Support and Advice for Living With Myasthenia Gravis
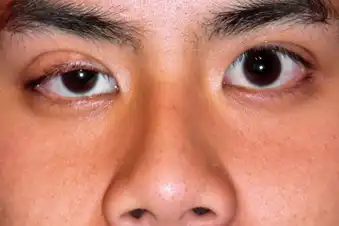
Take Time to Find the Right Treatment
Myasthenia gravis is a treatable condition in most people, but it can take time to find the best options for you. The first year can be the most challenging as we dial in treatments. But you and your doctor will work together over time to get it under control. We now have a number of treatment options available, and it’s important to find a strategy that works best for you.
Richard Nowak, MD, director, Yale Myasthenia Gravis Clinic, New Haven, CT.
Be Aware of Meds That Make MG Worse
It’s not clear why certain medications cause MG to get worse, but it’s important for you and your providers to be aware of them. You can find a list at myasthenia.org/MG-Community/Cautionary-Drugs. If you notice that your weakness is getting worse, inform your doctor.
Jeff Guptill, MD, director, Duke Early Phase Clinical Research Unit, Duke University Medical Center, Durham, NC.

Be Kind to Yourself
MG can make you feel weak, but you have the power to make a difference with self-care. This includes eating nutritious foods, being as active as you can, getting enough rest, and managing stress. Instead of trying to push through, allow time for rest. This might mean building rest times into your workday or pausing in the middle of climbing stairs.
Joan Wincentsen, executive director, Conquer Myasthenia Gravis, Elmhurst, IL.

Find the Right Support Team
Do your best to find a neurologist with experience. Seek out a specialized center, which may be at an academic medical center. Educate yourself from reliable sources like the Myasthenia Gravis Foundation of America and local MG foundations. The majority of patients can be treated successfully and are often the ones who don’t post online.
Henry J. Kaminski, MD, chair of neurology, George Washington University.

Exercise to Offset Weakness
Exercise has a strong benefit for MG. I ask my patients to exercise when they feel their best. For most, this tends to be in the morning. Consider taking pyridostigmine right before exercise and splitting exercise into shorter segments that engage different muscles. For instance, use the stationary bike and then switch to arm strengthening.
Rabia Malik, MD, neurologist, Rush University Medical Center, Chicago.

Track and List Tests and Meds
When I see new patients with MG, it can be challenging to track down test results and medications they’ve tried. This information is critical. Keep a list of tests and where they were done, even if you don’t have the results. Keep a list of medications, doses, and reasons for stopping them. This will make your time with a neurologist more productive.
Leeann Burton, MD, neuromuscular neurologist, Massachusetts General Hospital, Boston.

Think About Your Fatigue
Fatigue is common in MG. But it’s important to consider other potential causes that may need a different treatment. You may need evaluation for sleep apnea, which is common with conditions like MG. Low thyroid function, unbalanced diet, certain medications, and depressed mood are others that should be discussed with your doctor.
Madhu Soni, MD, associate professor of neurological sciences, Rush University Medical Center, Chicago.
Show Sources
IMAGES PROVIDED BY:
- Andrewya / Wikipedia
- Ingram Publishing / Thinkstock
- JGI / Jamie Grill / Getty Images
- Prykhodov / Getty Images
- (Left to right) zoranm / Getty Images, Jose Luis Pelaez Inc / Getty Images
- fizkes / Getty Images
- fizkes / Getty Images
SOURCES:
Richard Nowak, MD, director, Yale Myasthenia Gravis Clinic, New Haven, CT.
Jeff Guptill, MD, director, Duke Early Phase Clinical Research Unit, Duke University Medical Center, Durham, NC.
Joan Wincentsen, executive director, Conquer Myasthenia Gravis, Elmhurst, IL.
Henry J. Kaminski, MD, chair of neurology, George Washington University.
Rabia Malik, MD, neurologist, Rush University Medical Center, Chicago.
Leeann Burton, MD, neuromuscular neurologist, Massachusetts General Hospital, Boston.
Madhu Soni, MD, FAAN, associate professor of neurological sciences, Rush University Medical Center, Chicago.