- Overview
- Types
- Symptoms
- Causes & Risks
- Tests & Diagnosis
- Treatment
- Parenting
- School
- Living With
- Complications
- View Full Guide
Ways to Manage ADHD That Aren't Drugs


Know Your Options
If your child’s been diagnosed with ADHD, you want to know what can help him. Medication isn’t the only way to treat it. Other things can help, too. And many can be used along with medication or other nondrug treatments. Talk to your doctor to come up with a treatment plan that works best for your child.

Behavioral Therapy
This type of therapy, also known as cognitive behavioral therapy, can ease your child’s ADHD symptoms and help them feel better. Most of the time, it focuses on identifying and changing thoughts to change behavior. Research shows that it’s very good at improving mindfulness and reducing impulsive behavior. People with ADHD often have mental health problems like depression or anxiety, and behavioral therapy helps with these, too. It usually works best when combined with ADHD medication.

Behavior Therapy For Parents
As part of behavioral therapy, parents take a class or meet with an ADHD specialist to learn to help their child manage ADHD symptoms. It can help your child improve their behavior and strengthen your relationship with them, too. Ask your child’s doctor or an ADHD expert to recommend a therapist.

Behavior Therapy For Teachers
Teachers, too, learn ways to make it easier to work with kids with ADHD. Since an estimated 11% of kids in the U.S. are diagnosed with it, the training can help teachers with many students -- not just your child. Schools will help support students with ADHD. If you want to see if your child’s teacher may be open to such training, meet with the teacher or principal and discuss what you’ve learned from behavioral therapy.

Coaching
This is a newer type of ADHD treatment. Coaches -- who are sometimes called executive function coaches or organizational coaches -- aren’t the same as therapists or doctors. Some coaches may be licensed therapists or medical professionals, but they use different techniques during coaching. They help kids and adults with ADHD learn skills that help them manage symptoms. For example, coaches can help with goal setting, problem solving, and time management.
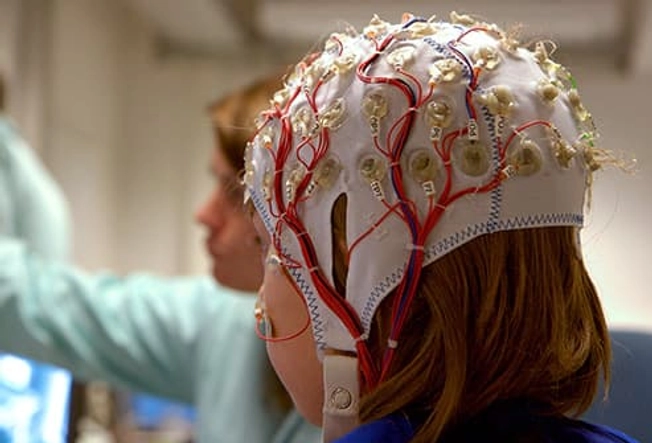
Neurofeedback
Neurofeedback -- also called brain training or EEG biofeedback -- involves placing headgear with sensors on your child’s scalp to monitor brain waves. While your child wears the sensors, they play a computerized game using their brain, which helps them learn how their brain works. The idea is that learning about their brain and how to control it can help ease ADHD symptoms. The verdict is still out on neurofeedback. But it doesn’t have any side effects, and some research shows that it improves some kids’ ability to pay attention, manage time, and stay on task. It’s also shown to lower impulsive and antsy behavior.

Music Therapy
Kids with ADHD often struggle with stress and anxiety. Music can be relaxing, which is why some experts think it’s good medicine. What’s more, music has a start, an end, and a rhythm. Some experts think that structure may help kids with ADHD get through everyday activities. Music therapy isn’t supposed to replace behavioral therapy or medication. Most ADHD professionals use it alongside other treatments.

Assistive Technology (AT)
ADHD affects the brain’s frontal lobes -- that’s an area that helps you get organized and plan ahead. Because of this, kids with ADHD may struggle to stay on top of homework and tasks at home, too. Some parents find that assistive technology -- like cell phone apps, online calendars, screen readers, and talking calculators -- help their kids pay attention. Many kids like screens and may be more willing to use apps that involve a cell phone, tablet, or other computer. There’s no one type of AT that’s most effective, so you may have to try several tech tools to see what works best for your child. And too much screen time may make some kids' symptoms worse. In addition, the FDA has approved a video game called EndeavorRX that can help improve attention.

Exercise
Regular exercise eases many ADHD symptoms. It can help kids pay attention and can boost their mood, too. Exercise may even help make it less likely that your child does risky things like speeding while driving, or abusing alcohol. One reason? Even short bursts of physical activity can raise levels of brain chemicals like dopamine.
Activity also helps with sleep. If your child often doesn’t get enough shut-eye, it can make ADHD symptoms stronger.

Healthy Diet
A bad diet doesn’t cause ADHD. But experts say that a nutritious diet filled with fruits and vegetables, whole grains, and lean protein is important for healthy brain development.
A small amount of research suggests that ADHD symptoms improve in some (but not all) kids after they stop eating anything that contains artificial food dyes. (Food dye can be found in some candy, cereals, and other foods.) Healthy levels of omega-3 fatty acids and other nutrients like zinc may also help. But there’s no proof that any one type of diet can greatly curb symptoms or cure ADHD.

Supplements
While vitamins and minerals in your diet can help your brain stay healthy, it’s not clear if certain nutritional supplements can help ADHD. Some research suggests that zinc supplements may help kids with ADHD be less hyperactive and impulsive. Other studies show that fish oil supplements might help with ADHD symptoms, too. But more research is needed. Be sure to talk to your doctor before your child takes any new medications, including over-the-counter supplements.
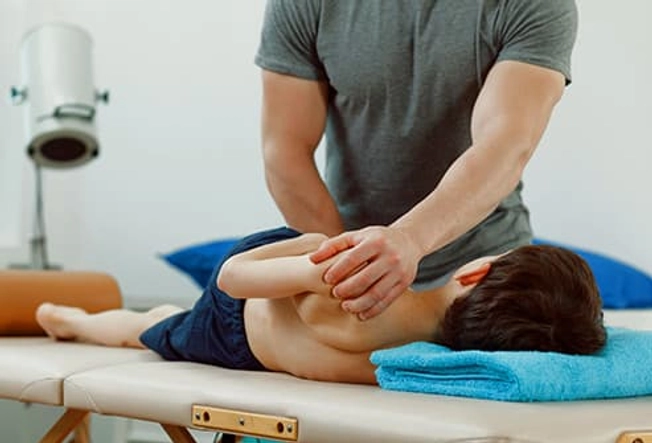
Chiropractic Care
This is a controversial ADHD treatment option. Chiropractors believe spine issues, like “misalignment,” may contribute to ADHD symptoms. One small study suggests some kids with ADHD may benefit from chiropractic care. But experts don’t know whether adjusting a person’s spine can affect brain areas that play a role in ADHD.