cosmetics. Stress or anxiety can cause a flare-up, too. So can sweating, along with wetting and drying your skin a lot, such as when you wash your hands. Cold, dry environments can also cause a flare.
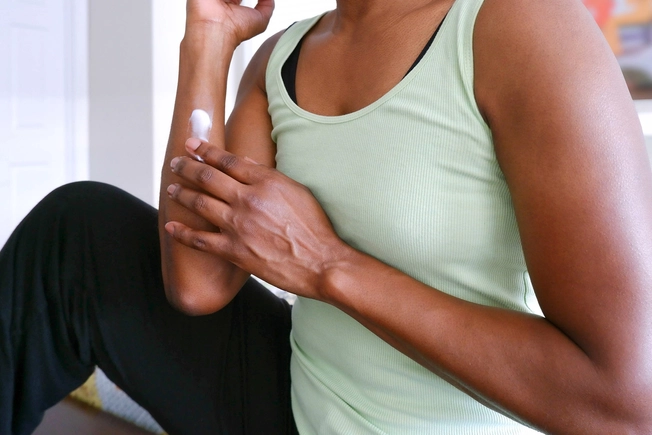
Skin Care
Your skin’s outer layer protects the inner layers from irritants and infections. People with atopic dermatitis have dry skin that isn't as protective. If you have eczema, use mild cleansers and a moisturizer after you wash. And don’t take hot showers or baths, or linger too long while showering or bathing.

Causes
Doctors don't know exactly what causes atopic dermatitis, the most common form of eczema. Genes likely play a role. An immune system problem could create inflammation in the skin. Emotional problems aren’t a cause, but stress can make symptoms worse.

Try Not to Scratch
It’s easier said than done, of course. Eczema is very itchy. But scratching worsens the rash and can make an infection more likely. Use a cold compress to soothe the skin. Try to distract children with activities. Moisturizers are soothing, and some medicated creams or ointments may help, too.

Corticosteroids
Over-the-counter hydrocortisone or nonsteroidal prescription creams may ease mild to moderate eczema. Ask your doctor before using corticosteroids on children under 2. Don’t use them for more than 7 days. Sometimes, stronger corticosteroids are needed to control inflammation. Side effects, like thinning skin, infections, and stretch marks, are more likely with long-term use. You have to be careful using steroids on the face, especially around the eyes. For severe eczema, your doctor may recommend steroid shots or pills, or biological injections.

Antihistamines
There’s some evidence that these medicines may bring relief from the cycle of itching and scratching for some people with atopic dermatitis. When taken by mouth, they can make you drowsy, so that you fall asleep more easily and hopefully scratch less when you’re asleep. Many over-the-counter and prescription-only options are available, each with slightly different dosing and side effects. Check with your doctor for a recommendation.

Taming the Immune Response
Prescription skin meds that calm an overactive immune system can treat eczema from atopic dermatitis. Doctors generally prescribe them only for short-term use in people who’ve tried other treatments that haven’t helped. They have a "black box" warning due to a higher cancer risk. So ask your doctor about the pros and cons. A biologic medication called Dupixent, given as a shot, works on the immune system to treat atopic dermatitis.
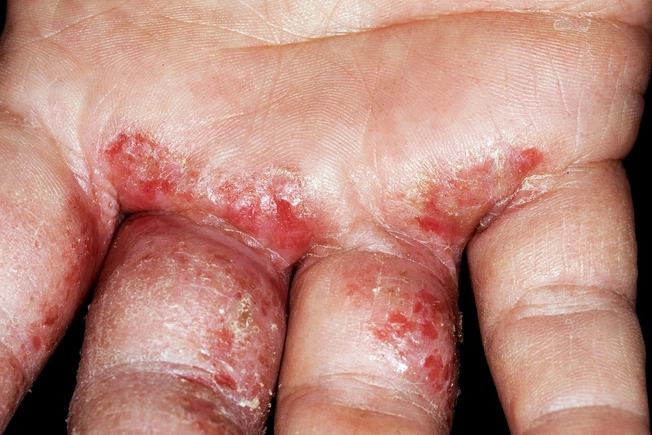
Hand Eczema
Alitretinoin, a relative of vitamin A, may improve or even clear up this condition when other treatments don't work. It hasn’t yet been approved by the FDA for this use. It can give you headaches or dry, flushing, or sun-sensitive skin. Alitretinoin can cause severe birth defects, so you shouldn’t take it when you’re planning to get pregnant.

