- Eye & Vision Basics
- Pediatric Eye Conditions
- Common Eye Problems
- Common Vision Problems
- Vision Correction
- Eye Diseases & Conditions
- Retinal Conditions
- Optic Nerve Problems
- Low Vision & Vision Loss
- View Full Guide
Reasons for Droopy Eyelids


Aging
The “levator” muscle holds up your eyelid. The skin and tissue around it stretch and get weaker as you age. That may make your eyelids droop slowly over time. You might not need treatment. But you can get surgery to raise your eyelid if you can’t see very well or don’t like how it looks. Skin can also hang over your eyelid. That’s called dermatochalasis, and it can look like ptosis. Your doctor should be able to tell the difference.
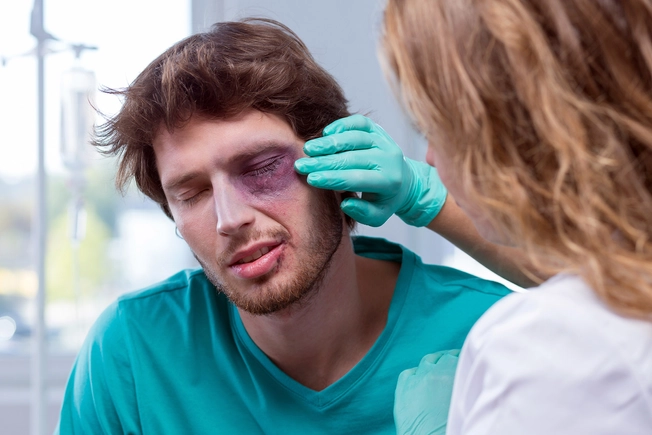
Eye Injury
You can accidentally hurt or weaken your levator muscle. It could happen if someone or something hits you in the eye. Wearing contact lenses for many years or rubbing your eye a lot can cause it, too. Tell your doctor if the drooping doesn’t get better on its own or gets worse over time. Surgery may help.
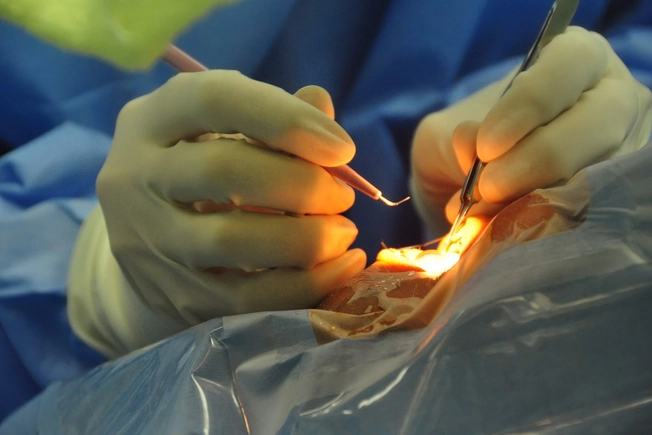
Eye Surgery
Your eye might droop after cataract, glaucoma, or LASIK surgery. Doctors aren’t sure why this happens. Some think the tool that holds your eyelid back during surgery may stretch or damage your eye muscles. Surgery can also make your eyelid swell. This kind of ptosis usually gets better on its own. Talk to your doctor if it hasn’t gotten better after 6 months.

You Were Born With Them
Some babies are born with one or two droopy eyelids. It happens when the muscle that holds up the eyelid doesn’t form the right way. Kids with ptosis might have less vision in the top part of their eye. They may tilt their head back to see better. Sometimes they get amblyopia, or “lazy eye.” Your doctor might suggest surgery to raise their eyelid.
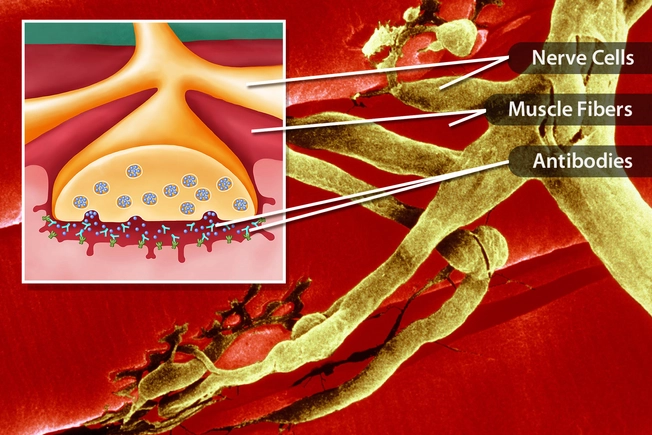
Myasthenia Gravis
This is when your immune system attacks and weakens the signal between your nerves and muscles by mistake. That includes the ones that control your eyelids, face, throat, and jaw. Your ptosis might get worse at night or when you’re tired. Drugs or surgery may help your muscles work better.
