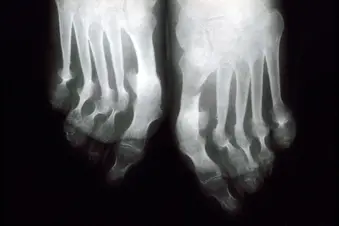
Until recently, little was known about psoriatic arthritis (PsA), a disease first described and classified by the medical community in the 1970s. A 2008 Belgian study offered hope to people with psoriatic arthritis who want to live a "normal," pain-free life again.
It found that a better understanding of how to diagnose and manage symptoms, along with advances in medicine, have made it possible for those living with the disease to reach remission.
But it's important to understand what exactly "remission" means so you can manage your expectations and keep symptoms from returning.
How Is 'Remission' for Psoriatic Arthritis Defined?
The medical community realized that they didn't have a clear definition as to what psoriatic arthritis remission meant. And they had no standard way of measuring how someone responded to treatments.
After much trial and error, rheumatologists (doctors who specialize in arthritis and other diseases of the joints, muscles, and bones) now define PsA remission as getting to "a minimal disease activity state."
And they now have tools and questionnaires to measure disease severity as well as how you feel you're doing. Some of these were originally created for other diseases, like rheumatoid arthritis, or have been used in studies. Assessment tools help doctors diagnose PsA and manage its treatment. They're a way to get you and your doctor to understand each other and talk about what's happening.
There are two types of remission:
Drug-induced, which is very low disease activity while you're taking medication
Drug-free, when you have complete relief from joint tenderness and swelling without medication
Reaching Remission: T2T
The standard for PsA care is becoming a "treat-to-target" (T2T) strategy, where minimal disease activity is the goal. What exactly that target looks like is something you and your doctor will agree on, probably a combination of scores, test results, and your quality of life.
Your doctor will come up with a treatment plan to make it happen, including benchmarks and next steps to take if those aren't met. How mild or severe your PsA is could affect how fast you get there.
You may see your doctor once every 4 weeks -- more often than you would with a typical treatment strategy -- so they can check on your symptoms, follow up with lab tests, and adjust your medication with that remission target in mind.
Does Early Treatment Raise My Chances of Remission?
Starting treatment as soon as possible to shut down the disease could make ongoing psoriatic arthritis remission more likely. Repeated episodes of joint inflammation can cause irreparable harm. Early, aggressive treatment can prevent joint damage, leading to a better long-term outlook.
For example, TNF blockers or TNF inhibitors, a kind of medicine called biologics, have been successful in treating PsA. In one study, more than half of people who used them were in remission a year later.
How to Avoid a Psoriatic Arthritis Relapse
There's no cure for PsA. Anti-rheumatic drugs don't change the underlying fact that you're affected by the disease. There may be places in your body where it still lingers even when your joints don't feel painful or swollen.
Remission as a result of taking anti-TNF biologics or other medicines is drug-induced, so your doctor will likely recommend you stay on your medication. Three out of 4 people who stopped taking their disease-fighting medication in one small study had symptoms return within 6 months. Fortunately, starting their medication again restored remission.
Although some people can stay in psoriatic arthritis remission without drugs, it's not common. If you want to try a lower dose or to stop taking a medicine once you've reached remission, you'll need to work with your doctor closely. As soon as symptoms begin, you'll need your medication again.
Changes in how you handle things in your daily life can also help prevent some PsA symptoms from returning. Some arthritis medications can cause fatigue, so pace yourself and stop to rest before you get tired. Protect your joints, keep your weight in check, and make regular joint-friendly exercise such as walking, swimming, or biking part of your routine.
What If Symptoms Come Back?
Psoriatic arthritis remission can last for weeks or years, then one day your symptoms suddenly show back up. Call your doctor as soon as you can. Early treatment can help prevent more problems down the road.
Show Sources
Photo Credit: Clinical Photography, Central Manchester University Hospitals NHS Foundation Trust, UK / Science Source
SOURCES:
Therapeutic Advances in Musculoskeletal Disease: "Is Remission a More Realistic Goal in Psoriatic Arthritis?"
Current Rheumatology Reports: "Remission in psoriatic arthritis."
Rheumatology Advisor: "Measuring Disease Activity in Psoriatic Arthritis."
Dermatology World Meeting News: "Tools help with diagnosis and assessment of psoriasis, psoriatic arthritis."
Arthritis Foundation: "How to Achieve Remission in Psoriatic Arthritis."
National Psoriasis Foundation: "Why early diagnosis is critical for psoriatic arthritis."
International Journal of Clinical Rheumatology: "Aiming for Remission in Psoriatic Arthritis."
Arthritis Research & Therapy: "Remission in psoriatic arthritis: is it possible and how can it be predicted?"
Annals of the Rheumatic Diseases: "Remission in PsA: What are the Chances?" "High incidence of disease recurrence after discontinuation of disease-modifying antirheumatic drug treatment in patients with psoriatic arthritis."
Mayo Clinic: "Psoriatic arthritis: Diagnosis & treatment."
Rheumatoid Arthritis Support Network: “PsA Facts: How Prevalent is Psoriatic Arthritis?”