Primary Mediastinal B-Cell Lymphoma: Stages and Treatment

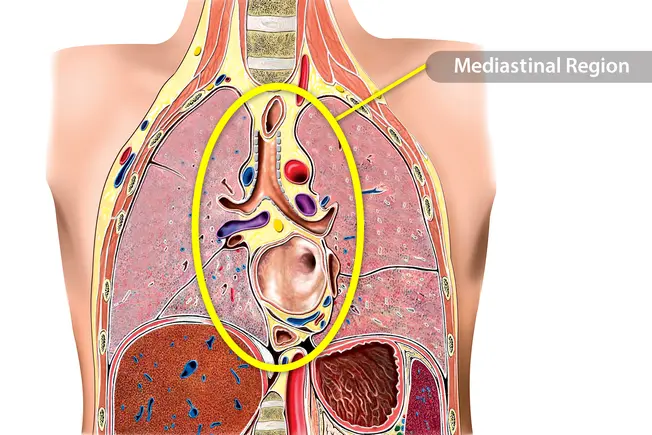
Primary Mediastinal B-Cell Lymphoma (PMBCL)
This cancer is a type of non-Hodgkin’s lymphoma that starts in the mediastinum. That’s the space between the lungs. While doctors usually catch it at an early stage, this lymphoma also tends to grow quickly.
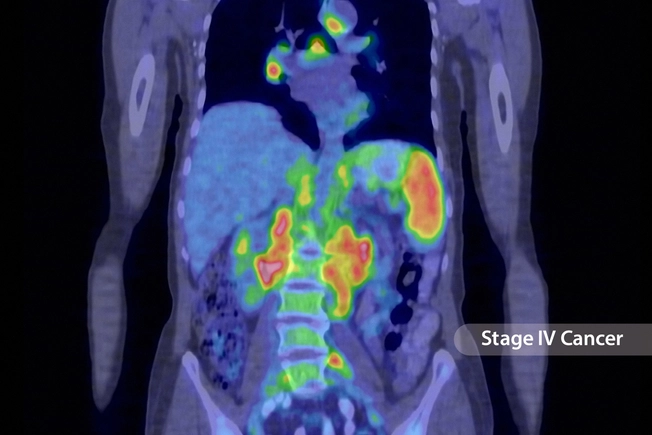
Staging PMBCL
After diagnosis, your doctor will run more tests to find out where the cancer is and if it has spread. PMBCL stages are similar to other lymphomas:
Stage I: The cancer is in one area only.
Stage II: The cancer is in two or more areas on one side of the diaphragm, the large muscle beneath the lungs.
Stage III: The cancer is on both sides of the diaphragm.
Stage IV: The cancer has spread to other organs and tissues. This may include the liver, lung, or bone marrow.

Grading PMBCL
Doctors group lymphomas into low grade or high grade based on how fast the cancer is expected to grow. They consider PMBCL a high-grade lymphoma. That’s because it tends to grow quickly.

A Matter of Size
You might hear a doctor say that the lymphoma is or is not “bulky disease.” Bulky disease means that the tumor mass is more than 10 centimeters across.
Treating PMBCL
Doctors used to consider PMBCL a form of diffuse large B-cell lymphoma (DLBCL). But experts now recognize it as a separate lymphoma. It’s still common for doctors to treat PMBCL with the same combination of drugs used to treat DLBCL. This regimen, called R-CHOP for short, combines three chemotherapy drugs with an antibody and a steroid. They are:
- Rituximab (Rituxan)
- Cyclophosphamide (Cytoxan)
- Hydroxydaunorubicin (Doxorubicin)
- Vincristine (Oncovin)
- Prednisone
Other Treatment Options
It’s now more popular for doctors to use another combination of drugs to treat this cancer. This chemotherapy combo, called R-EPOCH, contains a slightly different mix of drugs.
- Rituximab (Rituxan)
- Etoposide (Etopophos)
- Prednisone
- Vincristine (Oncovin)
- Cyclophosphamide (Cytoxan)
- Hydroxydaunorubicin (Doxorubicin)
Doctors might prescribe a drug called filgrastim to help white blood cells recover from chemotherapy more quickly.

R-CHOP or R-EPOCH?
PMBCL usually responds well to treatment. One study of people with this lymphoma showed that remission happened more often with R-EPOCH than R-CHOP. But people taking R-EPOCH had more side effects.

