What Is Hand Osteoarthritis?
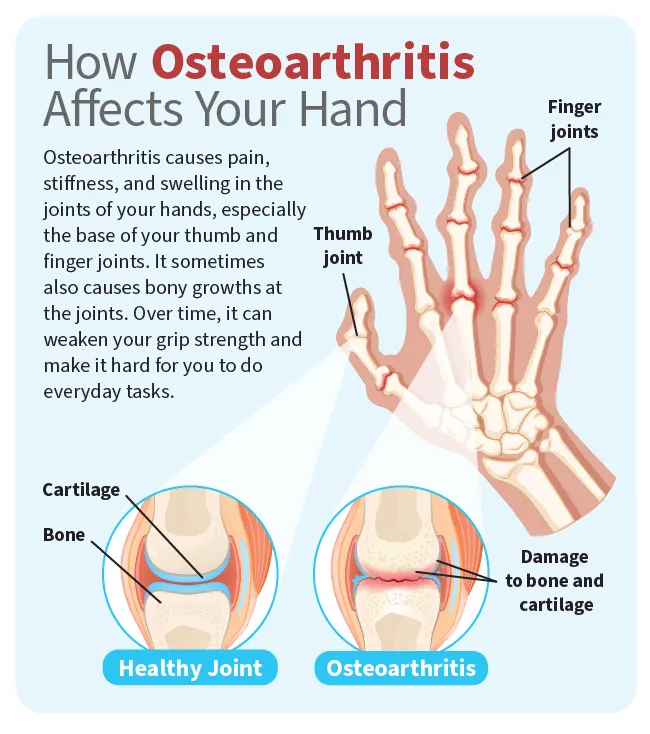
Hand osteoarthritis is swelling and irritation -- called inflammation -- that causes pain and stiffness in the joints of your hands. Osteoarthritis is the most common type of arthritis. It happens when the connective tissue (cartilage) at the ends of your bones wears away. This causes your bones to rub together.
There's no cure for hand osteoarthritis, but there are a lot of ways to protect your joints and feel better.
Without treatment, osteoarthritis gets worse over time. It’s important to get a diagnosis and a treatment plan as soon as possible.
Hand arthritis vs. tendonitis
Arthritis causes swelling, pain, and stiffness in your joints -- parts of your body where two bones meet. Tendonitis is inflammation of a tendon. A tendon is a thick, flexible band of tissue that connects your muscle to your bone. You can get tendonitis in your hand, wrist, and thumb, as well as other parts of your body. Because tendonitis causes pain near your joints, it is sometimes mistaken for arthritis.
Hand Osteoarthritis Stages
When you first start to feel symptoms of hand osteoarthritis, your joint pain and stiffness may be more noticeable in the morning. You may also feel the pain hours or the day after using your hand for heavy lifting or gripping. The pain may feel dull or like a burning sensation.
As osteoarthritis progresses and the cartilage in your joints wears away, your symptoms such as pain and stiffness will happen more often.
In later stages, joint pain may increase when you use your hands or when it rains. You may be woken at night from pain and have more difficulty using your hands for daily activities. Your affected joints may also swell from heavy use or appear larger due to new bone growths (nodes or spurs).
Where in the Hands Does Osteoarthritis Occur?
Osteoarthritis of the hands usually happens in three places:
- The base of your thumb, where it meets your wrist
- The joints closest to your fingertips
- The middle joint of a finger
There are different types of hand arthritis:
Basal joint arthritis (also called basal thumb arthritis or CMC arthritis) affects the basal joint at the base of your thumb. Your basal, or carpometacarpal (CMC), joint connects the bone of your thumb (metacarpal bone) to a bone in your wrist called the trapezium bone. Because you use your thumbs for most manual tasks, such as writing, cooking, and getting dressed, this condition can make it harder to perform daily activities.
The joint closest to the fingernail is called the distal interphalangeal (DIP) joint. The middle joint on your finger is called the proximal interphalangeal (PIP) joint. Osteoarthritis can also cause these joints to become painful, stiff, and bumpy.
Rheumatoid arthritis is usually caused by an autoimmune disorder such as lupus. Your immune system attacks the tissues in your body, including those in the joints of your hands, and causes painful swelling.
Post-traumatic arthritis is like osteoarthritis but is caused by an injury to the joint, such as a bone fracture or dislocation, or a torn ligament. It can affect joints in your hand or wrist. Unlike osteoarthritis, post-traumatic arthritis is more common in younger people.
