A Visual Guide to Understanding Heartburn and GERD


Heartburn Begins With a Bite
Take a bite of warm, gooey pepperoni pizza, and your digestive system kicks in. Acids go to the stomach, ready to break down your meal. In many people, a faulty valve-like structure lets these acids run amok, leaking into your esophagus and triggering a burning feeling in the chest. Heartburn is a very common symptom. More than 60 million Americans have it at least once a month. The following slides show where heartburn starts and how to stop it.
Heartburn: An Inside Look
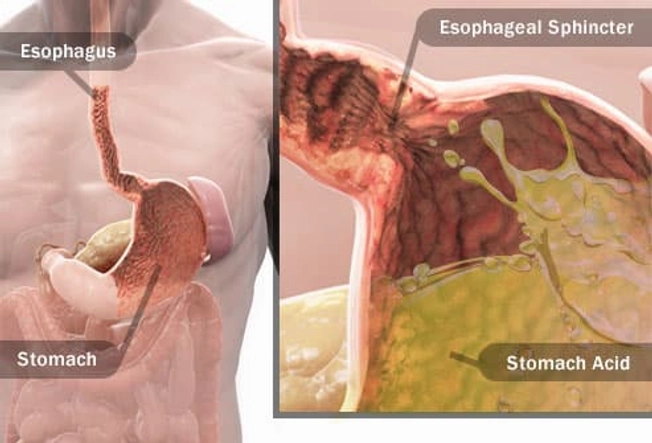
To understand what causes heartburn, let's trace the path of that pepperoni pizza. Once you swallow a bite, it travels through the esophagus to the stomach. A valve-like ring of muscle called the lower esophageal sphincter opens to let the food in. Then it's supposed to close again to prevent stomach acids from sliding up into the esophagus.
Heartburn: Faulty Valve
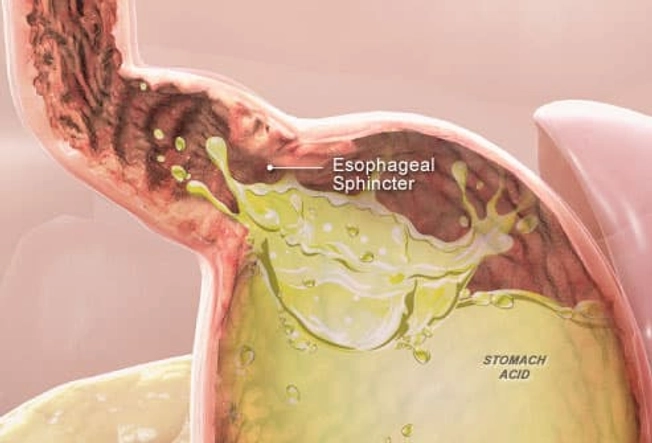
In some people, the sphincter between the stomach and esophagus doesn't work as well as it should. This allows acid to seep into the esophagus (called acid reflux), where it can cause pain and irritation. Not everyone with acid reflux suffers from heartburn, and some people with "heartburn" symptoms don't actually have acid reflux but may have some other condition causing this pain.

GERD (Acid Reflux) Symptoms
The hallmark of acid reflux is heartburn -- a painful burning sensation in the middle of the chest. Heartburn typically strikes after meals and can last several hours. The discomfort may be worse after bending over or lying down. Other symptoms of severe acid reflux include a sour-tasting fluid in the back of the throat, difficulty swallowing, or feeling that food is stuck in the chest or throat. A chronic cough or asthma attacks can also be caused by acid reflux. A description of heartburn symptoms is usually all that’s needed to diagnose acid reflux.

Heartburn: Who’s at Risk?
Anyone can develop heartburn, but certain lifestyle factors affect how well the sphincter works, as well as the amount of acid produced by the stomach. People who are overweight, eat large meals, wear tight-fitting clothes, or smoke tend to be more vulnerable.
Is it GERD?
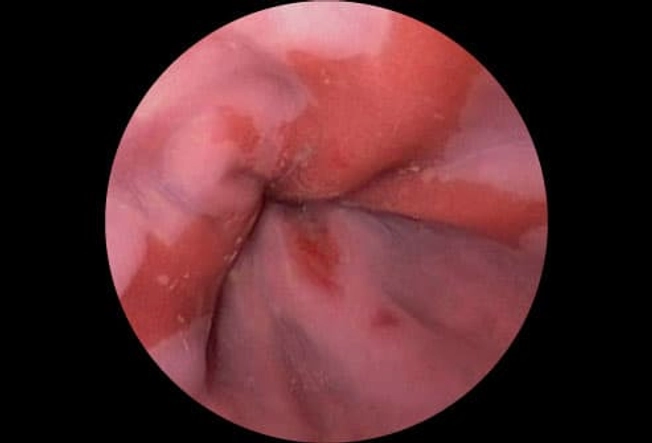
Heartburn usually doesn't pose a serious threat to your health. However, complications can occur with severe, frequent, and persistent acid reflux. If you have severe heartburn or heartburn two or more times a week, you may have a condition called GERD (gastroesophageal reflux disease) and you should see your doctor. Without treatment, chronic GERD can cause inflammation, ulcers, and scarring. GERD can also lead to changes in the cells lining the esophagus. Known as Barrett's esophagus (shown here), these changes raise the risk of esophageal cancer.

