1 of 7 / Types of Pain
View All
Pain Classifications
Even though the experience of pain varies from one person to the next, it is possible to categorize the different types of pain.
Chronic Pain
Learn about how chronic pain occurs and why chronic pain sometimes lingers.
Nerve Pain
Neuropathic pain is often described as a shooting or burning pain. It can go away on its own but is often chronic.
Psychogenic Pain
Depression, anxiety, and other emotional problems can cause pain -- or make existing pain worse.
2 of 7 / Symptoms & Causes
View All
Causes of Chronic Pain
Often conditions that accompany normal aging may affect bones and joints in ways that cause chronic pain.
What's Causing Your Chest Pain?
Certainly chest pain is not something to ignore. But you should know that it has many possible causes.
Burns and Pain
Burns differ in type and severity, as does the pain. Click here for more about the symptoms and treatments of burn-related pain.
Compressed Nerve (Pinched Nerve)
Pinched nerves can sometimes lead to other conditions such as peripheral neuropathy, carpal tunnel syndrome, and tennis elbow.
3 of 7 / Tests & Diagnosis
View All
4 of 7 / Treatment
View All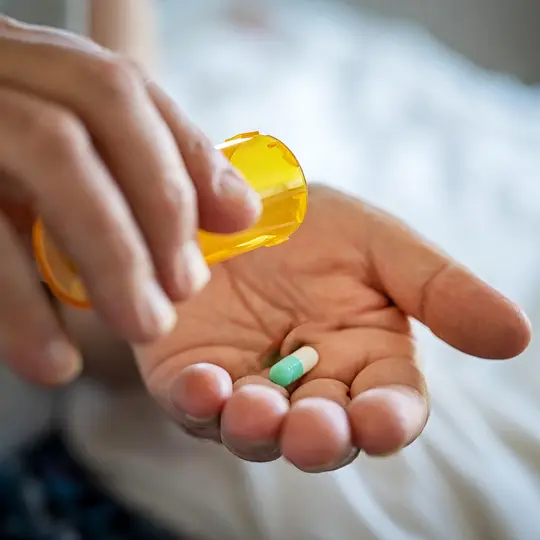
Treating Chronic Pain
Medications, mind-body techniques, and acupuncture can help relieve chronic pain. Learn about your options.
Spine Pain and Treatments
If you have painful compression fractures in the spine, both surgical and nonsurgical treatments may be explored.
Treating Foot Pain
To get the right treatment for foot pain, first you need to know the problem.
Treating Lower Leg Pain
If you're suffering from lower leg pain, you may wonder if it's serious or something you can treat at home.
5 of 7 / Living With
View All
6 of 7 / Support & Resources
View AllFind a Doctor
Use this directory to find detailed listings of doctors in your area.
Related Website: The Arthritis Foundation
For people who suffer from any form of arthritis, this website is a great resource.
Related Website: National Headache Foundation
Headache sufferers and headache doctors use this as foundation’s website as a resource.
7 of 7 / En Español
View All¿Tengo dolor crónico?
Los médicos suelen definir el dolor crónico como cualquier dolor que dura de 3 a 6 meses o más.
Preguntas frecuentes sobre el manejo del dolor
Ocho preguntas sobre el dolor crónico, respondidas.
¿Cómo encuentran los médicos la causa del dolor?
Si tienes dolor, tu médico tiene muchas formas de descubrir qué lo está causando. Te preguntarán sobre tus síntomas y tu historial médico, incluyendo cualquier enfermedad, lesión o cirugía que hayas tenido.
Las clasificaciones y causas del dolor: dolor neural, dolor muscular y más
A continuación, se ofrece una descripción general de los tipos de dolor y lo que los diferencia entre sí.
Suggested Reads about Pain Management
Which NSAID Is Right for You? Here's What to Know
Popular over-the-counter pain and inflammation drugs have been a revelation for people with pain, swelling, or even just run-of-the mill headaches. But these drugs, known as NSAIDs, which include Advil, Motrin, and others, are not all the same and come with some serious health risks if overused. Here’s how to make heads or tails of these commonly used drugs.
Cannabinoids Are Common: Why So Many Use CBD, Delta-8, Others
Some take them to manage pain, others to help improve their sleep. Known more commonly as CBD, delta-8, CBG and CBN, these products have flooded the marketplace.
Alivio del dolor crónico: nuevos tratamientos
Gracias a los nuevos avances en los medicamentos y la tecnología, hoy día tenemos mejores soluciones para el alivio del dolor crónico.
Researchers Locate Signals in Brain Related to Chronic Pain
Using surgical implants inside the brain, scientists have recorded for the first time electrical patterns that occur when a person is feeling chronic pain, a new study in Nature Neuroscience concludes.
Top Search Terms for Pain Management
8 million+ Physician Ratings & Reviews
Find Doctors and Dentists Near You
You can also search by physician, practice, or hospital name