Corneal Flash Burns Overview
Eyes, particularly the cornea (the clear window of tissue on the front of the eyeball), can be damaged easily by exposure to ultraviolet radiation from the sun and from other sources of ultraviolet light, such as a welder's arc, a photographer's flood lamps, a sun lamp, or even a halogen desk lamp.
The cornea takes the brunt of the damage if proper eye protection is not worn, such as dark glasses or goggles while skiing in bright sun. A corneal flash burn (also called ultraviolet keratitis) can be considered to be a sunburn of the eye surface.
- The cornea covers the iris (the colored part of the eye), focuses light on the retina, and protects deeper structures of the eye by acting like a windshield to the eye. The corneal surface consists of cells similar to those in the skin. The cornea is normally clear.
- Corneal damage from a corneal flash burn or from a disease may cause pain, changes in vision, or loss of vision.
Corneal Flash Burns Causes
Radiation damage to the cornea leading to a flash burn can be caused by ultraviolet light from various sources:
- Sunlamp in a tanning salon
- Reflection of the sun off the snow at high elevation (snow blindness)
- Photographer's flood lamp
- Lightning that strikes close to you
- Halogen lamp
- Welding torch
- Direct sunlight
- Solar eclipse
- Reflection of sunlight off water
Corneal Flash Burns Symptoms
Any time from 3-12 hours after overexposure to ultraviolet light, you may begin to notice symptoms:
- Pain that can be mild to very severe
- Bloodshot eyes
- Light sensitivity
- Excessive tearing
- Blurry vision
- Sensation of a foreign body in the eye
In most cases, both eyes are involved, although the symptoms may be worse in the eye that received more ultraviolet radiation. This is very different from a corneal abrasion due to an injury, where, ordinarily, only one eye is involved.
When to Seek Medical Care
Because the eyes are very sensitive to disease and damage, any blurred vision, change in vision, or worsening eye pain needs to be evaluated by your eye doctor.
If you are unable to discuss your situation with an eye doctor and you have changes in your vision, have blurry vision, see flashing spots or light, or have worsening eye pain or pain with the movement of your eyes, then you need to go to a hospital's emergency department for an evaluation.
Questions to Ask the Doctor
- Have you found a reason for my symptoms?
- Will I develop any scarring or permanent visual loss from a corneal flash burn?
- Is there anything I should do to prevent this injury from happening again?
- What can I expect to feel once the numbing eye drops have worn off?
- When may I resume my regular activities?
Exams and Tests
To make the diagnosis, your eye doctor or the physician in the hospital's emergency department will take a history, examine your eyes, and discuss recent exposure you may have had to ultraviolet light.
- Your eyelids, pupils, back of the eye, and vision are checked.
- Your eye doctor looks at the surface of your eyes using special equipment, such as a slit lamp, made especially for examining the eye's surface.
- A numbing eye drop to allow your eye to be examined and a painless dye called fluorescein may be put onto your eye to aid in the examination. The stain temporarily makes your eye look yellow but goes away after a few minutes. A special blue light is then used to evaluate the stained eye to determine if corneal damage is present. A damaged cornea, coupled with a history of ultraviolet light exposure, confirms the diagnosis of radiation eye burns or corneal flash burns.
Corneal Flash Burns Treatment
Self-Care at Home
- If you are experiencing eye pain and wear contact lenses, remove them immediately.
- Sunglasses may help if your eyes are sensitive to light.
- Over-the-counter artificial tears or lubricants may improve the discomfort in your eye.
Medical Treatment
In some cases, the eye may be patched to aid in healing and pain control. Wearing sunglasses may also help relieve the pain.
Medications
Treatment may involve pain medicine, antibiotic medication, or medicine to enlarge (dilate) the pupils. Depending on your situation, any combination of these treatments, or none of them, may be indicated.
- Topical, antibiotic eye drops or ointment made specifically for the eye may be recommended to prevent infection in the damaged cornea. Some eye doctors may use steroid eye drops to reduce inflammation and to avoid potential scarring.
- A short-acting drug may be used to paralyze the ciliary muscles of the eye, resulting in a fixed and dilated pupil. This drug would dilate your eyes and be used to rest the muscles of the eyes, as well as to decrease pain from eye muscle spasms.
- Oral medication can be used for pain control. Pain medication may be an anti-inflammatory pain medicine, such as ibuprofen (Advil , Motrin) or naproxen sodium (Anaprox). Other pain medicines, such as acetaminophen (Tylenol), may also be used; rarely, stronger agents may be used.
- Topical anesthetics for the eye should never be used because they can slow the healing of the cornea and lead to ulcer formation.
Next Steps
Follow-up
In most cases, you will need to follow up with your eye doctor in 24-48 hours for a reevaluation of the eyes and to make sure that the corneas are healing.
Prevention
To prevent damage to the cornea, wear protective eyeglasses that are coated to protect the cornea from ultraviolet light. The labels on the sunglasses indicate the level of ultraviolet A (UVA) and ultraviolet B (UVB) protection.
Protective eyeglasses would include:
- Sunglasses that protect against UVA and UVB radiation
- Ski goggles or "glacier glasses," particularly at high elevations
- Totally dark glasses for tanning beds
- A welder’s mask when welding
Outlook
The cornea repairs itself rapidly and usually heals without leaving any scars. In most cases, healing takes place in 1-2 days if you follow all instructions and protect your eyes from further damage.
However, some complications, such as infection, may not show up right away. Thus, it is important to return for a recheck with your eye doctor when it is scheduled.
For More Information
American Academy of Ophthalmology
655 Beach Street
Box 7424
San Francisco, CA 94120
(415) 561-8500
Multimedia
Media file 1: An eye doctor examines a patient's eye with a slit lamp.
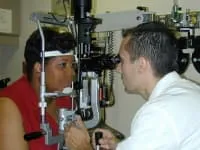
Media type: Photo
Synonyms and Keywords
corneal flash burns, welder’s arc burn, ultraviolet keratitis, snow blindness, flash burn, radiation eye burn, superficial punctuate keratitis, sunburn in the eye, actinic keratitis