Nighttime Heartburn
Waking with a sore throat, cough, or a bitter taste in your mouth? It could be nighttime acid reflux. In addition to disturbing sleep, nighttime reflux may raise the risk of esophageal damage. That's because lying down leaves stomach acid in the esophagus longer. And as we sleep, we swallow less acid-neutralizing saliva than when awake.

Managing Heartburn at Home
You may be able to manage mild heartburn with a few changes to your daily routine. Start by eating smaller meals. Finish dinner at least three to four hours before bedtime and avoid late-night snacks. (Having food in your stomach when you lie down can worsen acid reflux symptoms such as heartburn.)

Watch What You Eat
Some foods are known to contribute to heartburn by bringing additional acid into the stomach or by relaxing the lower esophageal sphincter. Stay away from food that may give you problems. Your symptoms may improve if you avoid tomatoes, onions, garlic, chocolate, peppermint, fatty foods, and citrus fruits, including oranges and grapefruit. If you find spicy foods are a trigger, try milder versions rather than giving up your favorite foods altogether.

Watch What You Drink
Certain beverages can also bring on heartburn. These include coffee, tea, sodas, alcohol, tomato juice, and orange juice. However, unless these are causing you acid reflux symptoms, you don't have to avoid them.

Change Your Exercise Routine
Exercise can increase abdominal pressure, increasing the risk of acid reflux. Some types of exercise increase the risk more than others by reversing the natural flow of digestion. Headstands and inverted yoga poses, such as downward dog, are good examples. Abdominal crunches can be a problem, because the motion may thrust stomach acids into the esophagus.

Raise the Head of Your Bed
If you have nighttime heartburn, try placing blocks under the legs of your bed to raise the head about 6 inches, or sleep with your upper body on a wedge pillow. This strategy uses gravity to keep stomach acids where they belong. (Avoid raising your head with piles of pillows. This bends your body in a way that can aggravate heartburn.) For some, reflux also happens less frequently when lying on your left side rather than your right.

Wear Loose-Fitting Clothes
Another way to ease heartburn is to take pressure off the abdomen. Lose excess weight and wear loose-fitting clothes and belts.

Heartburn During Pregnancy
More than half of all pregnant women report symptoms of severe heartburn, especially during their second and third trimesters. Changing hormone levels and increased abdominal pressures during pregnancy increase the risk of acid reflux and heartburn. Mild symptoms should be treated with lifestyle changes, including eating several small meals a day instead of three large ones, avoiding fried and spicy foods, and not lying down after eating. However, if diet and lifestyle don't alleviate symptoms, pregnant women should consult their doctor before taking any medications.

Heartburn Remedies: Antacids
For occasional heartburn, take something that works immediately, like a liquid antacid. Just like the name suggests, an antacid neutralizes stomach acid. This provides temporary relief from heartburn, and is emptied from the stomach quickly. It's important to follow the directions carefully, because the overuse of antacids can cause serious side effects. And with more prolonged heartburn symptom, antacids may not help.

Heartburn Remedies: H2 Blockers
Also available over-the-counter, H2 blockers work differently than antacids. Rather than zapping acids after they appear, these medications lower the production of stomach acid. This can help prevent heartburn from acid reflux if taken about 30 minutes before meals. More powerful doses are available in prescription form.

Acid Blockers: Proton Pump Inhibitors
Proton pump inhibitors, available over-the-counter and by prescription, are a class of drugs that block the production of stomach acid. They are more effective at decreasing acid production than H2 blockers.

Which Heartburn Medication to Take?
The heartburn treatment that's best for you depends on many things. How often does heartburn happen? How bad is it? Do you want fast relief or prevention? Antacids offer fast relief for mild heartburn. H2 blockers can stop the burn before it starts, but only if you know when to take them, and they may take longer to work. Proton pump inhibitors can tackle really stubborn heartburn. Your doctor can help you pick the treatment that's right for you.
IMAGES PROVIDED BY:
(1) Jack Hollingsworth / Photodisc
(2) Original background image from 3D4Medical.com
(3) Original background image from 3D4Medical.com
(4) Stockbyte
(5) Wade / Digital Vision
(6) © ISM / Phototake -- All rights reserved.
(7) © Roy Morsch / CORBIS
(8) Brayden Knell / WebMD
(9) Richard Nowitz / National Geographic
(10) SambaPhoto / Tony Generico
(11) Image Source
(12) MIXA Co. Ltd.
(13) GSO Images / Photographer’s Choice
(14) Hill Street Studios / Blend Images
(15) fanelie rosier / istockphoto
(16) © Bryan F. Peterson / CORBIS
(17) Jupiter Images Unlimited
(18) Jon Feingrish/Blend Images
REFERENCES:
American Gastroenterological Association.
Cleveland Clinic web site.
Daniel Mausner, MD, section head of gastroenterology, Mercy Medical Center, Rockville Center, N.Y.
Deepa A. Vasudevan, MD, assistant professor of family medicine, University of Texas Medical School, Houston.
International Foundation for Functional Gastrointestinal Disorders.
National Digestive Diseases Information Clearinghouse.
Robynne Chutkan, MD, founder, Digestive Center for Women, Chevy Chase, Md.; gastroenterologist, Georgetown Hospital, Washington, D.C.