Dos and Don’ts After a Blood Clot

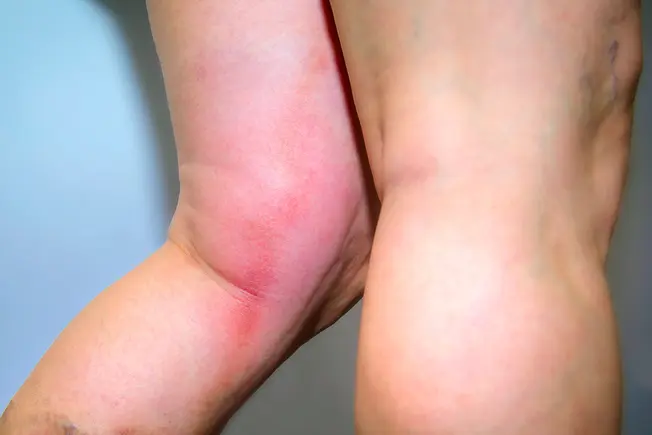
Do: Watch for Signs of Another One
If you’ve had a deep vein thrombosis (DVT) in one of your legs or arms, it’s sometimes normal for that limb to stay slightly swollen after treatment. After a clot in your lungs (a pulmonary embolism, or PE), you might feel mild pain or pressure in your chest. But watch out for new or worse pain, pressure, or cramping in your calf. That could signal a new DVT. Shortness of breath or fainting could be signs of another PE. If you have any of these, call 911 and get medical care right away.
Do: Know Your Odds
If you’ve had a blood clot before -- whether in your leg, arm, or lungs -- your chances of another one are higher. Your risk is also greater if you:
- Have cancer, an inflammatory disorder (like Crohn’s disease), a rheumatologic disorder (like rheumatoid arthritis), or a blood clotting disorder
- Are over 40
- Are overweight or obese
- Smoke, especially if you take birth control pills

Don’t: Hurt Yourself
Your doctor may prescribe clot-fighting drugs called anticoagulants, or blood thinners. These can make you more likely to bleed from small injuries, so it’s important to be careful when trimming your nails. You should wear gloves when you use sharp tools, and wear safety gear for sports and hobbies. Check with your doctor to see what other activities might not be safe for you.

Don’t: Eat the Wrong Foods
If you take the blood thinner warfarin (Coumadin, Jantoven) to ward off clots, you’ll need to watch what you eat. Vitamin K can affect how the drug works. So you have to be careful about the amounts of kale, spinach, Brussels sprouts, chard, or collard or mustard greens you eat. Green tea, cranberry juice, and alcohol can affect blood thinners, too. So ask your doctor about them.

Do: Get Moving
Exercises like walking or swimming can help you heal after a clot. They boost your blood flow and may make you feel better. If you had a pulmonary embolism, activities that get your heart pumping, like running or dancing, can make your lungs stronger. But talk to your doctor first about how much is right for you.

Do: Ask About Other Medicines You Take
If you take warfarin and certain other blood thinners, you shouldn’t take aspirin unless your doctor says it’s OK. That’s because it can raise your chances of major bleeding. Some antibiotics can keep these medicines from working the way they should. You should be careful with over-the-counter herbal supplements. A few, including ginseng, flaxseed, and fish oil, can also affect how blood thinners work.

Do: Share Information
Let all your doctors know if you’ve had a blood clot of any kind. And if you take blood thinners, tell your dentist when you make your appointment. Follow any instructions they give you to prepare for your visit.

Do: Ask About Compression Stockings
These special tight-fitting socks keep a certain amount of pressure on your leg, and that can help with blood flow after a DVT. Your doctor might also recommend them after a PE to boost your circulation.

Don’t: Sit Too Long
Try not to stay seated for more than 2 hours at a time -- get up and walk around regularly. If you had a DVT in one of your legs, don’t cross your legs when you sit down. That position can affect your circulation. Be mindful of this when you’re on long flights or driving for a long time.

Do: Travel Smart
If you’re in a car, take breaks often to stretch your legs. Deep knee bends can help get your circulation going. On a plane, try to move around the cabin once an hour. While you’re in your seat, flex your ankles to keep blood flowing. And drink plenty of water -- dehydration can make a clot more likely.

Do: Watch Your Weight
Obesity can strain your veins and make them weak. And if you have diabetes, make sure it’s well controlled. If it’s not, it can damage your blood vessels.

Don’t: Be Afraid to Ask for Help
It’s not unusual to feel anxious or depressed in the first few weeks after a DVT or PE. If those feelings are severe or they don’t go away, and you don’t feel like doing your normal activities, tell your doctor. They might be able to give you medication or a referral for talk therapy. A support group of people who’ve had the same problems may help, too.

Do: Be Careful During Pregnancy
Women who've had a DVT or PE have higher odds of another one when they’re pregnant. It’s important that they work with their doctors and watch their health closely. Even if they’ve stopped taking blood thinners, they might need to take them again, possibly as long as 6 weeks after delivery.