Slideshow: Ulcerative Colitis Surgery -- What to Expect

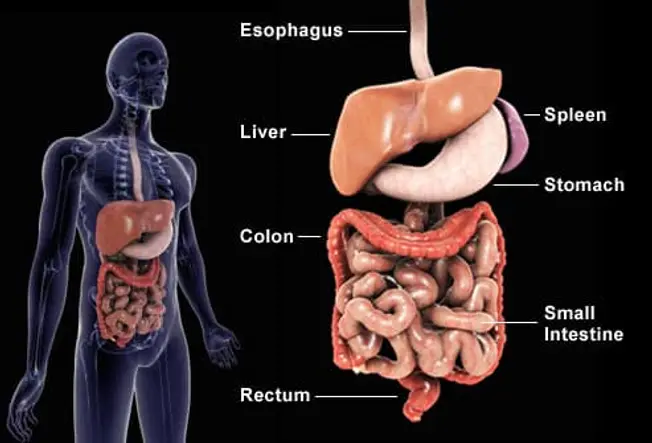
What Ulcerative Colitis Surgery Involves
A surgeon usually removes your colon (also called your large intestine) and rectum. Next they'll attach the lowest part of your small intestine to a hole they make in your torso to let waste leave your body and empty into an external bag. Another procedure creates an internal waste pouch that allows stool to be passed through the anus.
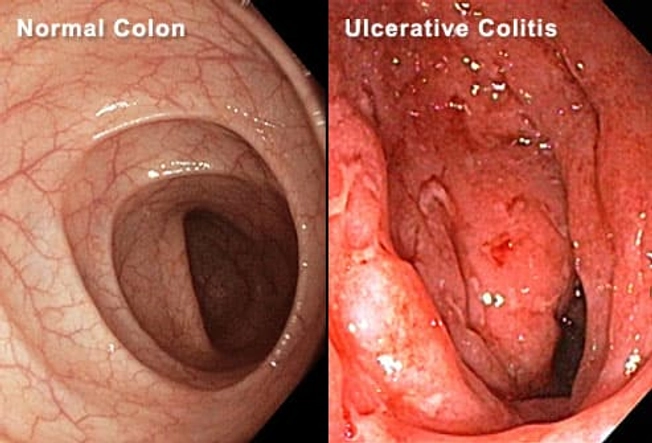
When Is Ulcerative Colitis Surgery Needed?
Your doctor may suggest surgery if you can't control inflammation and ulcers (right) with medication or other treatments. You may also need an operation if you get emergency complications of ulcerative colitis such as severe bleeding or tears in the colon. Some people choose to have surgery if their symptoms affect their ability to work and stay active.
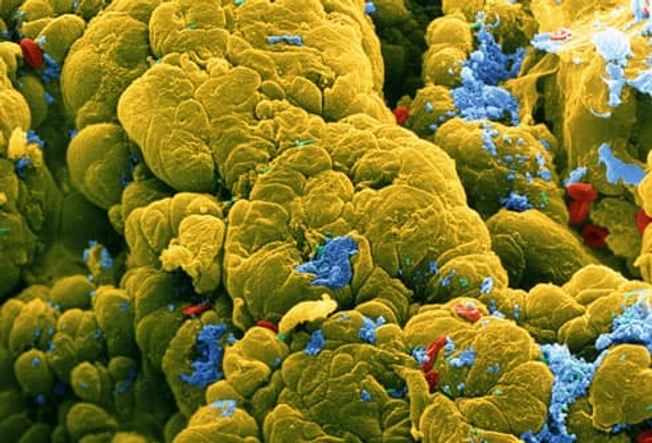
Surgery to Cure UC, Cut Colon Cancer Risk
The only way to cure ulcerative colitis is to get surgery to remove the diseased colon and rectum. You may also choose an operation if you want to cut your risk of colon cancer. Your chances of getting colon cancer go up if you have ulcerative colitis for 8 years or more or have a lot of colon damage. Your doctor may also suggest surgery if they find abnormal growth (shown in yellow in the image) during a checkup.
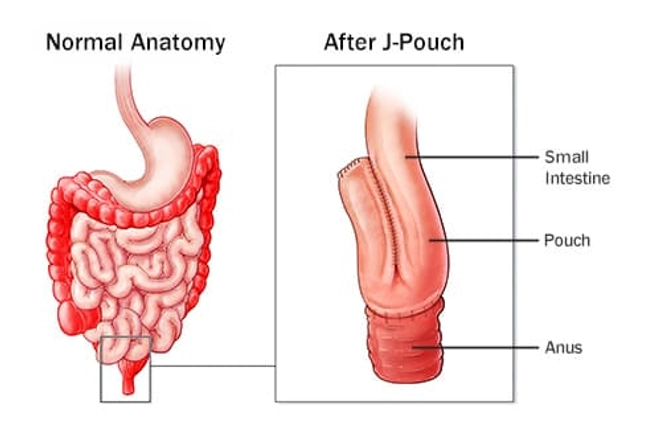
Ileal Pouch Anal Anastomosis: No Bags or Valves
The most common procedure for ulcerative colitis is pelvic pouch or ileal pouch anal anastomosis (IPAA). Your surgeon takes out your colon and rectum and fashions a new rectum, called a J-pouch, out of your small intestine. This type of surgery allows you to have bowel movements and use the bathroom. You won't need an ostomy bag. The procedure takes two separate surgeries about 2 months apart.
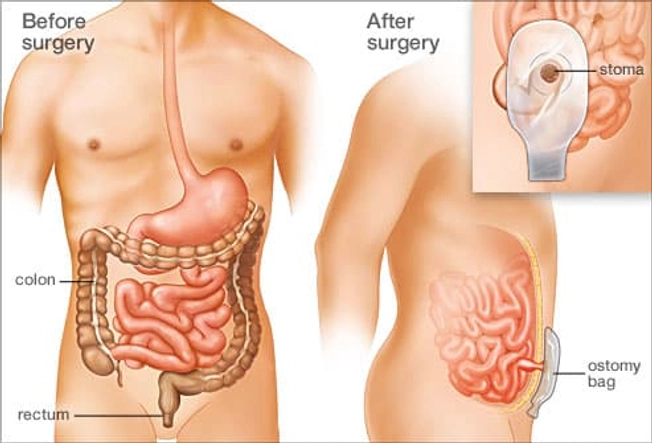
Proctocolectomy: Removal of Colon and Rectum
In this operation, also called a permanent or Brooke Ileostomy, your surgeon removes the colon and rectum and closes off the anus. They then make a hole in your belly, called a stoma. After surgery, waste will move from your small intestine, out the stoma, and into a plastic ostomy bag. While wearing a bag you'll still be able to work, be intimate, and play sports.
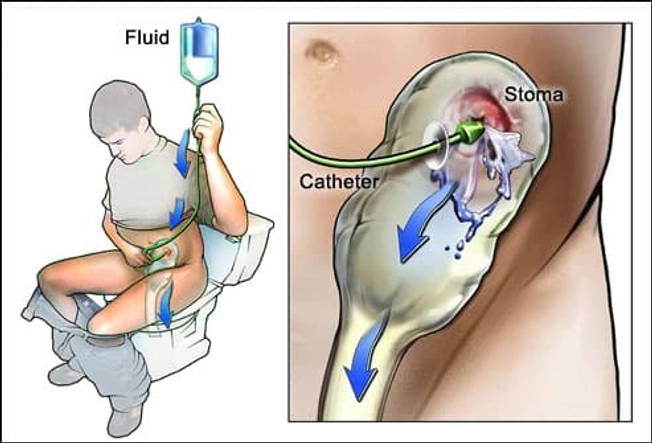
Caring for an Ostomy Bag
