A Visual Guide to Cervical Cancer

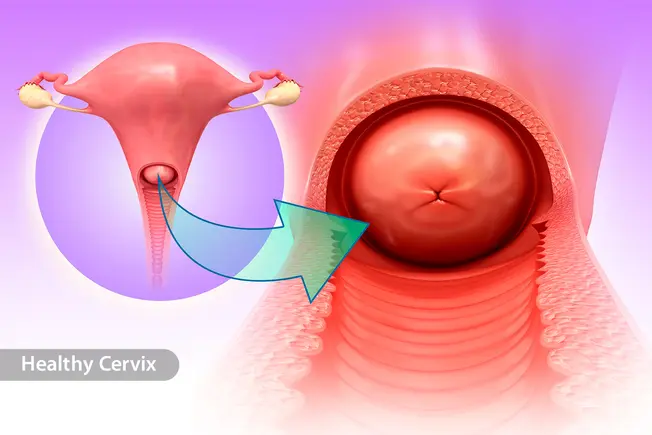
What Is Cervical Cancer?
Cervical cancer occurs when abnormal cells develop and spread in the cervix, the lower part of the uterus. More than 13,000 new cases are diagnosed each year in the U.S. A unique fact about cervical cancer is that most cases are triggered by a type of virus. When found early, cervical cancer is highly curable.

Symptoms of Cervical Cancer
When cervical cells first become abnormal, there are rarely any warning signs. As the cancer progresses, symptoms may include:
- Unusual vaginal discharge
- Vaginal bleeding between periods
- Bleeding after menopause
- Bleeding or pain during sex

Top Cause of Cervical Cancer: HPV
The human papillomavirus (HPV) is a large group of viruses. About 40 types can infect the genital areas, and some have high risk for cervical cancer. Genital HPV infections usually clear up on their own. If one becomes chronic, it can cause changes in the cells of the cervix. And it's these changes that may lead to cancer. Worldwide, over 90% of cervical cancers are caused by an HPV infection.
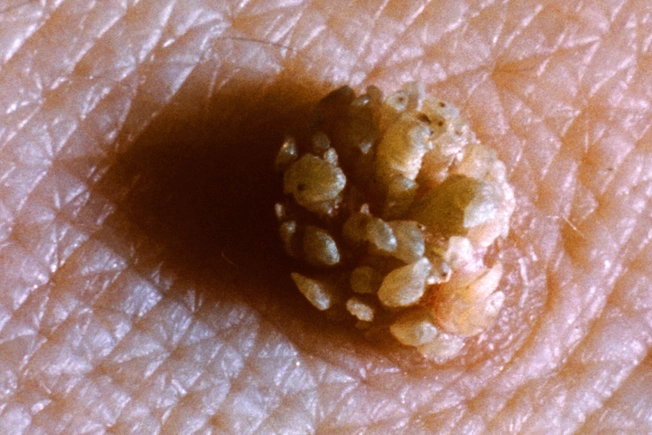
Symptoms of HPV
HPV infections usually have no symptoms and go away on their own. Some types of the HPV virus may cause genital warts, but these are not the same strains linked to cervical cancer. It's important to note that genital warts will not turn into cancer, even if they are not treated. The dangerous types of HPV can stay in the body for years without causing any symptoms.

Who Is at Risk for HPV?
HPV is so common that most people who have ever had sex -- both women and men -- will get the virus at some point in life. Because HPV can linger quietly, it's possible to carry the infection even if it has been years since you had sex. Condoms can lower your risk of getting HPV, but they do not fully protect against the virus. HPV is also linked to cancers of the vulva, vagina, penis, and to anal and oral cancers in both sexes.
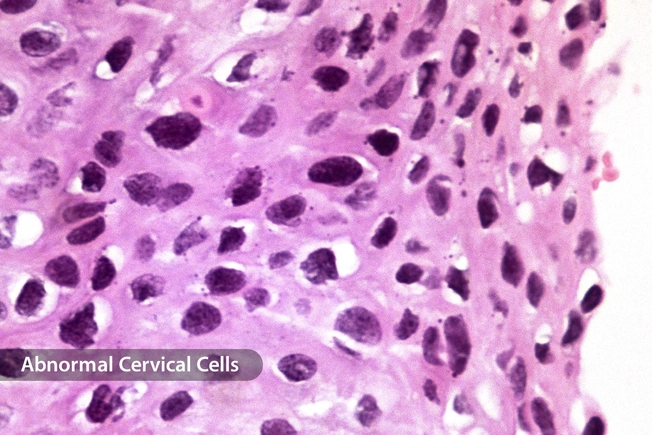
How HPV Causes Cervical Cancer
If one of the high-risk strains of HPV lingers in the body, it can cause abnormal cells to develop in the cervix. These precancerous changes do not mean that you have cervical cancer. But over time, the abnormal cells may give way to cancer cells. Once cancer appears, it tends to spread in the cervix and surrounding areas.

