Oral Herpes
Oral herpes is an infection caused by the herpes simplex virus (HSV). The virus causes painful sores, most commonly on or around your lips, but you may also get sores on your tongue, the roof of your mouth, and inside your cheeks. These sores are also called "cold sores" or "fever blisters." HSV can also cause symptoms such as fever and muscle aches, especially during your first outbreak of infection.
What does mouth herpes look like?
Early-stage oral herpes. HSV causes fluid-filled blisters in and around your mouth or under your nose. You may have one or two large blisters or patches of tiny blisters that merge into one big, red patch.
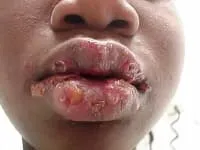
Late-stage oral herpes. After a couple of days, the blisters will break open and ooze a yellowish fluid. After a couple more days, the weeping sores will crust over and begin to heal.
Types of HSV
There are two types of HSV: HSV-1 and HSV-2.
HSV-1 usually causes oral herpes, and HSV-2 usually causes genital herpes. However, it is possible for HSV-1 to cause genital herpes and HSV-2 to cause oral herpes.
Once you're infected, you will have the virus for the rest of your life. When the virus isn't active (causing symptoms), it stays inactive in a group of nerve cells in your spine.
Is oral herpes an STD?
The answer to this question is complicated. Most people get infected with HSV-1 in childhood through nonsexual contact with an infected relative or friend. However, it can also spread through sexual contact. Meanwhile, it's possible to get HSV-2 (the kind that causes most cases of genital herpes) through nonsexual contact. Sometimes, people don't have any symptoms after getting infected, so it's not always possible to tell exactly how or when it happened. Technically, the CDC considers oral herpes an STD or STI (sexually transmitted infection), but that doesn't necessarily mean you got it through sexual contact.
The most important thing is to be honest and open with your potential sexual partners about any infections you could pass on to them before you have intimate contact or sex.
Oral Herpes Causes
You get oral herpes by touching a contagious area on a person infected with HSV-1 (most common) or HSV-2. The virus enters your body through broken skin or mucous membranes, such as those in your mouth or in and around your genitals. Most people get infected with HSV-1 through nonsexual contact with infected spit during childhood. Some people get infected through kissing or performing oral sex on an infected person. However, it's also possible to get it by sharing lip balm or razors, drinking out of the same glass, or eating with the same silverware as an infected person.
You can be infected with HSV even if the infected person doesn't have any symptoms because the virus can reactivate without causing symptoms. This is called asymptomatic shedding, viral shedding, or asymptomatic reactivation.
Is oral herpes contagious?
Yes, HSV is very contagious. In fact, most people are infected with HSV-1 as kids when an infected relative or friend gives them a kiss. The World Health Organization (WHO) says that about 67% of people worldwide are infected with HSV-1, and about 13% are infected with HSV-2.
Oral Herpes Symptoms
After the herpes virus infects you, your symptoms will usually pass through three stages:
Incubation period
The incubation period is the time between virus exposure and the onset of symptoms. For both HSV-1 and HSV-2, the incubation period is 2-12 days. For many people, it's about about 4 days.
Primary infection or outbreak
Often, people won't have any symptoms at all. Sometimes, people have mild symptoms, which they might mistake for something else. If you do have symptoms, the ones you have during the primary infection phase are usually the worst.
Symptoms of primary infection include flu-like symptoms, such as:
- Fever
- Body aches
- Sore throat
- Headache
- Swollen lymph nodes, usually near where the virus entered your body
You may also get a single, painful, fluid-filled blister or a cluster of blisters on or around your lips or under your nose. You may get sores inside your mouth and at the back of your throat. The sores usually last about 7-10 days. About 2 days after the blisters form, they burst and ooze fluid, and after about 5-8 days, the sores will form a yellowish crust and heal. The blisters, fluids, and sores are all contagious, so don't have intimate contact with others until all your symptoms are gone.
