Diverticulitis Slideshow: Causes, Symptoms, and Treatments

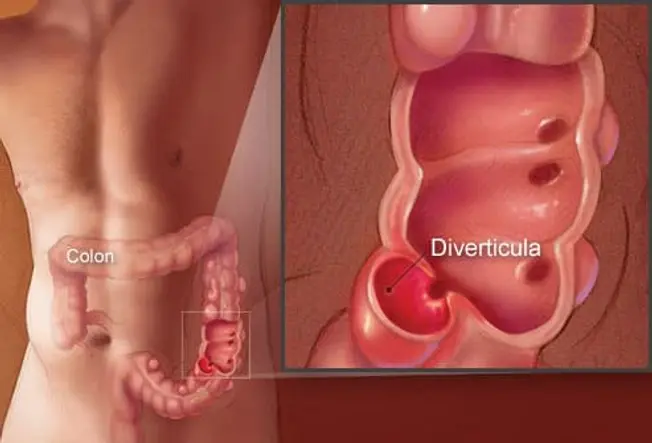
What Is Diverticulitis?
Sometimes tiny, bulging pouches (called diverticula) form in the colon. This condition is called diverticulosis. If the pouches become inflamed or infected, this is diverticulitis.
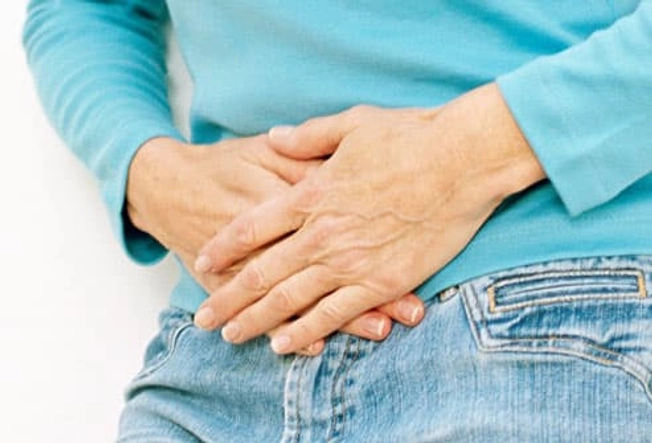
Symptoms of Diverticulosis and Diverticulitis
People with diverticulosis usually don't have outward symptoms. Symptoms of diverticulitis are more noticeable. There may be abdominal bloating, pain, and tenderness, typically in the left lower abdomen, plus diarrhea, chills, and a low-grade fever.

What Causes Diverticula to Form?
The reason diverticula form in the colon is not completely understood. Doctors think diverticula form when high-pressure areas inside the colon push against weak spots in the colon wall. These diverticula are most common in the lower part of the large intestine (called the sigmoid colon).
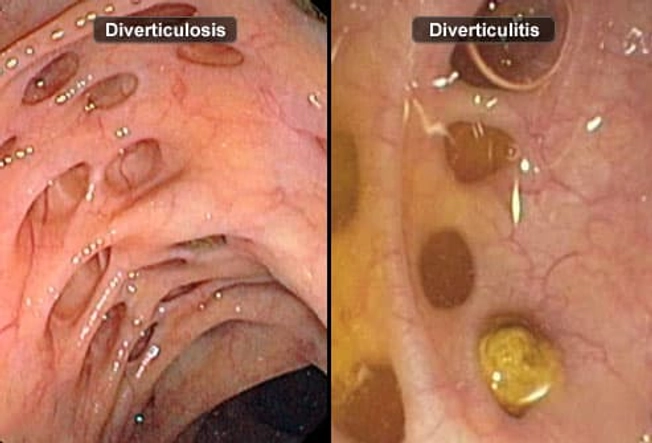
Diverticulosis vs. Diverticulitis
Having diverticulosis is very common and most people never know they have it. Half of all people older than 60 have it. But only 10%-25% of people go on to develop diverticulitis. Diverticulitis typically develops when the pouches that are blocked with waste become inflamed, leading to tears in the bowel wall and infection.
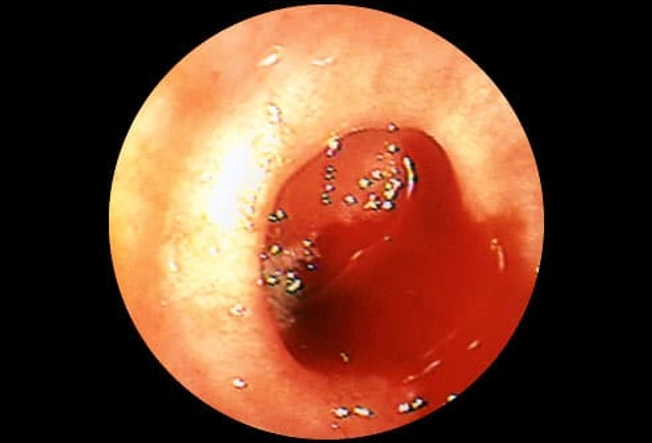
Diverticular Bleeding
When a hole develops between a pouch and a blood vessel, bleeding can happen. This can cause a large amount of blood to suddenly appear in your stool. This condition is usually painless and the bleeding usually stops on its own. But in rare cases, bleeding can be severe enough to require a transfusion or surgery. If you have bleeding, contact your doctor right away.

