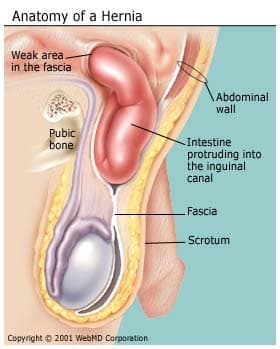
What Is a Hernia?
A hernia happens when an organ or fatty tissue squeezes through a weak spot in a surrounding muscle or connective tissue called fascia. They often happen where the abdominal wall is weaker, such as in the abdomen (belly area) or groin, and can have various causes.
Hernias can be painful. In some cases, they need emergency treatment. Call 911 right away if:
- Your herniais extremely painful, growing quickly, swollen, or red.
- You vomit or feel nauseated.
- You have constipation or bloating.
- You have a fever.
In a reducible hernia, the lump can be pushed back through the abdominal wall. If not, it's an irreducible hernia, which is more likely to have serious complications.
A hernia is an emergency if it is “incarcerated.” In an incarcerated hernia, tissue (such as from the bowel) has slipped through the herniaand gotten stuck there. Stool may not be able to get through normally, which can cause pain, nausea, vomiting, and even tear the bowel wall. If an incarcerated hernia becomes “strangulated,” the bowel tissue has started to die and needs emergency surgery.
Hernia Causes
Ultimately, all hernias are caused by a combination of pressure and an opening or weakness of muscle or fascia. The pressure pushes an organ or tissue through the opening or weak spot. Sometimes the muscle weakness is present at birth. But more often, it happens later in life.
Anything that causes an increase in pressure in the abdomen can cause a hernia, including:
- Lifting heavy objects without stabilizing the abdominal muscles
- Diarrhea or constipation
- Persistent coughing or sneezing
In addition, obesity, poor nutrition, and smoking can weaken muscles and make hernias more likely.
Types of Hernias
The most common types of hernias are inguinal (inner groin), incisional (resulting from a surgical cut, or incision), femoral (outer groin), umbilical (bellybutton), and hiatal (upper stomach).
Groin hernias
About 3 out of every 4 hernias are in the groin. There are two types: inguinal and femoral.
Almost all groin hernias are inguinal. You get them when part of your intestine pushes through a weakness in the lower belly and affects an area of the groin called the inguinal canal.
There are two kinds of this hernia:
- Indirect. The more common type; it enters the inguinal canal.
- Direct. It does not enter the inguinal canal but goes straight through the bowel wall.
They’re much more common in men than women, but they’re not limited to adults.
With an inguinal hernia, you’ll probably see a lump where your thigh and groin come together. It may seem to go away when lying down, but you see it clearly when you cough, stand, or strain.
Generally, these hernias aren’t dangerous. Your doctor may consider watchful waiting, or monitoring the hernia.
Femoral hernias account for only a few out of every 100. They’re more common in older women. They are often mistaken for inguinal hernias.
Femoral hernias bulge into a different area of the groin called the femoral canal. You might see a lump right around the crease of the groin or just into the upper thigh. Your doctor will likely suggest surgery for a femoral hernia instead of watchful waiting, since they are more likely to get stuck without being reducible.
Umbilical hernias
This is the second most common type of hernia. Umbilical hernias happen when fat or part of the intestine pushes through muscle near the bellybutton. They’re more common in newborns, especially in those born earlier than expected and babies under 6 months old. But adults can get them, too.
Women are more likely than men to get an umbilical hernia. Your chances are also higher if you:
- Are overweight
- Have been pregnant more than once
- Have a lot of belly fluid (a condition called ascites)
- Have a long-term cough
- Have trouble peeing because of an enlarged prostate
- Are constipated for long periods of time
- Vomit repeatedly
What all of these risk factors have in common is increased pressure in the abdomen that pushes the hernia out.
Incisional hernias
If you have surgery in which a doctor makes an opening through your belly, you might get an incisional hernia later. Tissue can poke through where the skin has been weakened by a scar left after surgery. Like groin hernias, they can lead to more serious problems if they’re not repaired.
Incisional hernias are common in people who have had an operation, especially emergency surgery. You can be more likely to get one if you do any of these things before your incision heals completely:
- Gain a lot of weight
- Exercise too soon or too heavily
- Get pregnant
Your chances are also higher if the wound gets infected or if you:
- Are a man over 60
- Are obese
- Have long-term lung disease
- Have diabetes or kidney failure
- Smoke
- Take long-term medications like steroids or drugs that affect your immune system
These are a little different from the other types of hernias because of where they happen.
Hiatal hernias involve your diaphragm, the sheet of muscle that separates your chest from your belly. Your esophagus runs from your throat to your stomach and passes through an opening in the diaphragm.
With a hiatal hernia, part of the stomach bulges up through this opening and into the chest. You won’t see any lump, but you might get heartburn or chest pain and notice a sour taste in your mouth.
Although they’re the most common hernias seen in pregnant women, this type of hernia is most often found in people over age 50.
Other types of hernias
Less common types of hernias include:
- Epigastric hernia. This is when fat pushes through the belly somewhere between the bellybutton and lower part of the breastbone. These show up in men more often than women.
- Giant abdominal wall hernia. You might get one of these if you have an incisional hernia or some other kind that’s hard to treat and keeps coming back.
- Spigelian hernia. You get this type when fat tissue pushes through muscle below your bellybutton along the bottom edge of where your six-pack might be.
