Colonoscopy is an outpatient procedure in which your large bowel (colon and rectum) is examined.
Your doctor may perform the procedure to diagnose and treat, when possible, certain diseases of the lower gastrointestinal (GI) tract, which includes the rectum and colon.
A colonoscopy may be used to screen for colon cancer and evaluate many problems, including:
- Long term, unexplained abdominal pain
- Anemia (low red blood cells)
- Blood in the stool
- Change in bowel habits
- Unexplained weight loss
Colonoscopy is often used to treat certain conditions:
- Bleeding from diverticula or other lesions can be treated by injecting medicine around them or by applying heat to cauterize -- or seal -- them.
- Polyps, some of which may be cancerous, can be removed using a lasso-like device through the colonoscope.
- Narrowed areas or strictures can often be dilated using a balloon.
How Do I Prepare for a Colonoscopy?
Before a colonoscopy, let your doctor know about any special medical conditions you have, including:
- Pregnancy
- Lung conditions
- Heart conditions
- Kidney Disease
- Allergies to any medications
- If you have diabetes or take medications that may affect blood clotting. Adjustments to these medications may be required before the colonoscopy. Never stop taking any medication without first consulting your doctor.
To prepare for the test, your doctor will prescribe dietary modifications. You may be asked to limit or eliminate high-fiber foods for a few days before the colonoscopy. You will also be asked to take laxatives by mouth to clean out the colon and may be put on a clear-liquid diet the day before the procedure.
Along with the dietary changes, your bowel must be further cleansed in order for the colonoscopy to be successful. Enemas or a special laxative drink may be given before the procedure. Follow your doctor's instructions on how to prepare for your colonoscopy.
Make sure you arrange for a driver to bring you home after a colonoscopy. Because you receive sedating medication during the procedure, it is unsafe to drive or operate machinery for about 8 hours after the procedure.
How Is a Colonoscopy Performed?
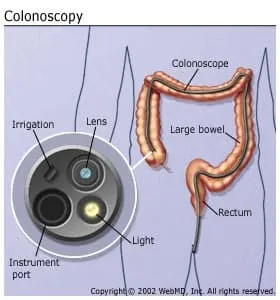
The colonoscopy should be performed by an experienced doctor and last approximately 30-60 minutes. You will receive medication to make you feel relaxed. You will be asked to lie on your left side on the examining table. During a colonoscopy, the doctor uses a colonoscope, a long, flexible, tubular instrument about 1/2 inch in diameter that transmits an image of the lining of the colon on a screen so the doctor can examine it for any abnormalities. The colonoscope is inserted through the rectum and advanced to the other end of the large intestine.
The scope bends, so the doctor can move it around the curves of your colon. You may be asked to change position occasionally to help the doctor move the scope. The scope also blows air into your colon, which expands the colon and helps the doctor to see.
You may feel mild cramping during the procedure. You can reduce the cramping by taking several slow, deep breaths during the procedure. When the doctor has finished, the colonoscope is slowly withdrawn while the lining of your bowel is carefully examined.
During the colonoscopy, if the doctor sees something that may be abnormal, small amounts of tissue can be removed for analysis (called a biopsy) and abnormal growths, or polyps, can be identified and removed. In many cases, colonoscopy allows accurate diagnosis and treatment without the need for major surgery.
What Happens After a Colonoscopy?
After you have a colonoscopy:
- You will stay in a recovery room for about 30 minutes for observation.
- You may feel some cramping or a sensation of having gas, but this usually passes quickly.
- You will need to have someone drive you home, as it is unsafe to drive or operate machinery for about 8 hours after the procedure (due to the sedative medication given).
- You can resume your normal diet.
Read your discharge instructions carefully. Certain medications, such as blood-thinning agents, may need to be avoided temporarily if biopsies were taken or polyps were removed.
Warning About Colonoscopy
Bleeding and puncture of the colon are rare but possible complications of colonoscopy. Call your doctor right away if you have:
- Excessive or prolonged rectal bleeding.
- Severe abdominal pain, fever, or chills.