More Treatment Options
Some people with PMBCL do well with a different drug combination, called MACOP-B. This plan is more often used in Europe. It includes:
- Methotrexate
- Hydroxydaunorubicin (Doxorubicin)
- Cyclophosphamide (Cytoxan)
- Vincristine (Oncovin)
- Prednisone
- Bleomycin (Blenoxane)
Doctors sometimes add rituximab to MACOP-B. But some studies suggest it doesn’t work better.
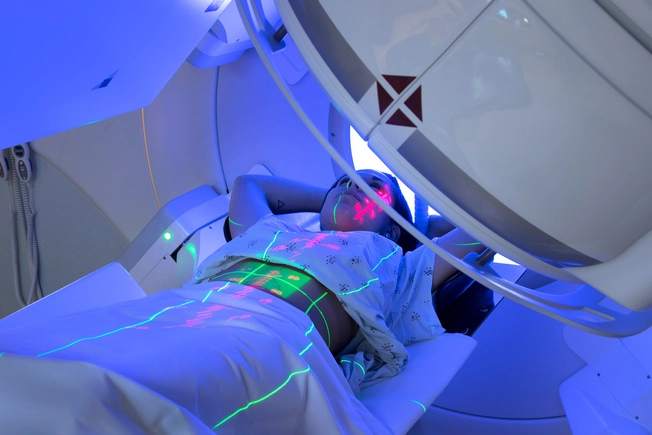
Is Radiation Needed?
After chemotherapy, your doctor might recommend radiation treatment. This therapy can help if your cancer isn’t completely gone. It can also lower the chance that your cancer comes back.
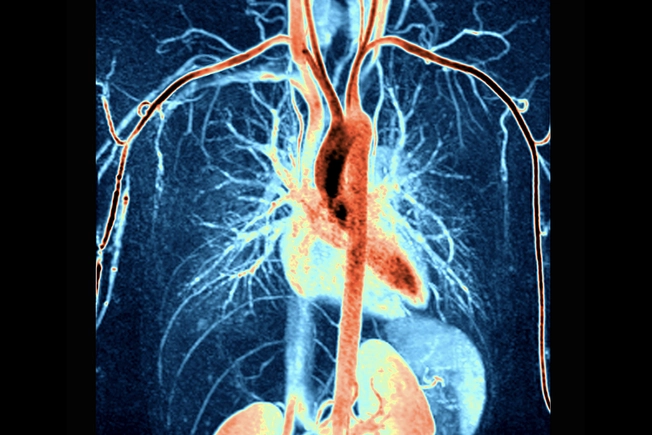
Did It Work?
After treatment ends, an imaging test will show your doctor how well treatment worked. Doctors sometimes use these scans to help decide if you need radiation. The test also will help to show how likely it is the cancer will come back.

When PMBCL Comes Back
PMBCL treatments often work well to get rid of this cancer. But if it comes back, you may have other options. The FDA has approved an immunotherapy drug called pembrolizumab (Keytruda) for people whose PMBCL doesn’t respond to chemo or has come back. This drug helps the immune system fight cancer. CAR T-cell therapy may also be an option. It’s a gene therapy that uses your immune system’s T cells to attack cancer. It’s approved to treat PMBCL that has relapsed.
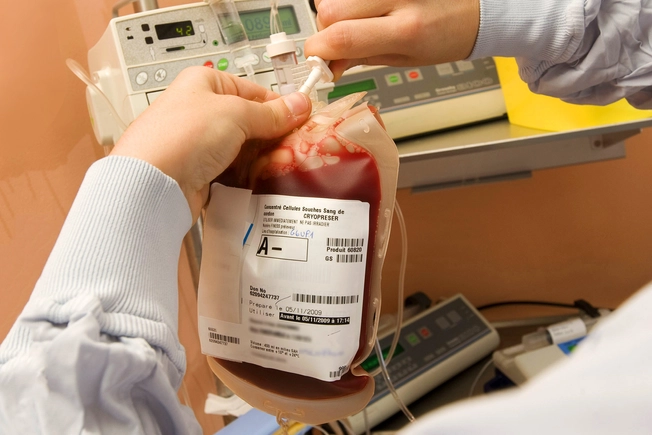
Exploring Other Options
If standard treatments don’t work, a blood stem cell transplant is sometimes an option. This treatment involves high doses of chemotherapy to knock out any cancer cells before infusing healthy cells. The treatment is hard, but it can get rid of PMBCL. Also, ask your doctor if you may be eligible for a clinical trial testing new treatments.