What Are Cardiovascular Diseases?
Cardiovascular diseases are conditions that affect the structures or function of your heart, such as:
- Abnormal heart rhythms, or arrhythmias
- Aorta disease and Marfan syndrome
- Congenital heart disease
- Coronary artery disease (narrowing of the arteries)
- Deep vein thrombosis and pulmonary embolism
- Heart attack
- Heart failure
- Heart muscle disease (cardiomyopathy)
- Heart valve disease
- Pericardial disease
- Peripheral vascular disease
- Rheumatic heart disease
- Stroke
- Vascular disease (blood vessel disease)
Cardiovascular disease is the leading cause of death in the U.S. It’s important to learn about your heart to help prevent it. If you have it, you can live a healthier, more active life by learning about your disease and taking care of yourself.
Types of cardiovascular disease can have various causes, so it’s important to know the difference.
Abnormal Heart Rhythms
The heart is an amazing organ. It beats in a steady, even rhythm, about 60 to 100 times each minute. That's about 100,000 times each day. Sometimes your heart gets out of rhythm. Your doctor calls an irregular or abnormal heartbeat an arrhythmia. An arrhythmia (also called a dysrhythmia) can bring on an uneven heartbeat or a heartbeat that is either too slow or too fast.
Aorta Disease and Marfan Syndrome
The aorta is the large artery that leaves your heart and brings oxygen-rich blood to the rest of your body. These two conditions can cause the aorta to widen or tear. This raises the chance of things like:
- Atherosclerosis (hardened arteries)
- High blood pressure
- Connective tissue disorders that can weaken your blood vessel walls, such as scleroderma, osteogenesis imperfecta, Ehlers-Danlos syndrome, and polycystic kidney disease
- Injury
If you have aorta disease, you’ll need a team of specialists and surgeons to take part in your treatment.
Cardiomyopathies
This is the term for diseases of the heart muscle. They’re sometimes simply called enlarged heart. People with these conditions have hearts that are unusually big, thick, or stiff. Their hearts can’t pump blood as well as they should. Without treatment, cardiomyopathies get worse. They can lead to heart failure and abnormal heart rhythms.
Cardiomyopathy may sometimes run in families, but it can also be caused by high blood pressure, diabetes, obesity, metabolic diseases, or infections.
Congenital Heart Disease
This is a problem in one or more parts of the heart or blood vessels. It happens before birth.
About 8 out of every 1,000 children get it. They may have symptoms at birth, but some people with it don’t have symptoms until childhood or even adulthood.
In most cases, we don't know why it happens. Genes may play a role, or it can happen if a baby is exposed to viral infections, alcohol, or drugs before it’s born.
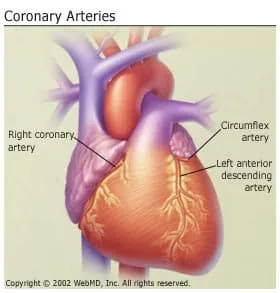
Coronary Artery Disease
You may hear this called CAD. It’s when plaque builds up and hardens the arteries that give your heart vital oxygen and nutrients. That hardening is also called atherosclerosis.
Deep Vein Thrombosis and Pulmonary Embolism
Blood clots can form in your deep veins, usually in your legs. This is deep vein thrombosis (DVT). They can break loose and travel through your bloodstream to your lungs, where they can block blood flow. This condition is called pulmonary embolism. It’s life threatening and needs immediate medical attention.
You might be at higher risk of DVT because of your genes or family history. Other things that can increase risk include sitting for a long time, like in a car or on a plane; long-term bed rest; pregnancy; and using birth control pills or hormone replacement.
Heart Failure
This term can be scary. It doesn’t mean your heart has "failed," or stopped working. It means your heart doesn’t pump as strongly as it should. This will cause your body to hold in salt and water, which will give you swelling and shortness of breath.
Heart failure is a major health problem in the United States, affecting more than 6.7 million people. It is the leading cause of hospitalization in people older than 65.
The number of people diagnosed with heart failure is projected to rise to 8.5 million Americans by 2030, according to the American Heart Association.
Heart Valve Disease
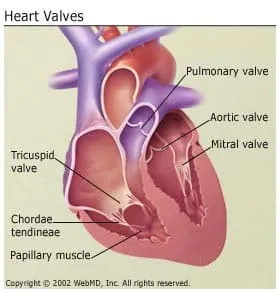
Your valves sit at the exit of each of your four heart chambers. They keep blood flowing through your heart.
Sometimes, there are problems with these valves. Examples of heart valve problems include:
Aortic stenosis. Your aortic valve narrows. It slows blood flow from your heart to the rest of your body.
Mitral valve insufficiency. Your mitral valve doesn’t close tightly enough. This causes blood to leak backward, leading to fluid backup in the lungs.
Mitral valve prolapse. The valve between your left upper and left lower chambers doesn’t close right.
Pericarditis
This condition is rare and means the lining surrounding your heart is inflamed. An infection often causes this.
Rheumatic Heart Disease
This happens when rheumatic fever, an inflammatory disease that’s most common in children, damages your heart valves.
Rheumatic fever starts with untreated strep throat and can affect many parts of your child’s body. If your doctor thinks your child may have had rheumatic fever, they’ll do a physical exam and give tests including X-rays and EKGs to look for heart damage.
Stroke
Strokes happen when something slows or blocks blood flow to your brain. Your brain can’t get the oxygen and nutrients it needs, and brain cells start to die. When blood can’t get to the part of your brain that controls a certain function, your body doesn’t work like it should.
A stroke can happen because of a blocked artery or a leaking or burst blood vessel. It needs immediate treatment to limit brain damage and other complications.
Stroke is the leading cause of disability and one of the top causes of death in the United States.
Other Vascular Diseases
Your circulatory system is made up of the vessels that carry blood to every part of your body.
Vascular disease includes any condition that affects your circulatory system. These include diseases of the arteries that go to your legs (peripheral vascular disease) and slow blood flow to your brain, causing strokes.
Cardiovascular Disease Treatments
Treatments for cardiovascular diseases can differ by the type of condition. Yours may include:
- Changing parts of your lifestyle like your diet, exercise, and alcohol and tobacco use
- Medications, including ones that treat risk factors like blood pressure or cholesterol or to break up clots
- Medical procedures like having a balloon or stent placed in your blood vessel, heart valve surgery, or coronary artery bypass graft surgery.