- Age-Related Macular Degeneration (AMD)
- Wet Age-Related Macular Degeneration
- Geographic Atrophy
- Appointment Prep
- View Full Guide
Macular Degeneration

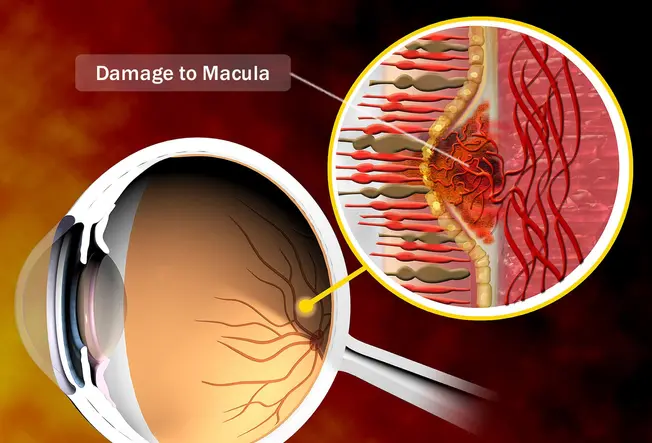
Your Macula
Macular degeneration is the leading cause of vision loss. It’s also called age-related macular degeneration. Your macula is part of your retina -- the area in the back of your eye that turns images into signals that go to your brain. It lets you see small details clearly. When the macula starts to break down, you have trouble seeing those kinds of things. For example, you might be able to see a clock's outline, but not make out its hands.

Symptoms
Early signs include blurred vision and trouble seeing color and fine details. As the disease gets worse, you lose your center vision. You may have trouble reading, driving, and making out people’s faces. You will need brighter light to do daily tasks and will find it harder to judge distances or go up and down steps. Visual hallucinations -- seeing things that aren’t really there -- are also a sign.

Who Gets It?
Macular degeneration affects more than 10 million Americans -- more people have it than cataracts and glaucoma combined. This is not true in other parts of the world. People over 60 are diagnosed with macular degeneration the most. White people are more likely to get it than people of other races, and women more than men.

Causes
Doctors don’t know exactly why macular degeneration happens, but your family history plays a part. Your chances of having it go up if you have a parent, sibling, or child with the disease. But your lifestyle matters, too. For example, smokers are twice as likely to have it as people who don’t light up. Other things that make it more likely include being female, being exposed to ultraviolet light, and getting older.
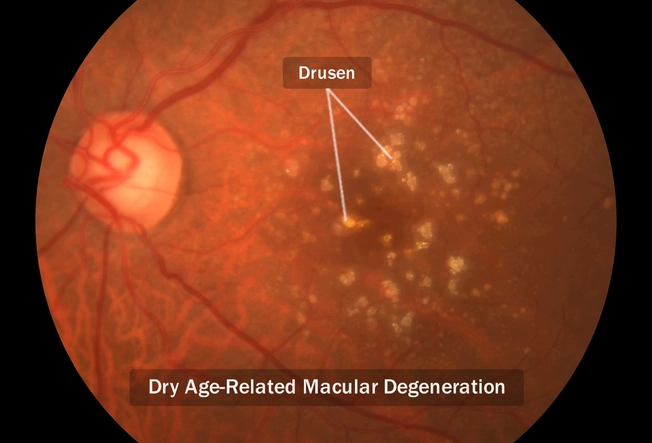
Different Types
Most people have a “dry” type of macular degeneration. That means small white or yellow fatty deposits, called drusen, have formed in your retina and are causing it to break down. The dry kind tends to get worse very slowly. With the “wet” version, abnormal blood vessels damage your macula and change the shape of your retina. While it’s less common, the wet type is the cause of 90% of legal blindness from macular degeneration.
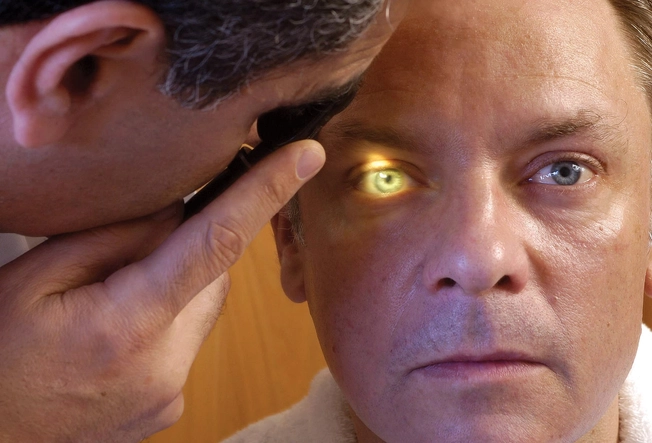
Diagnosis
Your eye doctor may put drops in your eyes to dilate (widen) your pupils. This lets them use a special device called an ophthalmoscope to look for fatty deposits and other signs of trouble in the back of your retina. If your doctor thinks you have the wet type, they'll take a special scan of your eye that can show any problem blood vessels. Yearly eye exams can help your doctor spot early signs before you have any symptoms.

