Major depressive disorder is the most widespread mood disorder in the world. Also called clinical depression, or just depression, it's when you have symptoms of low mood or hopelessness for at least 2 weeks. Scientists still don't know what causes it. But they know that treating it is complex and that people who have it need more ways to feel better faster.
For about half a century, scientists have put a lot of effort into improving medications that target a small set of neurotransmitters. Those are chemicals in the brain -- serotonin, norepinephrine, and dopamine in particular -- that affect how your nerve cells talk to each other, which then affects your mood.
Most people respond to standard antidepressants. But at least 30% of people who try two different kinds of these drugs continue to have symptoms of depression. That's called treatment-resistant depression.
So, over the past 2 decades, scientists have changed how they think about treatment for major depressive disorder as their understanding of the brain biology behind depression has changed.
The biggest change is that medication research has gone past only targeting certain neurotransmitters, says Gerard Sanacora, MD, PhD, director of the Yale Depression Research Program in New Haven, CT. "We've opened up a whole new vista of potential targets for new drugs."
New Medications and Faster Results
There's a long-held idea that depression takes weeks or months to resolve. But new fast-acting treatments have "changed what we think is possible in the field," Sanacora says.
In 2019, the FDA approved brexanolone (Zulresso). It's the first drug specifically for postpartum depression, which is a type of major depression. Experts aren't exactly sure how it works. But it's a human-made version of a steroid your body makes naturally. It affects your GABA receptors, which help regulate mood.
Brexanolone isn't as easy to take as other antidepressants. You get it through a vein in your arm at a health care facility over the course of 60 hours. But it can work quickly. Your depression symptoms might start to lift by the end of your treatment.
Another breakthrough drug came out that same year.
Esketamine is a prescription nasal spray. The low-dose psychedelic drug boosts the activity of glutamate in parts of your brain related to mood. Glutamate's job is to excite cells in the brain and nervous system. Esketamine can trigger new connections in your brain too. You may start to see improvements in your depression within hours or days of using it, Sanacora says.
Esketamine offers lifesaving hope for people with suicidal thoughts and relief for people with treatment-resistant depression. But used alone, symptom relief may only last a couple of weeks. That's why experts agree you should take rapid-onset drugs alongside traditional treatments.
As for those with mild or moderate depression, Sanacora still first suggests cognitive behavioral therapy, followed by conventional antidepressants also known as selective serotonin reuptake inhibitors (SSRIs). Doctors need more information on the safety and long-term effects of newer treatments for depression.
"Over the past 20 years, we've had a transformative change in the way we treat depression," Sanacora says. "But we still have to smooth it out to understand for which patients these treatments are best and when."
Improvements in Brain Stimulation
Medications aren't the only treatment for depression. Electroconvulsive therapy has been around for more than 70 years. It remains one of the most effective ways to manage major depressive disorder, especially if you don't respond to other treatments. While it isn't new, scientists have fine-tuned the procedure over the past decades.
Today, electroconvulsive therapy uses less energy than it did in the past. The goal is to give you the same benefits but with less negative impact on your memory and thinking skills. "That's been a huge improvement," says Susan Conroy, MD, PhD, a psychiatrist and neuroscientist at Indiana University School of Medicine.
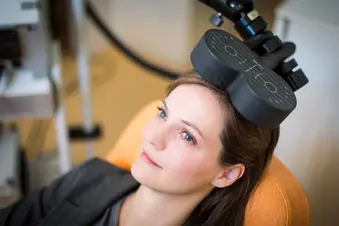
Conroy also uses transcranial magnetic stimulation to treat depression, which has fewer side effects than electroconvulsive therapy. It works by sending magnetic pulses around your skull.
Brain tissue translates these signals into electrical energy, Conroy says, which changes the way areas of your brain talk to each other. "By changing that circuitry, we think that's how transcranial magnetic stimulation gets people better from depression."
These and other forms of brain stimulation aren't right for everyone. But tell your doctor if other treatments don't help and your depression keeps you from doing daily activities, you aren't eating, and you have constant suicidal thoughts.
"These are all signs your treatment needs to be escalated and pretty quickly," Conroy says.
Future Treatment
Lots of other promising treatments for depression are on the horizon. Deep brain stimulation is one. In this treatment, a surgeon implants electrodes in your brain. These nodes send painless zaps that alter the electrical activity that's causing your symptoms.
You can think of this treatment kind of like a pacemaker for your mood. While it's not approved for the general public, it might be soon. "Technology is advancing really quickly," Conroy says.
Researchers are also studying a drug called SAGE-217. Sanacora says there's interest in how it might help prevent a serious relapse in people with a history of depression. The idea is that you'd take it as soon as your symptoms come back. "But you don't wait until the symptoms are full-blown," he says.
There's also a lot of buzz around drugs like psilocybin. Studies show these "magic mushrooms" can ease depression about as fast as ketamine -- what esketamine is made from -- with effects that may last longer. But when it comes to psychedelics, Sanacora says, "We need a lot more research before we can say anything with confidence."
In his 25 years in the field, Sanacora says he's never seen such excitement around treatments for depression. But that doesn't mean researchers have all the answers or that major depressive disorder has a cure.
Still, you can take steps now to ease depression or guard against a relapse. That might include medication, different kinds of talk therapy, regular exercise, a good social life, and a healthy sleep routine. You should be doing "all the things we know you can do to protect yourself as much as possible," Sanacora says.
Show Sources
Photo Credit: Philippe Garo / Science Source
SOURCES:
Gerard Sanacora, PhD, MD, director, Yale Depression Research Program; George D. and Esther S. Gross professor of psychiatry, Yale School of Medicine; co-director, Yale New Haven Hospital Interventional Psychiatry Service, Connecticut.
Susan Conroy, MD, PhD, assistant professor of psychiatry, Indiana University School of Medicine; medical director, Electroconvulsive Therapy (ECT) Service, IU Health Methodist Hospital; medical director, Transcranial Magnetic Stimulation (TMS) Service, Goodman Hall Adult Outpatient Psychiatric Clinic.
Frontiers in Psychiatry: "Associations Among Monoamine Neurotransmitter Pathways, Personality Traits, and Major Depressive Disorder."
Drugs Today: "Brexanolone for the treatment of patients with postpartum depression."
FDA: "FDA approves first treatment for post-partum depression."
Yale Medicine: "How New Ketamine Drug Helps With Depression."
Johns Hopkins Medicine: "Esketamine for Treatment-Resistant Depression," "Frequently Asked Questions About TMS."
JAMA Psychiatry: "Effects of Psilocybin-Assisted Therapy on Major Depressive Disorder," "Modern Electroconvulsive Therapy: Vastly Improved yet Grated Underused."
Experimental and Therapeutic Medicine: "Efficacy of electroconvulsive therapy as a potential first-choice treatment in treatment-resistant depression."
Cleveland Clinic: "Deep Brain Stimulation."
The New England Journal of Medicine: "Trial of SAGE-17 in Patients with Major Depressive Disorder."