Recurrent infection or outbreak
Some people never have an outbreak after the first one. Others will have outbreaks of infections every once in a while. Doctors aren't sure what causes the virus to reactivate in people who have periodic outbreaks, but they think the following may increase your risk of having one:
- Being out in the sun for a long time or when the sun is very bright or intense
- Having a fever or an illness
- Emotional stress
- Having your period if you're assigned female at birth (AFAB)
- Physical stress, such as an injury or having surgery
You're more likely to have a recurrent infection the first year after you're infected. If you do have a recurrent outbreak, it will usually be milder and won't last as long (usually about 8-10 days). Over time, you'll likely get fewer outbreaks as your body makes proteins (called antibodies) that can keep you from having any symptoms (though you'll always have the virus).
The most common symptoms of a recurrent outbreak include:
- A couple of days before, redness, swelling, heat, pain, tingling, or itching in the area where you'll get a blister (this is called a "prodrome")
- Blisters on your lips or under your nose, most often on the edges of your lips
- After a couple of days, the blisters will burst and ooze
- After about 4-6 days, the sores will crust and heal
When to Seek Medical Care
Most cases of oral herpes will clear up without any medical treatment. But see your doctor if:
- This is the first time you've had an outbreak
- You have a weakened immune system, for instance, because you have HIV or are taking immune suppressive drugs
- Your sores don't heal within 2 weeks
- Your symptoms are severe or so painful that you have trouble eating or drinking
- You have outbreaks often
- You have gritty or painful eyes
Oral Herpes Tests
Your doctor may be able to diagnose oral herpes based on where your blisters are and what they look like on a physical examination.
To confirm that you're infected with HSV, your doctor may also take a sample from your sores to do lab tests, such as looking at the sample under a microscope.
If you don't have sores, your doctor may use a blood test to look for antibodies (proteins your immune system makes) to HSV-1 or HSV-2. This will confirm that you have been infected with HSV although it won't say if you have an active infection.
Oral Herpes Risk Factors
Most adults are infected with HSV, even if you've never had symptoms. You're more likely to get HSV if you:
- Were assigned female at birth (AFAB)
- Have had multiple sex partners
- Started having sex at a young age
- Have a history of STD or STI
- Have a weakened immune system
- Don't use condoms and dental dams for intercourse and oral sex
You're most at risk of complications from the virus if you have a weakened immune system because you:
- Have HIV or AIDS
- Have an autoimmune condition, such as eczema, rheumatoid arthritis, or systemic lupus erythematosus
- Take chemotherapy drugs because you have cancer
- Take antirejection medicine because you had an organ transplant
Oral Herpes Treatment at Home
To ease your pain and discomfort, try some of these remedies:
- Use over-the-counter (OTC) cold sore medicines. For instance, docosanol (Abreva) may help shorten your healing time. Some other OTC cold sore medicines include alcohol, which can dry up your blisters and help you heal faster. Always use a cotton swab to apply the ointment according to the package directions. Using a cotton swab will help prevent spreading the infection to other parts of your body.
- Use lip balms or creams with sunblock to protect your lips from the sun, which can trigger a recurrent infection.
- Use ointments with benzocaine or lidocaine to numb sores in or around your mouth.
- Use a cold or warm compress on your blisters to help remove crusting and soothe your pain.
- Take acetaminophen (Tylenol), ibuprofen (Advil), or naproxen (Aleve) for pain, fever, and muscle aches.
- Drink plenty of fluids. Cold drinks and popsicles can help soothe sores in and around your mouth.
Medical Treatment
Most cases will clear up in 2-4 weeks without any specific treatment. But, treatment can make your symptoms less severe and shorten how long they last. Your doctor may recommend treatment options depending on your:
- Overall health and medical history
- Ability to tolerate certain therapies
- Age
- Personal preferences
Your doctor will also likely recommend that you:
- Keep the infected area clean and dry
- Take oral antiviral medicines, such as acyclovir (Zovirax), famciclovir, and valacyclovir (Valtrex), especially if you have recurrent infections often or have very painful symptoms.
