Slideshow: Stroke Rehab to Regain Arm Movement

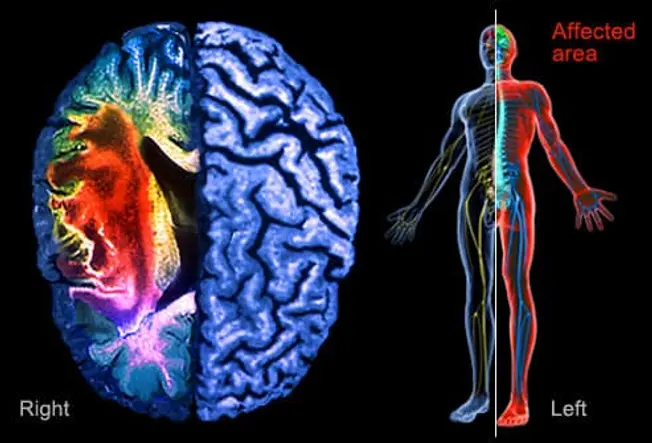
After a Stroke: Spasticity, Weakness, and Paralysis
Many people lose the use of their arm and hand after a stroke. Many also experience spasticity, uncontrollable muscle tightness, and stiffness, which make movement difficult. According to Stroke Connect, experts estimate that 20-50% of stroke survivors have some spasticity. Paralysis or weakness on one side of the body happens to about 80% of people. This usually happens on the opposite side of the body from where the stroke occurred in the brain. In rehab, you’ll work with a health care team to regain use of your arm.

Stroke Rehab Begins Right Away
Stroke rehabilitation begins once your condition has stabilized -- as soon as 24 to 48 hours after your stroke. Early, individualized therapy helps improve your chance of recovery. After leaving the hospital, you'll continue rehabilitation at an inpatient or an outpatient clinic, a nursing facility, or at home. While some stroke survivors recover fully, others will always have some disability.

Stretching Exercises Improve Range of Motion
Stretching exercises promote blood flow and make it easier to move your arm. Your therapist will start by gently stretching your hand, arm, and shoulder in a full range of motion. They can also show you how to use your unaffected hand to gently stretch the wrist, fingers, and thumb on your opposite hand.

Exercises to Help Rebuild Your Strength
Strengthening the muscles in your hand and arm will help improve your grip and ability to use your limb. An early arm exercise involves holding your weak arm with your strong arm and rocking it back and forth like a baby. As you gain strength and mobility, you can use squeeze balls, wrist weights, or hand weights to tone and build muscle.

Electrical Stimulation Therapy
A stroke interferes with your brain's ability to send messages to the nerves in your muscles. This can make it difficult to move and control your arm and hand. Electrical stimulation (ES) therapy is a safe way to stimulate the nerves that make your muscles contract. ES may help you regain control over your limb, improve muscle tone, and reduce pain and spasticity.

Constraint-Induced Movement Therapy
At some point in your recovery, your therapist may have you wear a restraining device on your functioning arm. You'll then be asked to use your affected hand and arm as much as possible to do repetitive tasks. This type of therapy is thought to increase brain plasticity -- the ability to repair itself. It may also help you regain function in your affected hand.

Practice Fine Motor Skills
Fine motor skills are small, precise movements you make with your hand and fingers. You can build this skill by tracing a design with a pen, shuffling cards, using a pegboard, or picking up small beans and putting them in a cup. As with all rehabilitation exercises, repetition is important to help retrain your brain. You need to practice daily, just as you would if you were learning to play the piano.

