Eczema is a common problem that causes the skin to become inflamed.
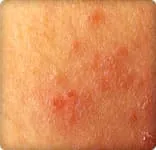
Eczema comes in many forms. But the different types of eczema tend to cause these symptoms:
- Itching. The itching can be intense. The damage to the skin during eczema is often due to scratching.
- Scaling. The surface of the skin can flake off, giving the skin a rough, scaly appearance.
- Redness. The affected skin may bleed and appear blotchy.
- Fluid-filled blisters. These can ooze and form crusts.
- Cracking. Severely affected skin may develop painful, deep cracks, also called fissures.
Depending on the cause, eczema may flare up and cause severe symptoms. But it can also become a chronic problem with less intense symptoms.
Here's a look at the types of eczema and their treatments.
Atopic Dermatitis
Atopic dermatitis is the most common form of eczema. It often affects people who also have:
Atopic dermatitis usually begins during infancy or childhood. But it can strike people at any age.
Symptoms of atopic dermatitis
Most often, it affects skin on the:
- Face
- Hands
- Feet
- Inner elbows
- Back of the knees
Over time, scratching the skin can cause it to become thick and red. Scratching can also create wounds that become infected.
Causes of atopic dermatitis
Irritants that can make symptoms of atopic dermatitis worse include:
- Soap
- Rough clothing
- Household chemicals
Foods, dust mites, and other allergy triggers can also make symptoms worse.
Treatments for atopic dermatitis include:
- Products to lubricate and moisturize the skin
- Steroid creams and ointments
- Drugs that control the immune system including crisaborole (Eucrisa), a nonsteroidal ointment that is used topically twice a day, abrocitinib (Cibinqo), dupilumab (Dupixent), and tralokinumab (Adbry), which are given as an injection every 2 weeks or so
- Antibiotics to treat infections
- Ultraviolet light, alone or with a drug called psoralen
Learn more about how to treat atopic dermatitis.
Contact Dermatitis
There are two types of contact dermatitis:
- Irritant contact dermatitis
- Allergic contact dermatitis
Causes of contact dermatitis
These types of eczema can develop after something damages the skin. These include chemicals and frequent hand washing.
Irritant contact dermatitis can start after touching a strong irritant one time or by coming into contact with the irritating substance repeatedly.
Contact dermatitis can also happen after a person touches an allergy-triggering substance, such as:
- Nickel
- Cosmetics
- Poison ivy
The hands are especially vulnerable to developing contact dermatitis. People can develop contact dermatitis even if they don't have atopic dermatitis.
Treatments for irritant contact dermatitis include:
- Moisturizers for the skin
- Steroid medications
Treatments for contact dermatitis from allergic triggers also include steroid drugs. These are rubbed on the skin or taken as a pill.
For either type of contact dermatitis, antibiotics may be necessary. Avoiding future contact with the irritant or allergy trigger is also important. Wearing gloves can help protect the skin on the hands, which are often affected. Read more on treatments for contact dermatitis.
Dyshidrotic Dermatitis
This type of eczema affects the hands and feet.
Symptoms of dyshidrotic dermatitis
The first symptom may be severe itching. Blisters may then appear, which give way a few weeks later to scaly patches. Sometimes deep cracks can appear on the hands or fingers.
This type of eczema may become chronic and painful.
Treatments include:
- Cool, wet compresses
- Steroid drugs that are rubbed onto the skin or taken by mouth
- Psoralen combined with ultraviolet A therapy
Causes of dyshidrotic dermatitis
Doctors aren’t sure what causes this form. Get more details on dyshidrotic eczema symptoms and causes.
Nummular Dermatitis
This type of eczema more often affects men than women. Men usually don't get their first outbreak before their mid-50s. Women tend to get it in their teen years or early adulthood.
Symptoms of nummular dermatitis
Nummular dermatitis causes coin-shaped red marks. The marks appear most often on the:
- Legs
- Backs of the hands
- Forearms
- Lower back
- Hips
Causes of nummular dermatitis
The cause of nummular dermatitis is unknown. But things that may raise the chance that an outbreak will strike include:
- Cold, dry air
- Exposure to chemicals such as formaldehyde
- Exposure to metals, including nickel
Treatments for nummular dermatitis include:
- Protecting your skin from scratches and other injuries
- Taking a lukewarm bath or shower, then applying a moisturizer to your skin
- Applying a steroid ointment to the rash
- Taking a steroid medication by mouth or injection that works throughout your body
- Taking antibiotics if an infection develops
See a photo of what nummular dermatitis looks like.
Neurodermatitis
Symptoms of neurodermatitis
This type of eczema often affects these areas:
- Back
- Sides or back of the neck
- Genitals
- Scalp
- Wrists
- Ankles
- Inside and behind the ear
Causes of neurodermatitis
People may scratch affected areas during the day without realizing it. They may also scratch while asleep.
Usually, neurodermatitis causes a skin outbreak that doesn't get any bigger. But the irritated skin can grow thick and deeply wrinkled. Infections may also develop in the irritated areas.
The main treatment for this type of eczema is to stop scratching it. In the meantime, steroid medicines that are rubbed onto the skin can help treat symptoms. Dupixent, an injectable, is approved to treat neurodermatitis.
When neurodermatitis affects the scalp, it can be harder to treat. In these cases, you may need to take the steroid medication prednisone by mouth.
See a photo of what neurodermatitis looks like.
Seborrheic Dermatitis
This type of eczema is better known as dandruff.
Symptoms of seborrheic dermatitis
In infants, it affects the scalp. In adults, it also often affects these areas:
- Eyebrows
- Sides of the nose
- Area behind the ears
- Groin
- Center of chest
Seborrheic dermatitis causes skin to fall off in flakes.
Causes of seborrheic dermatitis
The condition may be due to an overgrowth of a type of yeast that normally lives in these areas, as well as an overgrowth and rapid shedding of cells on the scalp. It may be especially hard to treat in people whose immune systems aren't working properly, including people with AIDS .
Treatments vary between infants and people with the condition later in life. The treatments include:
- Shampoo containing salicylic acid, selenium sulfide, zinc pyrithione, or coal tar
- Antifungal treatments that are rubbed onto affected areas
- Steroid lotions
View a slideshow for an overview on seborrheic dermatitis.
Stasis Dermatitis
This type of eczema can develop in people when the veins in their lower legs don't properly return blood to their heart.
Symptoms of stasis dermatitis
Stasis dermatitis can start quickly, causing weeping and crusting of the skin. Over time, this type of eczema can cause the skin to develop brown stains.
Treatments include:
- Steroid creams or ointments
- Creams or lotions that lubricate the skin
- Moist compresses
- Antibiotics to treat infections
- Elevating the legs
- Compression stockings
Causes of stasis dermatitis
This type of eczema can develop in people when the veins in their lower legs don't return blood to their heart the way they should. Learn more about stasis dermatitis causes and symptoms.