If you need this bag after your surgery you'll get advice from your medical team about how to care for it and the stoma. You can empty or throw out the bags when you need to. Irrigating the stoma can help you control the timing of bag changes. To prevent leaks, the pouch system that connects the stoma to the bag needs to be changed every 4 to 7 days. Call your doctor if you notice a change in color, bleeding, or swelling.
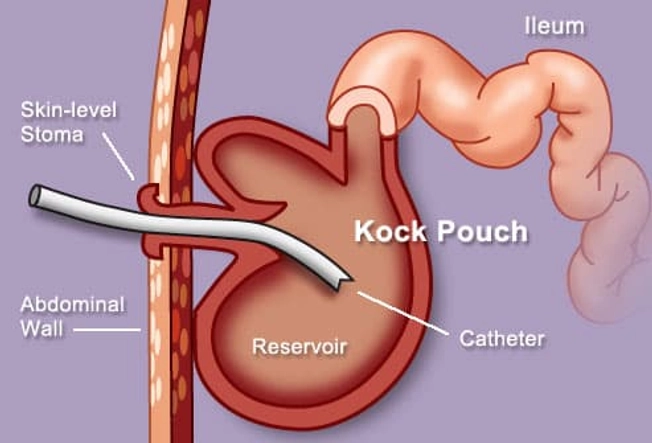
Continent Ileostomy: Waste Valve vs. Bag
The least common surgery for UC is continent ileostomy, also called the Kock pouch. Your doctor might suggest it if you can't have an IPAA or want to stop using an ostomy bag. During the procedure a surgeon removes your colon and rectum. They then use your small intestine to create a holding place (reservoir) for waste that will be drained from a valve in your abdomen.
Seek a Second Opinion
If your doctor recommends surgery to treat your ulcerative colitis, it's OK to get the advice of another doctor. A good first step is to seek treatment at a hospital that has experience in handling digestive disorders. Ask your doctor about:
- Treatment options
- What the procedure involves
- Risks, recovery, success rates
- Life after your surgery

Ulcerative Colitis Surgery Risks, Complications
If you have any of these symptoms, get medical help right away:
- Infection or pouch inflammation (pouchitis). Signs: Diarrhea, frequent bowel movements, stomach cramps and pain, fever, joint pain. Treatment: Antibiotics.
- Blockage or bowel obstruction. Signs: Cramping, nausea, vomiting. Treatment: IV fluids and fasting, sometimes surgery.
- Pouch failure. Signs: Fever, swelling, pain. Treatment: Surgery and permanent ileostomy.
Scheduled and Emergency UC Surgery
Most UC surgery can be arranged at time that's convenient for you. Try scheduling it while your symptoms are calm to cut the chances of complications.
The risks are higher when you have emergency surgery. You may need it if you get toxic megacolon -- a life-threatening condition when your colon rapidly swells and gas and bacteria build up inside. Get medical help right away if you have fever, belly pain, constipation, or swelling.

Life After Surgery
Ulcerative colitis surgery can help you have more control of your bowel movements and your life. But it's normal to have worries about how it will affect you and your body. Talk with your health care team before the operation so you know what to expect. And don't hesitate to join a support group or reach out to family, friends, and counselors to get the backing you need.