Symptoms of a Hernia
Symptoms depend on the type of hernia. In some cases, you may not have any symptoms.
For inguinal, femoral, umbilical, and incisional hernias, symptoms may include:
- An obvious swelling beneath the skin of the abdomen or the groin. It may be tender, and it may disappear when you lie down.
- A heavy feeling in the abdomen that sometimes comes with constipation or blood in the stool
- Discomfort in the abdomen or groin when lifting or bending over
- A burning or aching sensation at the bulge
- Weakness or pressure in your groin
- Heartburn
- A hard time swallowing
- Shooting pain
- Vomiting
- Constipation
- Pain and swelling around the testicles
Symptoms of a hiatal hernia may include heartburn and upper abdominal pain.
Strangulated hernia symptoms
Usually, you can push a hernia in. But sometimes, you can’t. It can get stuck in your abdomen. If the trapped part gets cut off, or strangulated, from blood flow, it’s a serious situation and can be life-threatening.
Call your doctor right away if you have any of the symptoms of a strangulated hernia, including:
- Nausea, vomiting, or both
- Fever
- Sudden pain that gets worse quickly
- A hernia bulge that turns red, purple, or dark
- Not being able to poop or pass gas
Hernia signs and symptoms in children
Hernias are common in kids, especially babies. They can happen when part of their abdominal wall is weak at birth. If your child has one, you’ll usually notice a bulge in their groin area or around their bellybutton. Your baby may also cry a lot and refuse to eat. Hernias often bulge when your child cries, coughs, or strains to poop. You may also notice that their belly is tender to the touch.
When to See a Doctor
You should see a doctor if you:
- Suspect that you have a hernia
- Can't get a hernia to go back in or it goes soft; seek medical care right away, as this is an incarcerated hernia and can lead to organ strangulation.
- Have a painful or noticeable bulge in your groin on either side of your pubic bone
- Know you have a hernia, and have symptoms of a strangulated hernia. Seek medical care right away.
Hernia Treatment
Hernias usually don’t get better on their own. They tend to get bigger. In rare cases, they can lead to life-threatening complications. That’s why doctors often suggest surgery. But not every hernia needs treatment right away. It depends on the size and symptoms. If it doesn't have symptoms, it may not need treatment at all.
A surgical hernia repair involves pushing the bulge back inside the body part that should contain it using mesh, and keeping it there.
Hernia Surgery
Your doctor will likely suggest it if any of these things happen:
- Tissue (such as the intestine) becomes trapped in the abdominal wall. This is called incarceration. If left untreated, it may lead to strangulation. That’s when the blood supply to the tissue gets cut off.
- The hernia becomes strangulated. This can cause permanent damage and is a surgical emergency. Strangulated organs, usually your intestines, will die, and if not removed quickly, you can become seriously ill. Call your doctor right away if you have a fever or nausea, sudden pain that gets worse, or a hernia that turns red, purple, or dark.
- The hernia causes pain or discomfort, or it’s growing larger.
You may be able to wait to have surgery if:
- Your hernia goes away when you lie down, or you can push it back into your belly. This is called a reducible hernia.
- It’s small and causes few – or no – symptoms (These may never need surgery.)
Talk to your doctor. They’ll watch for changes to your hernia during your yearly physical.
Nearly all children and adults can have hernia surgery. If you’re seriously ill or very frail, you may choose not to have an operation. Your doctor can help you weigh the benefits of the procedure against your ability to recover.
Types of Hernia Surgery
Your doctor can remove your hernia in one of two ways. Both are done at a hospital or surgery center. You’ll usually go home within a few days. In many cases, you’ll be able to go home the same day as your procedure.
Open surgery: You'll get general anesthesia before having open surgery. The surgeon makes a cut (incision) to open your skin. They’ll gently push the hernia back into place, tie it off, or remove it. Then they’ll close the weak area of the muscle – where the hernia pushed through – with stitches. For larger hernias, your surgeon may add a piece of flexible mesh for extra support. It’ll help keep the hernia from coming back.
Laparoscopic surgery: In this surgery, your abdomen is inflated with a harmless gas. This gives the surgeon a better look at your organs. They’ll make a few small incisions (cuts) near the hernia. They’ll insert a thin tube with a tiny camera on the end (laparoscope). The surgeon uses images from the laparoscope as a guide to repair the hernia with mesh. For laparoscopic surgery, you’ll receive general anesthesia.
You'll usually get better faster with laparoscopic surgery: On average, you're back to your normal routine a week sooner than with open surgery.
What kind of surgery you’ll need often depends on the size, type, and location of your hernia. Your doctor will also consider your lifestyle, health, and age.
Hernia Surgery Risks
This type of operation is normally very safe. But like all surgeries, having your hernia removed comes with a number of possible problems. They include:
- Infection of the wound
- Blood clots: These can develop because you’re under anesthesia and don’t move for a long period of time.
- Pain: In most cases, the area will be sore as you heal. But some people develop chronic, long-lasting pain after surgery for a groin hernia, for example. Experts think the procedure may damage certain nerves. Laparoscopic surgery may cause less pain than an open procedure.
- The hernia could come back after the surgery: Research shows that using mesh can cut your risk of this happening by half.
Nonsurgical Hernia Treatments
Your doctor may suggest that you wear a corset, binder, or truss. These supportive undergarments apply gentle pressure on the hernia and keep it in place. They may ease discomfort or pain. You use them if you can't have surgery or for temporary relief before your procedure. Only use these garments under your doctor’s care.