Phototherapy
UV light affects the immune system. In some people, it can improve moderate to severe cases of eczema from atopic dermatitis or contact dermatitis. Usually, these treatments use UVB light. “PUVA” is a UV treatment combined with a drug called psoralen. But it doesn’t work for everyone, and it makes some people's eczema worse. Too much UV light is bad for your skin. So you should talk to your doctor about the risks and benefits.

Helping Your Child Feel Better
If your child has eczema, keep their fingernails short and their skin moisturized. Dress them in loose-fitting clothes and make sure they don't get overheated. Depending on how severe their eczema is, your doctor may recommend wet wraps, a diluted bleach bath, over-the-counter or prescription medications, and/or light therapy to help.
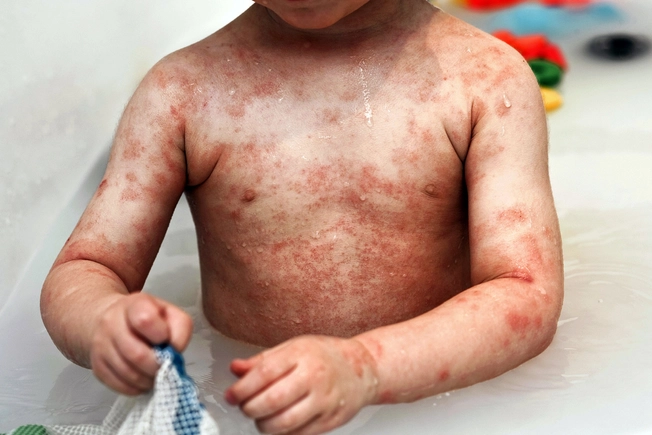
Bleach Baths
A small amount of household bleach in the bath may help tame inflammation, though recent research shows it may not help prevent infections. Talk to a dermatologist or other doctor first. These baths use a specific amount of bleach, greatly diluted. Never put bleach directly onto skin!

Natural Treatments
Some research shows that coconut oil, sunflower oil, and vitamin B12 skin creams may help. So can massage and other things that lower your stress level, since stress can make eczema worse. Herbs and supplements can have side effects, so talk to your doctor first.
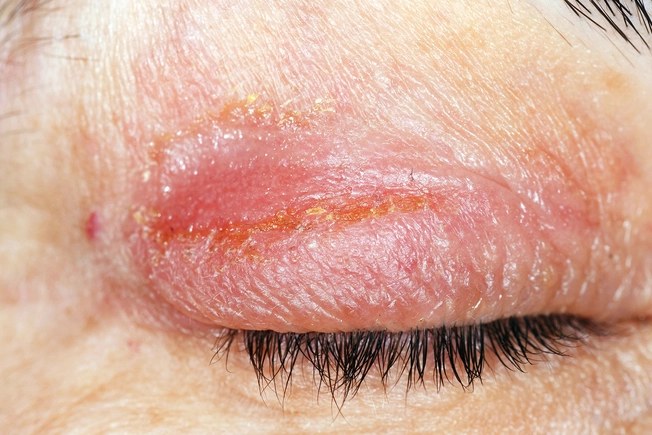
Eczema and Infections
These can look a lot alike. You’ll want to make sure that it really is eczema, and not an infection. Tell your doctor about symptoms of an infection, such as honey-colored crusts, pus- or fluid-filled blisters, scaly patches, swelling, or a fever.

Caring for Dry Skin
Even when the eczema eases up, your skin may still be dry. Take short daily baths in warm water. Pat your skin partially dry and use a thick moisturizer, as well as any medication, right after your bath. Moisturize throughout the day and stick to mild soaps or cleansers. Look for fragrance-free products to help prevent a reaction. Remember, "unscented" may just mean the product has another ingredient to mask the scent.

Living With Eczema
Does your child feel self-conscious about his rashes? Help him avoid triggers, set up a routine for bathing and moisturizing, and stick to your treatment plan. Adults with the condition may also need to take a look at their routines to avoid exposure to some chemicals in cleaning products, perfumes, and cosmetics, as well as cigarette smoke.