What Else Raises Your Risk?
Hispanic and African-American women have higher rates of cervical cancer than white women. The risk is also higher in infected women who:
- Smoke
- Have many children
- Use birth control pills for a long time
- Are HIV positive or have a weakened immune system
- Have multiple sexual partners
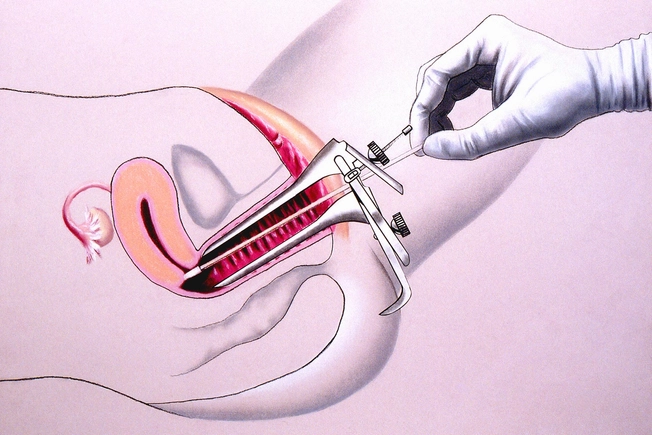
Early Detection: Pap Test
The Pap test is one of the great success stories in early detection. A swab of the cervix can reveal abnormal cells, often before cancer appears. At age 21, women should start having a Pap test every three years. From age 30 to 65, women who get both a Pap test and an HPV test can go up to five years between testing. But women at higher risk may need testing more often, so it's best to check with your doctor who will help you know what the best testing schedule is for you. Skipping tests raises your risk for invasive cervical cancer.
Of note: You'll still need Pap tests after getting the HPV vaccine because it doesn't prevent all cervical cancers.
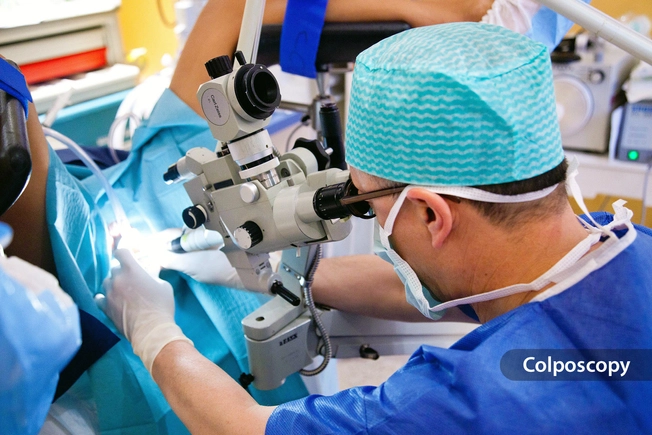
What If Your Pap Test Is Abnormal?
If test results show a minor abnormality, you may need a repeat Pap test. Your doctor may schedule a colposcopy -- an exam with a lighted magnifying device -- to get a better look at any changes in the cervical tissue and also take a sample to be examined under a microscope. If abnormal cells are precancerous, they can then be removed or destroyed. Treatments are highly successful in preventing precancerous cells from developing into cancer.

Early Detection: HPV DNA Test
In some cases, doctors may offer the option of the HPV DNA test in addition to a Pap test. This test checks for the presence of high-risk forms of HPV. It may be used in combination with a Pap test to screen for cervical cancer in women over 30. It may also be recommended for a woman of any age after an abnormal Pap test result.