What's Fiber Got to Do With It?
A diet low in fiber is linked to diverticulosis. Researchers aren't sure why. Adding more fiber to the diet can help prevent constipation and may decrease the risk for painful diverticula in the colon.

Your High-Fiber Choices
Luckily, you don't have to look hard to find an abundance of high-fiber foods. Fiber is found in fruits, vegetables, whole grains, and legumes (dried beans, peas, and lentils). Make smart food choices, including brown rice and whole wheat pasta in place of the regular version. And add extra veggies to your favorite dishes -- pizza, stews, and spaghetti sauce. The American Dietetic Association recommends that women get about 25 grams of fiber and men about 38 grams each day.
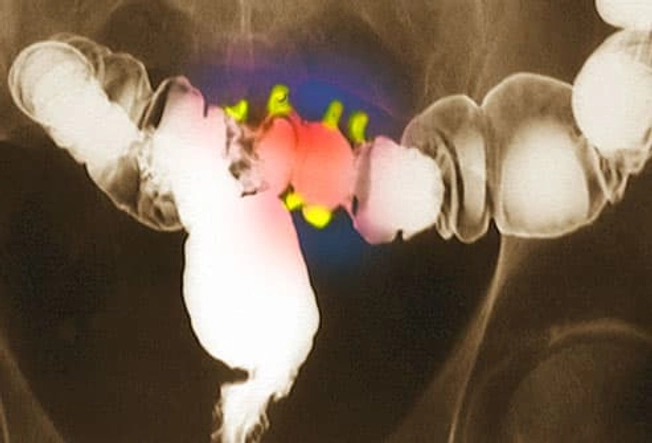
Diagnosing Diverticular Disease
Since diverticulosis doesn't usually cause symptoms, it is often only diagnosed when the patient is being seen for another reason. The diverticula (pictured here in yellow) can be seen via X-ray or a colonoscopy. When diverticulitis leads to a painful abscess, an ultrasound and CT scan of the abdomen and pelvis can show collections of pus.

Treatment for Diverticulosis
Most patients with diverticulosis have minimal or no symptoms and do not require specific treatment. A high-fiber diet and fiber supplements are recommended to prevent constipation and the formation of more diverticula.

Treating Diverticulitis
When diverticulitis symptoms -- abdominal pain, cramps, and fever -- are mild, antibiotics taken by mouth are usually enough. When pain is worse, a clear liquid diet to allow the colon and bowel to recover may also be prescribed. When pain is increasingly severe, or when there is high fever or the inability to drink liquids, a hospital stay may be necessary, along with intravenous antibiotics and not eating or drinking for a few days.

Complications of Diverticulitis
When inflammation of the diverticula leads to a tear in the intestinal wall, as pictured here, pus can leak into the abdominal area, causing peritonitis (a painful infection of the abdominal cavity), abscesses, intestinal obstruction, and an opening (called a fistula) between the bowel and the urinary tract or other organ in the abdomen or pelvis.

When Surgery Is Necessary
Diverticulitis that does not respond to medical treatment requires surgery. Surgery usually involves draining pus and removing the segment of the colon containing the diverticula. Removal of bleeding diverticula is necessary for patients with persistent bleeding. Surgery may also be necessary for any diverticula that erode into the bladder, causing severe, recurrent urine infections and passage of gas during urination, and to treat intestinal obstruction.

Preventing Diverticulitis?
Once formed, diverticula are permanent. And no treatment has been found to prevent complications of diverticular disease. But diets high in fiber increase stool bulk and prevent constipation, which may help symptoms. What about seeds and nuts? There's no evidence these foods cause diverticulitis flares. But if you feel they trigger your symptoms, eat other high-fiber foods instead. Drinking plenty of water and getting regular exercise may also help.