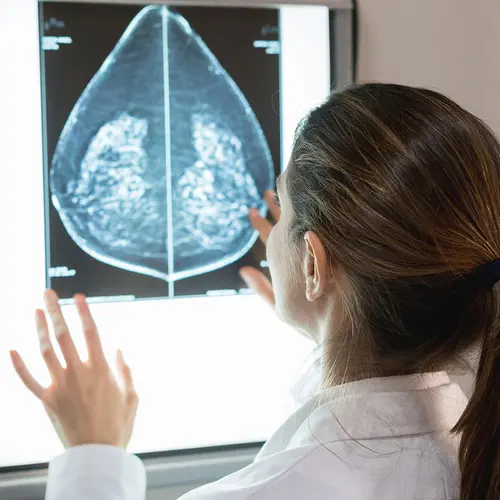
When it comes to breast cancer, Hispanic women or Latinas are more likely to be diagnosed at more advanced stages, which are harder to treat. They’re also more likely to have aggressive forms of the disease, such as triple negative and HER2-positive breast cancers.
Laura Fejerman, PhD, is among those working to increase breast cancer awareness and breast cancer screening among Hispanic women or Latinas. She is co-director of the Women’s Cancer Care and Research Program at the UC Davis Comprehensive Cancer Center. In 2014, Fejerman and her colleagues discovered a gene variant in Hispanic women or Latinas that was thought to be inherited from their Indigenous American ancestors. This protective variant seems to play a role in lowering breast cancer risk. But all Hispanic women or Latinas still need to keep up with regular breast cancer screening and get any lumps or breast changes checked out by a doctor.
Fejerman started “Tu Historia Cuenta,” or “Your Story Matters,” a breast cancer outreach program. It includes the importance of knowing your family history (though not all breast cancers run in families, having a family history of the disease is a risk factor) and talking about a subject that some find uncomfortable.
“If your grandma had cancer and your aunt had cancer and your cousin has cancer, that really matters for your own health,” Fejerman says.
“People don’t like telling members of the family that they have cancer or sharing with friends, because either they feel like it’s a burden to them or they feel embarrassed, especially if it’s a gynecological or breast cancer,” she says. “It kind of stays in a very private circle.”
“Your Story Matters” works with Spanish-speaking community health educators to teach women about breast cancers. In the past 2 years, through online and in-person classes, the program has reached about 1,300 Hispanic women or Latinas in California, Fejerman says. The program encourages mammography screening, as well as genetic screening and counseling if women have a significant family history of the disease.
Genetic screening can inform women if they have a higher risk of breast cancer. It’s not for everyone – typically, it’s recommended for at-risk people. But Hispanic women or Latinas are less likely to get this screening and counseling, Fejerman says, noting that they often don’t know about these services or don’t have insurance that covers it.
The Pandemic and Other Barriers
The COVID-19 pandemic “disproportionately affected the Hispanic community and other communities of color,” states the American Cancer Society’s report, “Cancer Facts and Figures for Hispanic/Latino People: 2021-2023.”
“A lot of people missed their routine screenings,” says Darcie Green, director of Latinas Contra Cancer (LCC), a service and advocacy group in San Jose, CA, that assists lower-income Hispanic women or Latina clients with cancer issues. LCC’s work includes providing health education to lower cancer risk and helping their clients get screening mammograms. (Screening mammograms are routine checks of the breasts. Diagnostic mammograms are done if there is a specific breast concern, like a lump.)
But it’s not just the pandemic. Underserved Latinas routinely face health disparities when seeking mammograms, Green notes.
Women with insurance who know how to navigate the health care system can easily book a mammogram appointment, drive to the facility, and get their screening. In contrast, many LCC clients face more hurdles, especially in an expensive urban area where it’s harder for families to survive economically.
They might not be able to afford unpaid time off from work to check on something they’re concerned about, Green points out. “They may be the breadwinner in their house. They may be caring for multiple generations in their household.”
Underserved Hispanic women or Latinas might also have trouble making an appointment if they don’t have a primary care doctor or OB/GYN. They may have other barriers like child care issues, long travel times, or reliance on public transit, Green says. To counter these barriers, LCC can help clients make appointments or arrange for transportation.
Finding Solutions
Women who are uninsured or under-insured can still get mammograms. In every state, the federally operated National Breast and Cervical Cancer Early Detection Program can help low-income, uninsured, or under-insured women ages 40-64 to get mammograms at little or no cost.
Mammograms, on their own, don’t diagnose breast cancer. A biopsy is needed for a diagnosis. But screening mammograms are an important part of early detection, which can be lifesaving because they may flag a cancer before it has spread. You may not be able to feel it yet.
Talking about breast health is also important. Discussing one’s breasts can be awkward, Green says. LCC tries to normalize the conversation and increase women’s awareness – not just about getting mammograms, but also about checking for lumps, puckering, redness, and other changes that require medical attention. “Knowing your breasts, knowing your body, is a really important thing to do,” Green says.