Cluster headaches are a series of relatively short but very painful headaches every day for weeks or months at a time. You tend to get them at the same time each year, such as in the spring or fall. Because of this, people often mistake cluster headaches for symptoms of allergies or work stress.
Experts don't know what causes them, but a nerve in your face is involved, creating intense pain around one of your eyes. It's so bad that most people can't sit still and will often pace during an attack. Cluster headaches can be more severe than a migraine, but they usually don't last as long.
These are the least common type of headaches, affecting fewer than one in 1,000 people. Men get them more than women do. You usually start getting them before age 30. Cluster headaches may go away completely (this is called going into remission) for months or years, but they can come back without any warning.
What Happens
You get a cluster headache when a nerve pathway in the base of your brain is triggered. That signal seems to come from a deeper part of the brain called the hypothalamus, home of the "internal biological clock" that controls your sleep and wake cycles.
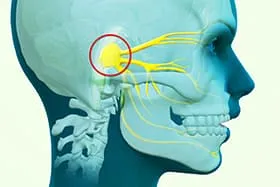
The nerve that's affected, the trigeminal nerve, is responsible for sensations such as heat or pain in your face. It's near your eye, and it branches up to your forehead, across your cheek, down your jaw, and above your ear on the same side.
A brain condition, such as a tumor or aneurysm, won't cause these headaches.
Characteristics of Cluster Headaches
There are a few things that set this type of headache apart. They include:
- Speed. Cluster headaches generally reach their full force quickly, within 5 or 10 minutes.
- Pain. It’s almost always on one side of your head, and it stays on the same side during a period, the time when you're getting daily attacks. (When a new headache period starts, it might switch to the opposite side, but that's rare.) It's often described as a burning or piercing. It may be throbbing or constant. You'll feel it behind or around one eye. It may spread to your forehead, temple, nose, cheek, or upper gum on that side. Your scalp may be tender. You can often feel your blood pulsing.
- Short duration. Cluster headaches usually last only 30 to 90 minutes. They can be as short as 15 minutes or as long as 3 hours, but then they disappear. You'll probably get one to three of these headaches a day. Some people have as few as one every other day, while others get them up to eight times a day.
- Predictable. Attacks seem to be linked to the circadian rhythm, your body's 24-hour clock. They happen so regularly, generally at the same time each day, that they've been called "alarm clock headaches." They might even wake you up an hour or two after you go to bed. Nighttime attacks can be more severe than daytime ones.
- Frequent. Most people will get daily headaches for 2 weeks to 3 months; in between these periods, they'll be pain-free for at least 2 weeks.
Symptoms
The pain usually starts suddenly, often around or behind the eye. You may notice:
- Discomfort or a mild burning feeling
- A swollen or drooping eye
- A smaller pupil in the eye
- Eye redness or watering
- Runny or congested nose
- Red, warm face
- Sweating
- Sensitivity to light
- Restlessness or agitation, pacing
Cluster headaches are more common in people who smoke or who are heavy drinkers. During a cluster period, you'll be more sensitive to alcohol and nicotine. Just a bit of alcohol can trigger a headache. But drinking won't trigger one during headache-free periods.
Triggers
When you’re in a cluster period, any of these can bring on a headache:
- Cigarette smoke
- Alcohol
- Strong smells
- Change to a high altitude
- Bright light
- Exercise or exertion
- Heat
- Foods that contain nitrates, such as bacon or lunch meat
- Cocaine
Migraine vs. Cluster Headache
Both types of headaches cause intense pain. But the way they hurt and where you feel them are different.
Migraine headaches begin slowly and can last a few hours to a few days. You might get some warning signs up to a day before the pain starts, like cravings for certain foods or changes in your mood. You might also see auras just before the migraine hits.
Migraine gives you a throbbing pain. A cluster headache usually hurts on just one side of your head, but you might feel a migraine on both sides, on one side only, or along your forehead. It will probably get worse when you move your head. You may also have:
- Nausea and vomiting
- Sensitivity to light, sound, and smells
- Colored spots, lines, flashing lights, or sparkles in your vision, called auras
- Numbness or tingling
- Weakness
- Trouble speaking or hearing
After a migraine ends, you can have a sort of "hangover," where you feel tired or confused. You may hear your doctor call this a postdrome period.
Many things can trigger a migraine, such as:
- Changes in the weather
- Too much or too little sleep
- Strong smells
- Stress
- Loud noises
- Too little food
- Anxiety or depression
- Certain medicines
- Hormone changes
- Caffeine, certain foods, and food additives
Treatment
You have several options when it comes to treating cluster headaches:
Acute attack treatments help when the headache hits:
- Triptans. These drugs are among the best ways to treat the pain. You might get:
- Sumatriptan (Imitrex, Onzetra Xsail, Sumavel, Zecuity, Zembrace SymTouch), which works both as a shot or inhaled
- Zolmitriptan (Zomig)
- Dihydroergotamine (DHE 45). This prescription medicine is based on the ergot fungus.