- Use antiviral ointments on your sores, such as penciclovir (Denavir) or acyclovir
- Take nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen or naproxen to control your pain
Medicines used to treat recurrent infections work best when you start them within 48 hours of the onset of your symptoms.
Some people may need to go to the hospital, including:
- People with weakened immune systems, such as people with HIV infection
- People with infections that include multiple sites or their internal organs (disseminated HSV)
- People with severe complications, such as encephalitis (brain infection) and keratitis (eye infection)
- Infants who were exposed to HSV during delivery (neonatal herpes)
Follow-up
- Drink plenty of fluids and watch for signs and symptoms of dehydration.
- Use NSAIDs, such as ibuprofen or naproxen, to control any fever and pain.
- Use antiviral medications, as instructed by your doctor.
Oral Herpes Prevention
If you get cold sores more than nine times a year or if you're at high risk of serious complications, your doctor may prescribe an antiviral medicine for you to take regularly.
If sunlight seems to trigger your condition, apply sunblock to the spots where you usually get cold sores. Or ask your doctor about using an oral antiviral medicine before you do outdoor activities that cause an outbreak.
Consider the following to prevent transmitting HSV:
- If you're having any symptoms, don't kiss other people on the mouth or perform oral sex on them until your sores have healed and your skin looks normal.
- Don't share personal care items such as lip balms, towels, or toothbrushes. Don't eat or drink after others or allow others to eat or drink after you.
- Don't kiss someone or perform oral sex on them if they have visible sores on or around their mouth or genitals.
- Even if you and your partner(s) have no symptoms, use a dental dam or condom when you're performing or receiving oral sex.
- When you have cold sores, wash your hands carefully before touching yourself or other people, especially babies.
Outlook
Most cases will clear up in 2-4 weeks on their own. Treatment with an antiviral medicine may make your symptoms less severe and shorten how long they last.
Once you have been infected with HSV, you'll always have the virus. There is no cure. However, many people never have a second outbreak or only have a couple of outbreaks during their lives. Some people have recurrent outbreaks, often due to sun exposure, an illness, emotional or physical stress, or hormone changes, such as getting your period if you're AFAB. Recurrent outbreaks are usually less severe and shorter than the first outbreak.
Takeaways
Oral herpes is usually caused by infection with HSV-1. Most adults are estimated to acquire HSV-1 by the age of 50. HSV-1 usually causes blisters called "fever blisters" or "cold sores" around your lips and in your mouth. The sores can be painful, but they usually clear up on their own in about 2-4 weeks. Once you're infected with HSV, you have it for life, so you may have outbreaks every once in a while. To help ease any pain and fever, use NSAIDs, such as ibuprofen or naproxen. Ask your doctor about a prescription antiviral medication to help shorten your infection time and keep yourself from passing HSV on to other people.
Oral Herpes FAQs
How do you know if you have oral herpes?
Sometimes, you may not know you were infected with HSV because you don't have any symptoms or you have mild symptoms that could be something else. However, if you get fever blisters or cold sores, that's the main symptom of oral herpes.
Is oral herpes that big of a deal?
Oral herpes can cause painful sores in and around your mouth, but most people will get over the infection in about 2-4 weeks without any medical treatment. For some people with weakened immune systems, any infection can be serious. If you have a weakened immune system because you have HIV or are taking immune suppressive drugs and you develop fever blisters or cold sores, talk to your doctor so they can help make sure your infection doesn't become serious.
Does oral herpes mean I have herpes?
That depends on what you mean by "having herpes." Most people use the term to mean genital herpes. You may or may not have genital sores with an HSV-1 infection, which causes most cases of oral herpes. Regardless of where you have symptoms, you can still pass it on to other people. So, you need to be honest with potential intimate partners about any infections you could spread to them. Don't engage in intimate or sexual contact when you have symptoms.