Diagnosing Cervical Cancer: Biopsy
A biopsy involves the removal of cervical tissue for examination in a lab. A pathologist will check the tissue sample for abnormal changes, precancerous cells, and cancer cells. In most cases, a biopsy takes place in a doctor's office during a colposcopy. A cone biopsy allows the pathologist to check for abnormal cells beneath the surface of the cervix, but this test may require anesthesia.
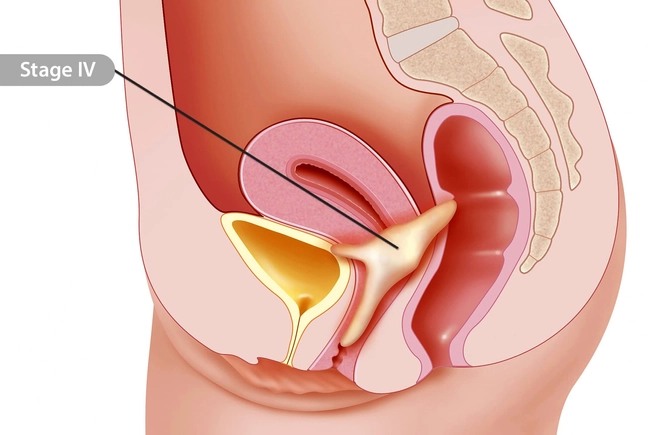
Stages of Cervical Cancer
Cervical cancer is divided into four stages. In stage I, the cancer is beyond the lining of the cervix, but it’s still only in your uterus. Stage II means it’s spread beyond your cervix and uterus. At this stage, it can also spread to nearby tissues. A stage III tumor reaches the lower part of your vagina and may make it hard to pee. Stage IV, the most advanced, means the cancer has spread to other parts of the body, like nearby organs.
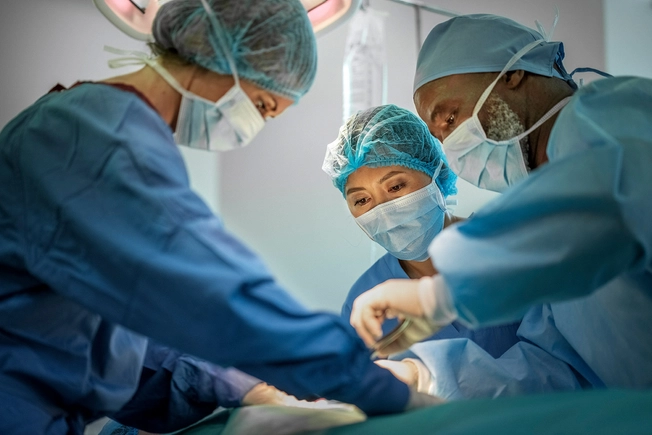
Treatment: Surgery
If the cancer has not progressed past Stage II, surgery is usually recommended to remove any tissue that might contain cancer. Surgical treatment options vary from cervical conization to simple hysterectomy to radical hysterectomy. A radical hysterectomy includes, the removal of the cervix and uterus as well as some of the surrounding tissue. The surgeon may also remove the fallopian tubes, ovaries, and lymph nodes near the tumor.
Treatment: Radiation
External radiation therapy uses high-energy X-rays to kill cancer cells in a targeted area. It can also help destroy any remaining cancer cells after surgery. Internal radiation, or brachytherapy, uses radioactive material that is inserted into the tumor. Women with cervical cancer are often treated with a combination of radiation and chemotherapy. Side effects can include low blood cell counts, feeling tired, upset stomach, nausea, vomiting, and loose stools.
Treatment: Chemotherapy
Chemotherapy uses drugs to reach cancer wherever it is in the body. When cervical cancer has spread to distant organs, chemotherapy may be the main treatment option. Depending on the specific drugs and dosages, side effects may include fatigue, bruising easily, hair loss, nausea, vomiting, and loss of appetite.
Treatment: Targeted Therapy
This treatment targets changes in cancer cells. One of them involves a protein called VEGF (vascular endothelial growth factor) that feeds cancer cells. Bevacizumab (Avastin) is a type of targeted medication called an angiogenesis inhibitor. It blocks VEGF so that the tumor starves. Doctors often combine Avastin with chemo to treat more advanced cervical cancer.

Treatment: Immunotherapy
This treatment unleashes your own immune system to spot and kill cancer cells. Immune checkpoint inhibitors are drugs that block molecules on immune cells that help tumors evade detection. Once the cancer cells are unmasked, your body’s disease-fighting T cells attack the growth.

Coping With Cancer Treatments
Cancer treatments may make you tired or uninterested in food. But it's important to take in enough calories to maintain a healthy weight. Check with a dietitian for tips on eating well during cancer treatment. Staying active is also important. Gentle exercise can increase your energy while reducing nausea and stress. Check with your doctor to find out which activities are appropriate for you.

Cervical Cancer and Fertility
Treatment for cervical cancer often involves removing the uterus and may also involve removing the ovaries, ruling out a future pregnancy. However, if the cancer is caught very early, you still may be able to have children after surgical treatment. A procedure called a radical trachelectomy can remove the cervix and part of the vagina while leaving the majority of the uterus intact.

Survival Rates for Cervical Cancer
The odds of surviving cervical cancer are tied to how early it's found. About 66% of women overall will survive for at least five years after diagnosis. But statistics don't predict how well any one individual will respond to treatment.
Vaccine to Help Prevent Cervical Cancer
The Gardasil 9 vaccine is now available to help prevent diseases caused by 9 types of HPV: cervical, vaginal, and vulvar cancers in females, anal cancer, certain head and neck cancers, such as throat and back of mouth cancers, and genital warts in both males and females.
Males and females from ages 9 to 45 may take the vaccine, which is given over several months. The vaccine helps prevent 90% of cancers caused by HPV.

Who Should Get the HPV Vaccine?
The vaccines are only used to prevent, not treat, HPV infection. They’re most helpful if you get the shots before you start having sex. The vaccine is typically given to people between ages 9 and 45. The CDC recommends the HPV vaccine for all boys and girls at age 11 or 12.