Spasticity Treatment: Oral Medications
Drug therapy for spasticity is often used in addition to physical exercises and stretching. Oral muscle relaxant medications help reduce large areas of spasticity by interfering with the nerve signals that cause muscles to contract. However, these medications may cause side effects such as drowsiness and weakness. Talk with your doctor or pharmacist to learn more.
Injections to Help Spasticity
For spasticity in a few select areas, you may benefit from a targeted therapy. A doctor can inject you with botulinum toxin, phenol, or both. Botulinum treatments block the release of nerve chemicals involved in muscle contraction. Phenol injections serve as nerve blocks in affected muscles, which helps with spasticity. Effects of both treatments usually last about three to six months. Depending on the medication, side effects can include pain, swelling, soreness, fatigue, and muscle weakness.
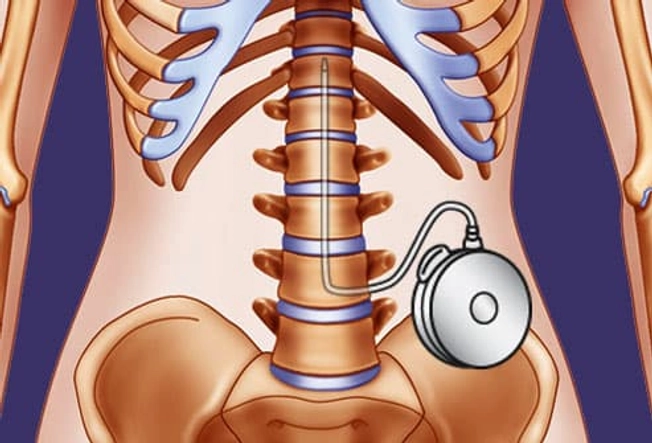
Intrathecal Baclofen Therapy for Spasticity
Another option may be intrathecal baclofen therapy. For this, a small pump is surgically implanted to administer muscle relaxant medicine to the spinal fluid. It can be useful when someone has severe spasticity or hasn't done well on oral medications. The pump uses a smaller amount of baclofen medication than when it's taken by pill, so it can cut down on some side effects. But there still are possible side effects and complications; talk to your doctor.

Occupational Therapy: Relearning Life Skills
One of the most important parts of your recovery is relearning daily living skills so that you can be mobile and independent. An occupational therapist (OT) will show you how to work around your disabilities so that you can change your clothes, take a shower on your own, cook, clean, and if possible, drive a car. Your OT will also help you set up your home to make it safer and easier to move around in.

Stick With Rehabilitation: Keep Setting New Goals
The first three months after a stroke are when most people make the biggest gains in their recovery. But by continuing to set new goals for yourself and exercising every day, you can see progress even years later. Practicing new skills helps the undamaged part of your brain take over new functions. Scientists are just beginning to understand how powerful our brains are, so it’s worth sticking with it.
IMAGES PROVIDED BY:
1) Photo Researchers Inc
2) Jose Luis Peleaz/Iconica
3) Image Source
4) Altrendo Images/Stockbyte
5) Andersen Ross/Digital Vision
6) Steven L Wolf, Ph.D./Emory Center for Rehabilitation Medicine
7) John Greim/Photo Researchers Inc
8) Bruce Ayres/Stone
9) Christine Balderas/iStock Exclusive
10) BSIP/Photo Researchers Inc
11) Simon Fraser/Brampton Day Hospital, Cumbria / Photo Researchers, Inc
12) Manchan/Photodisc
REFERENCES:
American Stroke Association: "Spasticity," "Functional Electrical Stimulation," "Constraint-Induced Movement Therapy," "Tips for Improving Fine Motor Skills."
The Extremity Constraint-Induced Therapy Evaluation Study: "Stroke Savvy."
National Stroke Association: "Treating Post Stroke Mobility Problems," "Muscle Weakness After Stroke: Hemiparesis."
National Institute of Neurological Disorders and Stroke: "Stroke Rehabilitation Information," "Post Stroke Rehabilitation," "Stroke: Challenges, Progress, and Promise."
Duncan, P. "Management of Adult Stroke Rehabilitation Care: A Clinical Practice Guideline." Stroke, 2005; vol 36: pp e100-e143.
Randie M. Black-Schaffer, M.D., M.A., Medical Director, Stroke Program, Spaulding Rehabilitation Hospital, Boston, MA.
The Ohio State University Medical Center, Department of Rehabilitation Services: "Assisted Arm Range of Motion," "Self-Range of Motion Exercises for Shoulders, Arms, Wrists, and Fingers," "Arm Strengthening Program," "Electrical Stimulation," "Activities to Improve Fine Motor Coordination in Hands."
Harris, J. "Strength Training Improves Upper-Limb Function in Individuals With Stroke." Stroke, 2010; vol 41: pp 136-140.
International Functional Electric Stimulation Society: "ES in Stroke and Brain Injury."
Shaw, S. Botulinum Toxin Type A for Upper Limb Spasticity After Stroke. Expert Review of Neurotherapeutics, 2009; vol 9 no 12: pp 1713-25.
Saulino, M. "The Pharmacological Management of Spasticity." The Journal of Neuroscience Nursing, 2006; vol 38, no 6: pp456-459.
WebMD Medical Reference from Medicinenet.com: "Definition of Neuroplasticity."