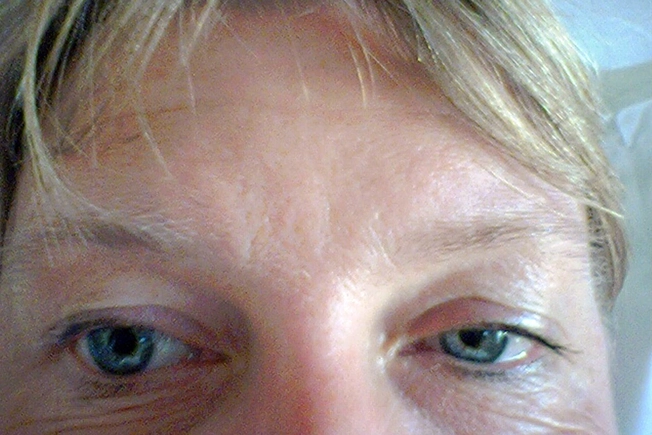
Horner Syndrome
This is when damage to certain nerve pathways makes your eyelid sag. The affected eye might have a smaller pupil, and part of your face might not sweat. Some people are born with Horner syndrome. But noncancerous (benign) or cancerous tumors, like ones in your brain, head, or lungs, can also damage these nerves. Your doctor will check for diseases that limit blood flow to your head and neck.
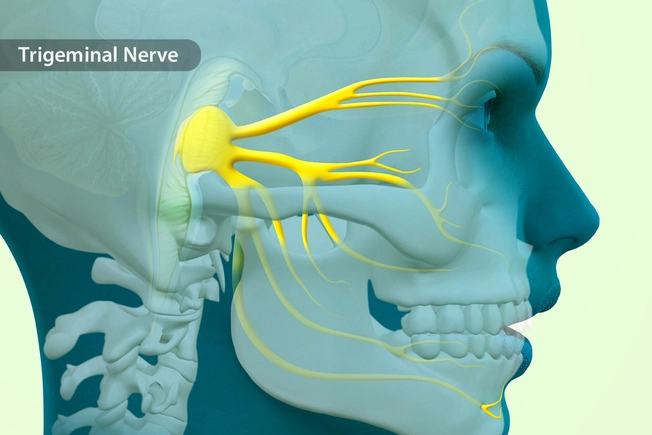
Serious Headaches
You might get symptoms of Horner syndrome if you have migraine or an issue with your trigeminal nerve. That’s a nerve that runs through your face and jaw. Your eye will probably go back to normal when the headache goes away. But sometimes it can sag in between attacks. Talk to your doctor about drugs or other treatments to manage the cause of your headaches. They’ll also rule out a more serious condition.
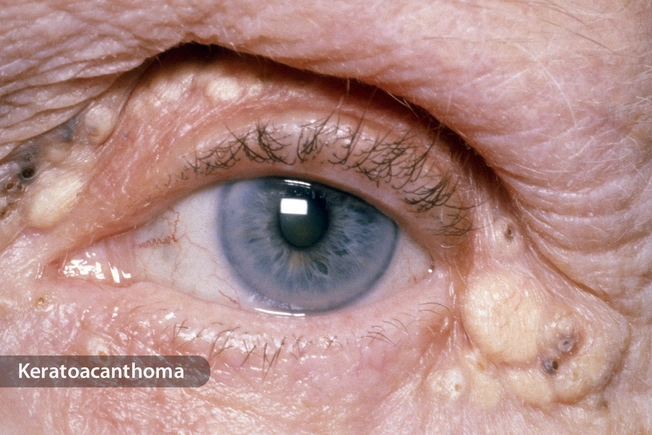
Eyelid Tumor
Your doctor might call this mechanical ptosis. That just means something is weighing your eyelid down. A tumor might grow on your eyelid if you have a genetic disorder called neurofibromatosis type 1 (NF1). It’s usually not cancerous, but you may need surgery or radiation treatment to get rid of it. There’s no cure for NF1.
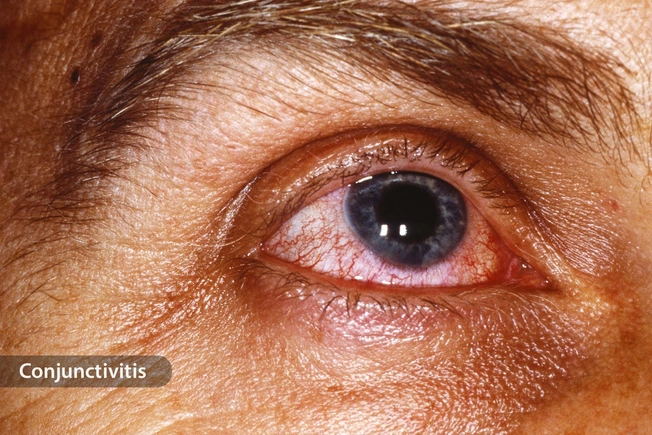
Eye Infection
Pinkeye (conjunctivitis) or styes can make your eye swell. Your eyelid will likely go back to normal as you heal. That might take 1-2 weeks or longer. You should get better on your own. Check with your doctor if your eye is swollen shut or you have pain, pus, or a fever. You might need antibiotics or surgery to drain the fluid. In the meantime, artificial tears or a warm or cool compress might help your eye feel better.
