Angular cheilitis is a condition that causes red, swollen patches in the corners of your mouth where your lips meet and make an angle. Other names for it are perleche and angular stomatitis. You can get it on one side of your mouth or on both sides at the same time.
Symptoms
The main things you’ll notice are irritation and soreness in the corner(s) of your mouth. One or both corners may be:
- Bleeding
- Blistered
- Cracked
- Crusty
- Itchy
- Painful
- Red
- Scaly
- Swollen
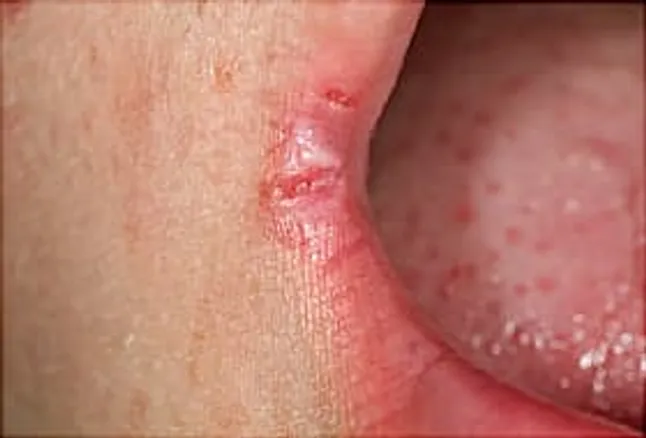
If the irritation is strong, it can make it hard for you to eat. You may not get enough nutrients or you may lose weight.
Causes
Saliva gets trapped and builds up in the corners of your mouth. When it dries, the skin in the area can crack. You may lick your lips often to soothe your cracked skin. The warmth and moisture in the corners of your mouth create the perfect conditions for fungus to grow and multiply -- and cause infection.
Fungal infection is the most common cause of angular cheilitis. It’s usually caused by a type of yeast called Candida-- the same fungus that causes diaper rash in babies. Certain bacteria strains also can cause it.
A deficiency in riboflavin (vitamin B2) may also lead to angular cheilitis.
If your doctor can’t find the cause, it’s called idiopathic angular cheilitis.
Who’s at Risk?
You’re more likely to get angular cheilitis if the corners of your mouth are moist a lot of the time. This might happen for many reasons, such as:
- You have braces.
- You wear dentures that don’t fit well.
- You lick your lips a lot.
- You have a lot of saliva.
- Your teeth are crooked, or your bite isn’t lined up correctly.
- You have sagging skin around your mouth from weight loss or age.
- You suck your thumb.
- You smoke.
- You don’t get enough nutrients, like vitamin B or iron.
Certain medical conditions can put you at a higher risk, such as:
- Anemia
- Cancers of the blood
- Diabetes
- Down syndrome
- Immune disorders, like HIV
- Kidney, liver, lung, or pancreatic cancer
Angular Cheilitis and Diabetes
It’s common for people with diabetes to get fungal infections like angular cheilitis. This is because fungi like Candida feed off glucose -- the blood sugar your body uses as a source of energy. If you have diabetes, you have too much glucose in your blood.
Extra glucose can create a breeding ground for fungus. Diabetes also weakens your immune system, which makes it harder for you to fight off infection.
You can help prevent conditions like angular cheilitis by keeping your blood glucose levels in check. Eat well, exercise, and take your insulin correctly. It’s also important not to smoke.
Diagnosis
To find out if you have angular cheilitis, your doctor will examine your mouth closely to look at any cracks, redness, swelling, or blisters. They’ll also ask you about habits you might have that could affect your lips.
Other conditions (such as herpes labialis and erosive lichen planus) can cause symptoms similar to angular cheilitis. To be sure of the cause, your doctor might swab the corners of your mouth and your nose and send it to a lab to see what kinds of bacteria or fungi might be there.
Treatment
The goal is to clear out the infection and keep the area dry so your skin isn't infected again. Your doctor will recommend an antifungal cream to treat fungal infections. Some are:
- nystatin (Mycostatin)
- ketoconazole (Extina)
- clotrimazole (Lotrimin)
- miconazole (Lotrimin AF, Micatin, Monistat Derm)
If your infection is bacterial, your doctor will prescribe an antibacterial medication, such as:
If your angular cheilitis isn’t caused by a fungal or bacterial infection, your doctor may suggest you put petroleum jelly on the inflamed areas. This protects your mouth from moisture so the sores can heal.