- Octreotide. This is a lab-made form of somatostatin, a growth hormone. You take it through an IV in your vein.
- Lidocaine. This is a pain reliever, in the form of a nasal spray.
- Oxygen. Your doctor might call it inhaled oxygen. You’ll breathe it in through a face mask for 15 minutes.
Preventive medicine can often stop a headache before it starts. Your doctor can prescribe medication to make a cluster shorter and make attacks less severe, including:
- Corticosteroids like prednisone
- Divalproex sodium (Depakote)
- Galcanezumab (Emgality)
- Ergotamine tartrate (Cafergot, Ergomar)
- Gabapentin (Gralise, Neurontin)
- Lithium carbonate
- Topiramate (Qudexy XR, Topamax, Trokendi XR)
- Verapamil (Calan, Verelan)
Occipital nerve block (your doctor may also call it occipital nerve injection). The doctor will inject a mix of anesthetic and steroid into these nerves. They’re at the base of your skull, and they’re often the starting point for headaches. This is a temporary treatment until a preventive can start to work.
Nerve stimulation. If medication doesn’t work, some people have success with:
- Occipital nerve stimulation. Your doctor surgically implants a device that sends electrical impulses to this group of nerves at the base of your skull.
- Neuromodulation. These FDA-approved noninvasive devices include:
- Cefaly. You put electrodes on your forehead and connect them to a headband-like controller that sends signals to your supraorbital nerve.
- GammaCore. This gadget, also known as a noninvasive vagus nerve stimulator (nVNS), uses electrodes to send signals to this nerve.
Surgery
If nothing else works, surgery may be an option for people who don't get a break from cluster headaches.
Deep brain stimulation, which involves placing an electrode deep into the brain, is losing favor to less invasive options.
Most procedures involve blocking the trigeminal nerve, a main pathway for pain. It controls the area around your eye, but a misstep can lead to weakness in your jaw and loss of sensation in your face and head.
Lifestyle changes
These moves can help you avoid cluster headaches:
- Keep a regular sleep schedule. A change to your routine can kick off a headache.
- Skip alcohol. Any type, even beer and wine, can trigger a bout of headaches when you’re in a cluster series.
Alternative treatments
Talk to your doctor about:
- Capsaicin. A nasal spray of this pain reliever might help.
- Melatonin. This medication, known for easing sleep problems like jet lag, might lower the number of headaches.
Breathing exercises
Breathing exercises have real effects on your body that help keep you calm and control your stress. And for people who get tension headaches or migraine, they can be a key part of treatment.
But are they any match for the intense pain of a cluster headache? While there haven't been studies to show it, some doctors think they're worth trying. After all, there's no harm, and it won't cost you anything.
Breathing exercises can lower anxiety. So if you worry about your next attack, they're a good tool to help you stay even and relaxed.
You can try different types of breathing. No matter which one you use, it helps to:
- Find a quiet space where you won't be bothered.
- Sit down and get comfy.
- Let go of your worries for a few minutes.
It's also best to set aside time for it each day. This regular practice will train your body to fall into the breathing more easily when you need it. If you do it only when you're in pain, it'll be much harder to really sink into it.
And keep in mind that these exercises can’t replace medicine. They're something to use along with your normal treatment.
Deep breathing. When you're stressed and anxious, you tend to take shorter breaths than usual. This exercise helps you reset. The aim is slow, deep, and steady breaths:
- Put your focus on your bellybutton. You might want to put a hand there to help.
- As you breathe in through your nose, pull the air into your belly. Feel it expand as you fill up your lungs.
- Breathe out through your nose with a long, slow breath. Pull your belly in as you empty out your lungs. You can even think to yourself, "Relax."
With each full, deep breath, your nervous system takes it down a notch.
Rhythmic breathing. If your breathing style is usually short and fast, this exercise will help you slow it down a bit:
- Breathe in slowly through your nose as you count to five.
- Breathe out slowly through your nose as you count to five.
- Repeat and see if you can feel yourself relax with each breath.
As you notice yourself getting calmer, you give your body feedback that helps you relax even further.
Visualized breathing. For this one, you combine breathing with pictures in your mind:
- Get comfortable, close your eyes, and breathe normally.
- As you breathe in through your nose, picture calming air that fills up your lungs and expands your chest and belly. Imagine you're breathing in more and more relaxation.
- As you breathe out, picture pushing the tension out right along with your breath.
- Repeat, breathing in calm and out tension.