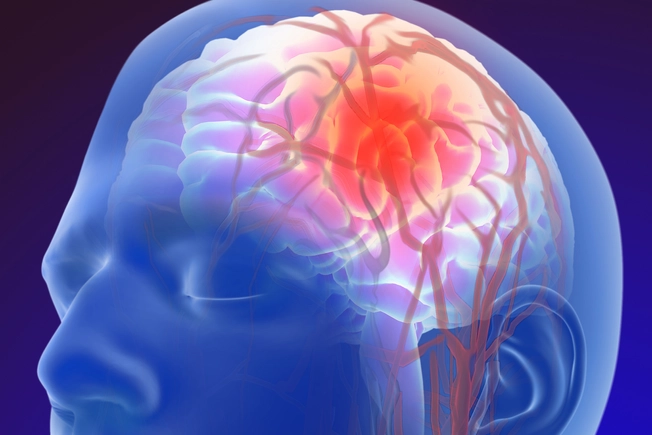
Stroke
Your brain can’t get enough oxygen and nutrients if a blood vessel bursts or is blocked by a clot. That causes a stroke, and it can make one side of your face -- including eyelids -- droop. Get help within 3 hours of first symptoms. Watch out for numbness/weakness, or trouble speaking, seeing, or walking.
To cut your odds of a stroke, exercise and eat well. Work with a doctor to manage diabetes, cholesterol, and blood pressure. And if you smoke, quit.
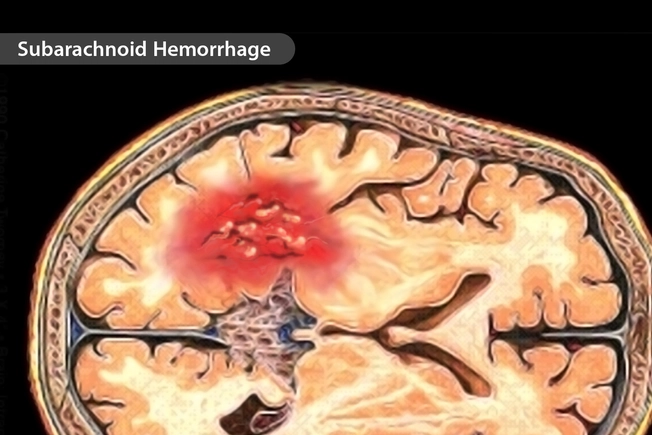
Bleeding in Your Brain
A brain aneurysm is a weak part of a blood vessel that can burst, causing a hemorrhagic stroke. This can trigger a subarachnoid hemorrhage. That’s when you bleed around your brain. It’s an emergency that can cause fainting or a seizure. Tell your doctor if you have terrible head or eye pain, vision changes, or weakness and numbness on a side of your body. They might be able to treat your aneurysm with surgery.
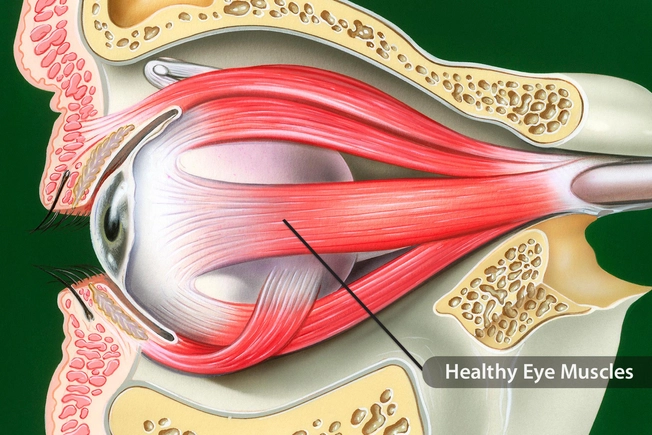
Muscle Problems
Droopy eyelids can be a sign of oculopharyngeal muscular dystrophy. That’s a muscle disease of your eye and throat. You’re born with it, but symptoms might not show up until after age 40. Both eyelids might sag. You might not be able to see very well, and tongue and throat problems may make it hard to eat. Surgery can help fix your ptosis. You might need occupational therapy or another surgery if other parts of your body are affected.
