1 of 3 / A Balanced Life
View All
Is My Medical Condition Making Me Angry?
Anger is a natural, healthy emotion. But frequent outbursts can be harmful to your health.
Boost Your Energy in 10 Minutes or Less
Are your eyelids sagging as the afternoon wears on? What you need: a lasting solution to keep sluggishness at bay.
Life and Wellness Coaches
Life and wellness coaches push their clients to achieve success in their career, relationships, or lifestyle.
2 of 3 / Manage Stress
View All
Controlling Stress
No matter how busy your schedule, it is possible to manage stress and keep it from ruining your life.
Tips to Manage Stress
Managing stress is key to your health. And it isn't so very difficult to do.
Causes of Stress
Read on to learn why you get stressed out, and how that stress might be affecting your health.
How Worrying Affects the Body
When worrying becomes excessive, it can lead to feelings of high anxiety and even cause you to be physically ill.
3 of 3 / CAM Treatments
View All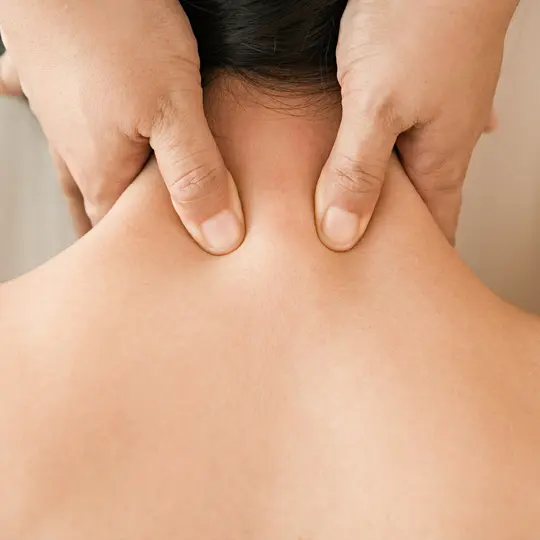
Differences Between Complementary and Alternative Medicines
Many people take “complementary medicine” and “alternative medicine” to mean the same thing.
What Is Alternative Medicine?
Alternative medicine is a term that describes medical treatments that are used instead of traditional (mainstream) therapies.
Acupressure Points and Massage Treatment
Used for thousands of years in China, acupressure applies the same principles as acupuncture to aid relaxation and wellness.
Massage Therapy Styles and Health Benefits
Massage has been practiced for thousands of years. Today, if you need or want a massage, you can choose from among 80 styles.
Suggested Reads about Health & Balance
How Your Future Self Can Make You Healthier Right Now
Connecting with your future self can benefit you today, research shows. Here are two science-backed ways to do just that.
Toxic Positivity: When ‘Good Vibes Only’ Goes Too Far
Toxic positivity is when you insist on hyping the positive to an unrealistic and even damaging extent. And you might not even know you’re doing it.
Playing with Dogs Helps People Concentrate and Relax, Study Says
The study found that walking a dog relaxes people; brushing the dog improves concentration; and playing with the pooch does both.
Why Immersion in Very Cold or Hot Water Can Be So Healthy
Cold plunges, hot tubs, face dunking – trendy water activities may be very good for you. We ask experts why.
8 million+ Physician Ratings & Reviews
Find Doctors and Dentists Near You
You can also search by physician, practice, or hospital name