Treatment for the Dry Type
There’s no treatment or cure for dry macular degeneration. But you may be able to slow it down with AREDS or AREDS2 supplements, which contain a particular combination of vitamins and minerals. Research shows these high-dose supplements could reduce the risk that intermediate dry macular degeneration will progress to the advanced stage by 25%. Your eye doctor can tell you if they might be right for you.
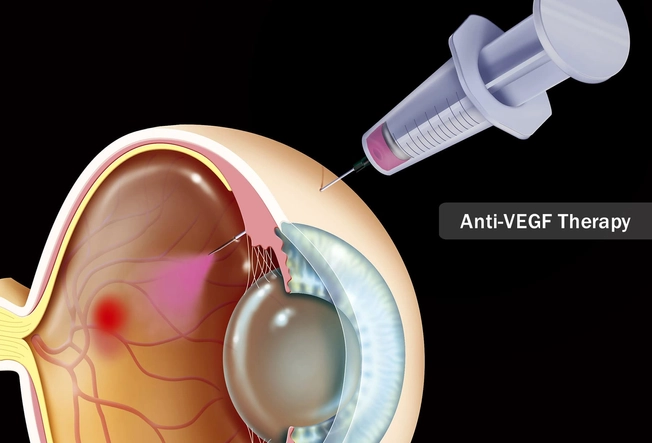
Treatment for the Wet Type
For this kind, your doctor may recommend a drug that blocks proteins in your body that make problem blood vessels in your retina bigger. Vascular endothelial growth factor (VEGF) is the main protein that causes new blood vessels to form in the macula in wet AMD. Delivered by injection, VEGF inhibitors reduce leakage from blood vessels, prevent their growth, decrease swelling of the retina, reduce vision loss, and improve vision in wet AMD.
Angiopoietin-2 is another protein involved in blood vessel formation. Ang-2 inhibitors help stabilize these fragile new blood vessels so they don’t leak and help make vessels less sensitive to the effects of VEGF.
How often you have the shots and how long you get them depend on the specific drug and how well it works for you.
Laser Surgery
If you have wet macular degeneration, your doctor may recommend this. They’ll point a laser at the extra blood vessels in your eye to break them up. Photodynamic therapy (PDT) is another option. A special light-sensitive drug is put into your body through a vein in your arm, then triggered with a laser to destroy problem blood vessels.
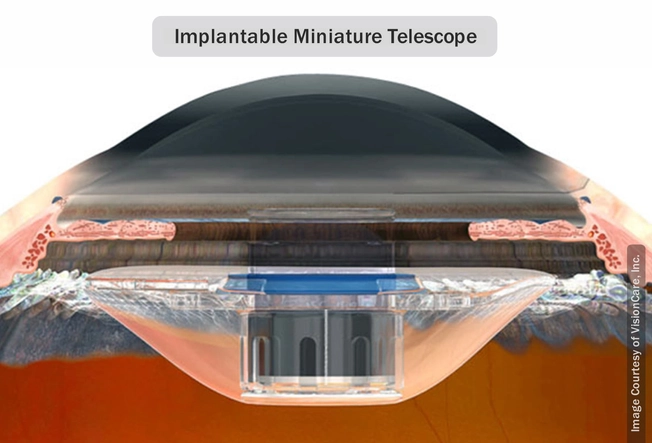
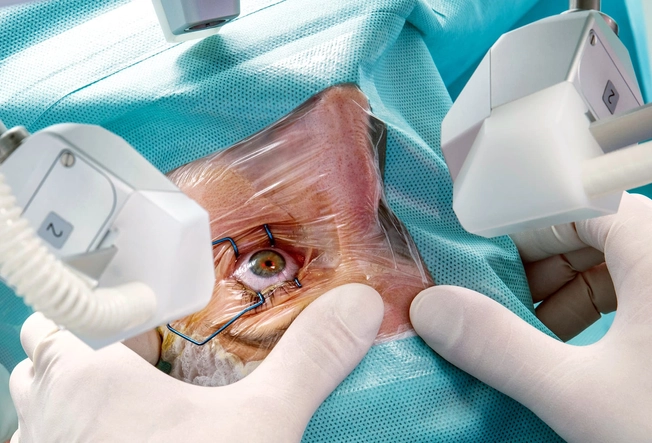
Regain Some Vision
In advanced cases of dry macular degeneration, your doctor may suggest replacing the lens of your eye with a telescope the size of a pea. This makes images larger so the healthy parts of your retina can see them. But it’s not right for everyone, including people who have had cataract surgery.

Technology
Plenty of high-tech devices can help you get through your daily life. You can get a telescope put on your eyeglasses so you can see things far away. Computer software can turn words on a screen into speech you can hear. And a closed-circuit television magnifier lets you see something like a book or needlepoint on a TV screen.

Lifestyle Changes
There’s no cure for macular degeneration, but you can make healthy choices to slow it down and keep your symptoms from getting worse: Get regular exercise, protect your eyes from the sun with sunglasses, and if you smoke, quit. Try to eat a healthy diet rich in leafy green vegetables and fish. Keeping your blood pressure and cholesterol levels in check can help, too.

Emotional Support
Vision loss can have a big effect on your life. You have to change the way you do everyday tasks, such as cooking or reading, and you may rely more on your friends and family than you used to. You may feel depressed. Talking with a counselor or finding a local support group can help you work through these emotions.

Research
Researchers are looking into many new treatments. Drugs that lower cholesterol have shown promise in cutting back on the fatty deposits that cause dry macular degeneration. And low doses of X-ray radiation might help break up problem blood vessels in the wet type. New drugs being tested may also improve your vision with fewer side effects.