Diabetes
Over time, high blood sugar can damage blood vessels and nerves in and around your eyes. You might get a droopy eyelid along with double vision. That can happen with diabetic third nerve palsy. Symptoms sometimes get better when you manage your diabetes. But the doctor might suggest surgery if your ptosis affects your vision and lasts longer than 6 months.
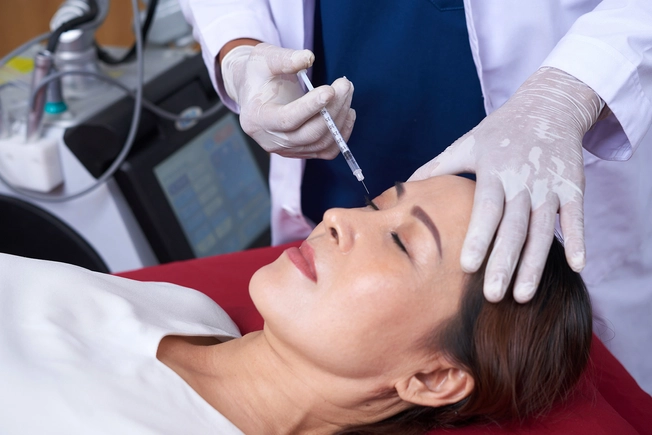
Botox
Botulinum toxin (Botox) can paralyze your muscles, like the ones that cause wrinkles. You might not have any problems with Botox. But it’s possible for the toxin to get into the muscle that controls your upper eyelid. Your ptosis should get better as it wears off, but apraclonidine eyedrops might help. Your doctor will help you decide what treatment is right for you.

Mitochondrial Myopathies
Genetic diseases can make it hard for mitochondria to work. That’s what powers most of the cells in your body. Your eyes and eyelids might get weak. It may cause mild vision problems in adults. Kids with mitochondria issues should get eye exams often. The doctor might give you nutrition supplements like creatine, carnitine, or coenzyme Q10 to help your mitochondria. More research is needed to know how well these supplements work.
IMAGES PROVIDED BY:
1) filadendron / Getty Images
2) KatarzynaBialasiewicz / Getty Images
3) nakornkhai / Getty Images
4) Stockbyte / Getty Images
5) Left to right: Don W. Fawcett / Science Source, Emily Ciosek / Science Source
6) Waster / Wikipedia
7) Claus Lunau / Science Source
8) Clinical Photography, Central Manchester University Hospitals NHS Foundation Trust, UK / Science Source
9) John Watney / Science Source
10) Lars Neumann / Getty Images
11) Catherine Twomey / Science Source
12) JOHN BAVOSI / Science Source
13) vitapix / Getty Images
14) DragonImages / Getty Images
15) Artem_Egorov / Getty Images
SOURCES:
American Academy of Ophthalmology: “What Is Ptosis?” “Can pink eye cause droopy eyelid?”
Practical Neurology: “Ptosis.”
Cleveland Clinic: “Ptosis: (Drooping Eyelid): Management and Treatment.”
Graefe’s Archive for Clinical and Experimental Ophthalmology: “Incidence and Risk of Ptosis Following Ocular Surgery: A Systematic Review and Meta-Analysis.”
Clinical Ophthalmology: “Ptosis after glaucoma surgery” “Neurofibromatosis: an update of ophthalmic characteristics and applications of optical coherence tomography.”
Seminars in Ophthalmology: “Ptosis After Cataract Surgery.”
NYU Langone Health: “Types of Ptosis.”
University of Iowa Health Care (EyeRounds.Org): “A Primer on Ptosis,” “Self-Resolving Ischemic Third Nerve Palsy.”
National Institute of Neurological Disorders and Stroke: “Myasthenia Gravis Fact Sheet,” “Mitochondrial Myopathy Fact Sheet.”
Genetics Home References (NIH): “Horner syndrome,” “Oculopharyngeal muscular dystrophy.”
Journal of Medical Case Reports: “Chronic persistent Horner’s syndrome in trigeminal autonomic cephalalgia subtypes and alleviation with treatment: two case reports.”
American Association of Neurological Surgeons: “Neurofibromatosis.”
CDC: “Conjunctivitis (Pink eye).”
Familydoctor.org: “Sty.”
American Stroke Association: “08 Ways to Help Prevent a Second Stroke.”
Columbia University Irving Medical Center: “Subarachnoid Hemorrhage.”
Cedars Sinai “Oculopharyngeal Muscular Dystrophy (OPMD).”
Mayo Clinic Heath System: “Diabetes and your eyes.”
Medicine (Baltimore): “Ptosis as the only manifestation of diabetic superior division oculomotor nerve palsy.”
American Family Physician: “Diplopia and Ptosis.”
Dermatologic Surgery: “Persistence of Upper Blepharoptosis After Cosmetic Botulinum Toxin Type A.”
Journal of the Neurological Sciences: “Apraclonidine in the Treatment of Ptosis.”