How to Treat Atrial Fibrillation

Determining Treatment for Afib
Your irregular heartbeat means blood doesn't flow as well as it should, and clots may form inside your heart. If one of those travels to your brain, it can cause a stroke. Your doctor may recommend medications but your course of treatment depends on your age, your symptoms and how often they occur, how long you have been in AFib, any other health problems you have, and if you have already had a stroke.
Blood Thinners
To help lower the chances of clots, your doctor may prescribe a more powerful blood thinner called an anticoagulant, especially if you have high blood pressure, diabetes, or heart failure. The most common is warfarin (Coumadin). It can cut your risk of stroke, but you'll have to get your blood tested often, and you'll have to be careful to avoid cuts or other injuries. Some foods can make warfarin less effective, too. If you need a procedure, dental work, or surgery, it might be necessary to stop the blood thinner. It's important to let all your doctors know you are taking a blood thinner just in case.

Other Blood Thinners
Newer anticoagulants including apixaban (Eliquis), dabigatran (Pradaxa), edoxaban (Lixiana, Savaysa), and rivaroxaban (Xarelto) also reduce the risk of stroke. You don't have to have regular blood tests when you take them. Plus, food doesn't affect how well they work. But you still could have problems with bleeding.

Slow Down Your Racing Heart
When your heart is beating too fast, medicine can slow it down and lessen the strain on your heart muscle. Getting the rate below 100 beats per minute can help you feel stronger. To do that, doctors often prescribe either beta-blockers or calcium channel blockers, depending on your health.
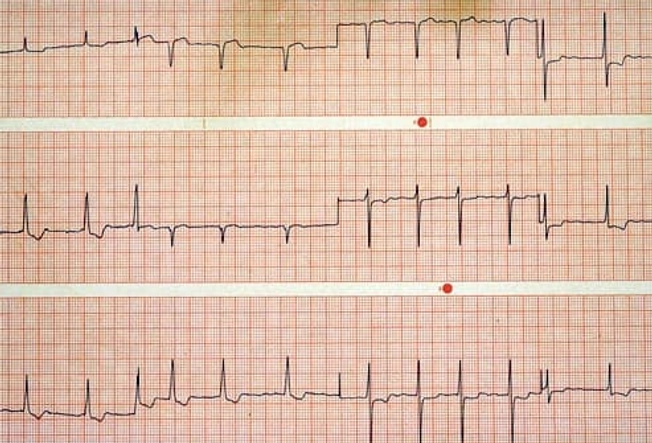
Reset an Irregular Heart Rhythm
Some people with AFib need electrical cardioversion to "reset" their heart's rhythm. While you're under mild anesthesia, a doctor uses patches or paddles to gently shock your heart.
Your doctor might want to do an ultrasound first to check for clots in your heart. If you have one, you may need to take blood thinners for a few weeks both before and after your procedure.

Heart Reset With Anti-arrhythmics
About half of people who have electrical cardioversion get AFib again. So doctors sometimes prescribe medications called anti-arrhythmics to help keep your heartbeat regular. You'll need to check in with your doctor often, because they can cause side effects including heart rhythm problems.

Ablation
When drugs and electrical treatments aren't working, your doctor may suggest a procedure called ablation. While you're sedated, a cardiologist will insert a thin, flexible tube into a large blood vessel and guide it to the spot in your heart that's misfiring. They'll destroy the tissue there by heating or freezing it. Depending on what kind of ablation you have, you may need a pacemaker, too. Sometimes it takes more than one ablation for it to work, but it can get rid of the atrial fibrillation when it is a success.
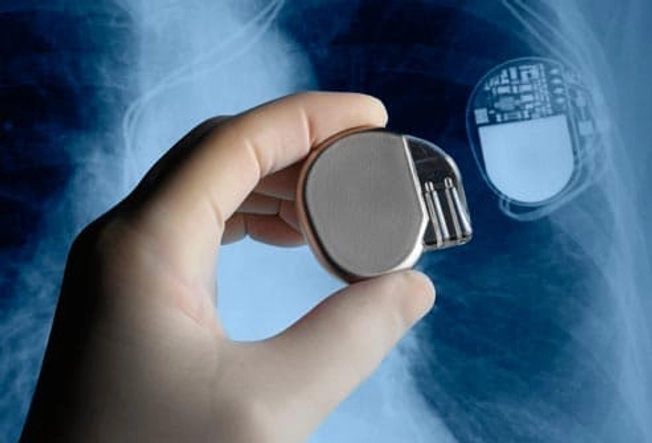
Pacemaker for a Steady Beat
This small, battery-powered device goes under your skin near your collarbone. It has wires that attach to your heart to keep it going when it gets too slow.
After surgery, you'll need to avoid pulling on the area, but you'll soon be able to get back to your usual activities. Most electronics like microwaves or phones won't bother your pacemaker, but some security systems and headphones can. You'll learn what to avoid and how to check your own pulse.
Heart Surgery
If medication and simpler procedures haven't helped, or if you have certain other heart problems, your doctor may recommend an operation called a Maze procedure. The surgeon makes precise cuts to scar the surface of the heart's upper chambers and interrupt the electrical signals that throw off your heart rhythm. Sometimes it can be done with only a tiny "keyhole" incision. If the surgery works, you should have fewer symptoms and be able to live normally. This surgery is often the last option for people whose atrial fibrillation is causing severe heart problems.

Lifestyle Changes
No matter how you treat your AFib, your daily habits can help your heart. Eat a heart-healthy diet. Cut back on the caffeine you drink. (Some people find that coffee, sodas, and tea make their symptoms worse.) Read medicine labels to check for decongestants -- especially in cold and cough medicines. Limit alcohol to no more than 1 drink a day if you're a woman and 2 if you're a man. Get regular exercise. And if you smoke, quit.
Talk to your doctor if your symptoms get worse.