Hand Osteoarthritis Causes and Risk Factors
The smooth cartilage on the ends of your bones helps cushion your joints and allows them to slide easily. But over time, the cartilage gets worn down. The bones rub against each other, causing the symptoms of osteoarthritis.
It's not clear what causes osteoarthritis. It's likely a combination of wear and tear and changes in the tissues themselves as you age. Certain things can make you more likely to have hand osteoarthritis:
- Age. The older you are, the higher your risk.
- Sex. Compared with men, women are twice as likely to get it.
- Ethnicity. Rates are lower in African Americans.
- Weight. People who have obesity have a higher risk.
- Injuries. It can develop after you've had a joint injury, even if the injury healed properly.
- Genetics. Your parents might have passed down a higher chance of osteoarthritis.
- Joint problems. This includes infections, loose ligaments, overuse, and joints that aren’t aligned the way they should be.
What causes flare-ups?
It's not always easy to know what causes your osteoarthritis to flare up. Some triggers could be:
- Stress
- Cold or wet weather
- Changes in barometric pressure, which is the air pressure in the atmosphere
- Repetitive motions involving your joint, such as grasping an object
- Overdoing an activity
- Medication changes
Hand Osteoarthritis Symptoms
The most common symptoms are pain and stiffness. Over time, they may get worse. The pain might become constant and sharper, and the stiffness could keep you from bending your finger joints all the way.
Hand osteoarthritis can cause other problems, such as:
- Clicking and cracking (crepitus). That's the sound of your joints rubbing against each other as the cartilage breaks down.
- Swelling and redness. This is a sign of inflammation around a joint.
- Weakness. Pain and joint damage can make it harder to do things such as turning doorknobs or lifting heavy pots.
Heberden’s nodes
Bumps and lumps are another common symptom. Heberden’s nodes are pea-sized bony growths that form on the joint closest to the fingernail, called the distal interphalangeal (DIP) joint.
When the cartilage in your joints breaks down, it causes bones to grind together. This leads to new bone growths at the joint. These growths are called nodes or spurs, which can cause symptoms such as:
- Pain, stiffness, and swelling
- Limited range of motion
- Difficulty doing tasks with your fingers, such as fastening buttons or opening jars
Bouchard's nodes
Bouchard's nodes are similar to Heberden's nodes, but they happen at the middle joints of your fingers.
Hand Osteoarthritis Diagnosis
Your doctor will look at your hands and ask about your symptoms and family history. You'll probably have X-rays, so your doctor can see the condition of your joints and cartilage. They also might do tests to rule out other causes of painful joints, such as rheumatoid arthritis.
Hand Osteoarthritis Treatment
Your doctor might recommend one or more of these nonsurgical treatments to ease pain, reduce stiffness, and make it easier to use your hand:
Pain medication. Over-the-counter medicines such as acetaminophen (Tylenol) and nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen can ease pain and swelling. Ask your doctor how often and how long to take these medications.
Splint, brace, or sleeve. These devices can hold your hand in a stable position to lessen pain. By limiting motion, they reduce strain and help keep your joints properly aligned. Make sure you are guided by a doctor or physical therapist on the right way to use a splint or brace and for how long. If you use one for too long, it can cause muscle weakness.
Hand therapy. An expert called a hand therapist can show you exercises and ways to do everyday tasks. For example, instead of carrying grocery bags with your hands, you might carry them over your forearm. The therapist can also show you stretching and strengthening exercises to help with pain and improve your range of motion.
Assistive devices. There are gadgets for people who have trouble using their hands due to injury or conditions such as arthritis. These include items to help you open jars, get dressed, or grab objects. An occupational therapist can teach you how to use these devices for everyday activities.
Steroid shots. An injection of a steroid into the joint may help relieve pain and reduce inflammation for several weeks or months. Your doctor will offer these only a certain number of times because they can have side effects such as infection and weakened ligaments.
Ice and heat. A cold pack can help ease pain and swelling. Heat (heating pad, warm compress) can reduce stiffness. Apply ice and heat for no longer than 20 minutes at a time.
Surgery
If other treatments haven’t worked or your symptoms have gotten worse, you and your doctor may consider surgery. Surgical options include:
Joint fusion. During this surgery (also called arthrodesis), your surgeon will use a plate and screws to hold the bones of your joint together. This will help get rid of your pain, but your joint will be less flexible and no longer bend as it did before.
Joint fusion is commonly used to treat osteoarthritis of the top (distal interphalangeal) and middle (proximal interphalangeal) joints of the finger as well as basal thumb arthritis (base of the thumb at the wrist).
Joint replacement. With a joint replacement (arthroplasty), your surgeon will replace your damaged joint with an artificial joint called an implant. The implant will be made of ceramic, plastic, metal, or a combination of these materials. Many of the joints in your hand and wrist can be replaced surgically with an artificial implant. If you receive a hinged finger implant, it will be flexible, but may not move the same way it did with your original joint.
Joint replacement is used to treat arthritis of the middle (proximal interphalangeal) joint or the knuckles.
Tendon transfer.Tendons are thick bands of tissue that connect muscles to bones. The tendons that control your fingers are attached to muscles in your palm and forearm. If your arthritis causes ongoing inflammation, it can cause a tendon to tear. If this happens, your surgeon can restore your hand function by using part of a healthy tendon to reattach your affected bone and muscle. Tendon transfer is also used to treat basal thumb arthritis.
Basal thumb arthritis may also be surgically treated by removing part or all of the wrist bone below your thumb joint.
Hand Osteoarthritis Home Remedies
These home treatments can help:
Exercises. Your doctor or physical therapist can show you what to do to improve your joints' strength and range of motion and to ease pain.
Assistive devices. Special pens, kitchen utensils, and other tools with big grips may be easier to use.
Ice or heat. Ice may reduce swelling and pain. Heat (using a warm washcloth or taking a paraffin bath) can loosen stiff joints.
Skin treatments. Medicated creams can give relief when you rub them on sore joints. Gels with NSAIDs also help.
Supplements. Many people take glucosamine and chondroitin supplements for osteoarthritis. Researchers are still looking into whether they help. Ask your doctor if they're OK to try.
Hand Osteoarthritis Prevention
There’s no one way to prevent osteoarthritis. Some lifestyle changes might lower your odds:
- Try not to do activities that involve the same motions over and over again. And if you can, skip the ones that might work your joints too much.
- Maintain a healthy body mass index (BMI).
- Eat a nutritious diet.
- Don't smoke.
- Exercise to make your joints and muscles stronger.
Takeaways
Osteoarthritis can affect various parts of your hand, from your fingers to your wrist. It causes pain and stiffness, making it difficult to do everyday tasks. There's no cure for osteoarthritis, but there are many treatments to help ease your pain and restore your hand function. Talk to your doctor about nonsurgical treatments including pain medication, exercise, injections, splints, and hot/cold therapy, as well as surgical options for long-term relief.
Hand Osteoarthritis FAQs
How do you treat osteoarthritis of the hands?
In the early stages of hand osteoarthritis, nonsurgical treatments can offer some pain relief, ease stiffness, and make it easier to use your hands for daily tasks such as getting dressed, writing, or cooking. These include pain medication, splints or braces, exercises or hand therapy, steroid injections, applying ice or heat, and using assistive devices to help you grip or open objects.
If these treatments don’t relieve your symptoms or if your hand osteoarthritis has advanced, you and your doctor may want to consider surgery. Surgical options include joint fusion, joint replacement, and tendon transfer.
What are the stages of hand osteoarthritis?
In the early stages of hand osteoarthritis, you may feel pain and stiffness in your fingers or hand, especially in the morning or several hours after heavy use. As the condition worsens and the cartilage in your joints wears away, you may feel pain more often.
In the later stages of hand osteoarthritis, your joint pain and stiffness may increase or happen more often, such as when you use your hands or when it rains. The pain and stiffness may also make it hard to sleep and harder to use your hands for daily activities. Your joints may also swell or appear larger due to new bone growths (called nodes or spurs).
What is the standard treatment for hand osteoarthritis?
There are several nonsurgical options for treating hand osteoarthritis. First, your doctor may recommend over-the-counter pain medication. Acetaminophen (Tylenol) and NSAIDs such as ibuprofen can help ease joint pain in your hand. There are other treatments you can do at home to help pain or stiffness such as applying cold or heat for 20 minutes at a time, using a splint or brace to keep the joint from moving, or doing exercises that your doctor or therapist provides.
What is the most common site of osteoarthritis in the hand?
Osteoarthritis most often affects the joint where the base of your thumb meets your wrist (carpometacarpal), as well as two joints of your fingers: the middle joint (proximal interphalangeal) and the top joint, closest to your fingernail (distal interphalangeal).

