- Headaches Overview
- Migraine
- Cluster & Tension Headaches
- Other Types of Headaches
- Appointment Prep
- View Full Guide
How Migraine Can Affect Your Health

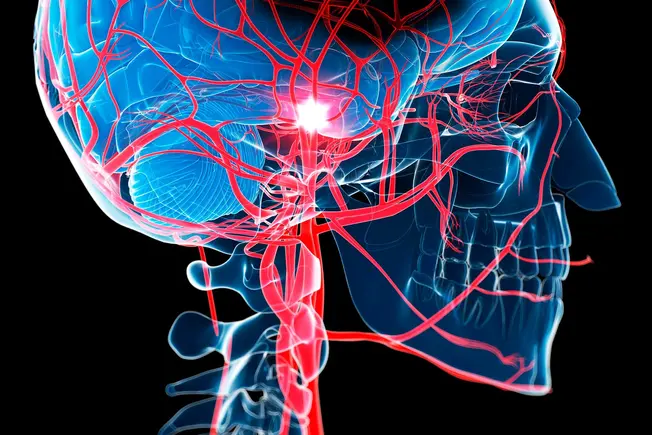
Stroke
Women who get migraines with aura are more likely to have a stroke, which happens when part of your brain suddenly gets cut off from a blood supply. Studies show the chance of having a stroke gets worse if you also smoke, have high blood pressure, or take birth control pills.
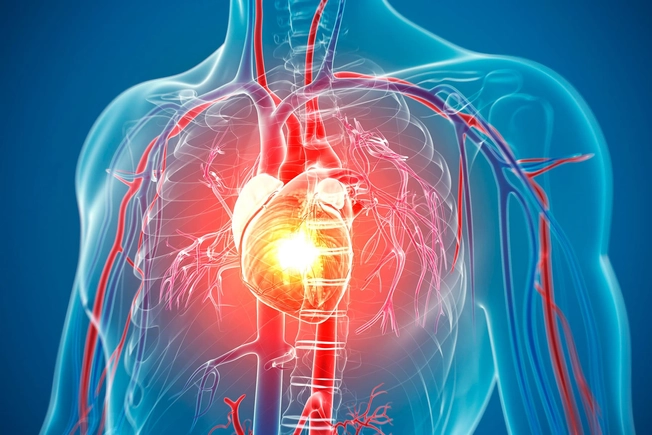
Heart Disease
You're more likely to have heart disease, such as chest pain called angina or a heart attack, if you also have migraines, and vice versa. But there are many things you can do to help lower this risk, including a healthy diet, regular exercise, and a good night's sleep.

High Blood Pressure
Some studies show that people with migraines may be more likely to have high blood pressure. But the research was mostly with white women, so more studies are needed to see if this holds true for others as well.
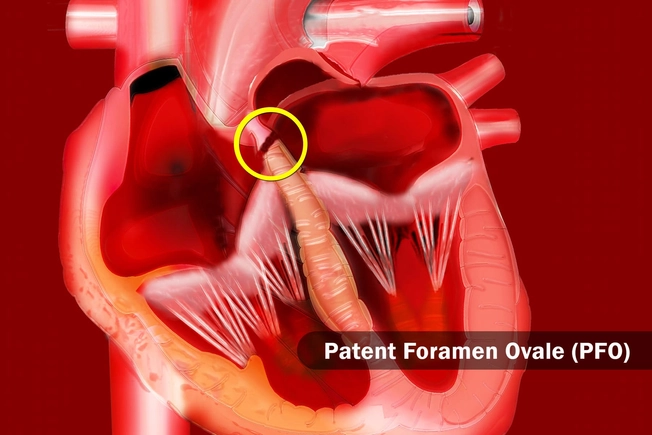
Heart Abnormalities
People who get migraines, especially if they get an aura, are more likely to have problems with the structure of their ticker. One issue in particular is called "patent foramen ovale" (PFO). It's a small hole between the right and left upper chambers of the heart. About a third of people who get migraines have it. That number alsmost doubles though among people who have migraine with aura.
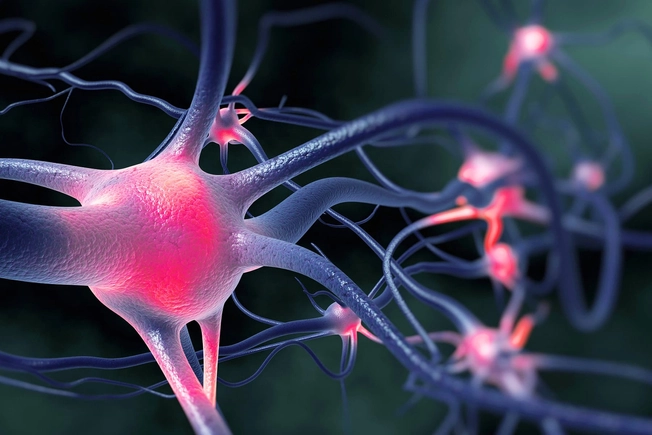
Epilepsy
You're more likely to have this condition, which causes seizures, if you get migraines -- and the other way around, too. Both conditions appear to be caused by a similar problem: cells in the brain called neurons that are unusually sensitive. And both disorders may be due to genes you get from your parents. Doctors use some of the same drugs, like divalproex sodium (Depakote) and topiramate (Topamax), to treat them.

Insomnia
Sleep problems, including insomnia, are common in people who get migraines. They can also lead to anxiety and depression, which are linked to migraine. Irregular sleep habits are also one of the major triggers for migraine headaches. You may sleep better if you wake up every day at the same time and avoid alcohol and caffeine late in the day.

Anxiety and Depression
About 25% of people with migraine have depression, and up to 50% have anxiety. It's more typical if your migraines are frequent -- headaches on 15 days out of the month. The links aren't clear, but it may have something to do with the way your brain sends signals from one neuron to another with a chemical called serotonin.

Childhood Abuse
If you had sexual, physical, or emotional abuse as a child, you may start getting migraines earlier, and they're more likely to turn into a long-term problem. It's not clear why, but doctors know that early stress can change your brain structure, hormones, or nervous system, and even turn on certain genes. Talk to a trusted health care provider about current or past abuse.

Tinnitus
It's a condition that makes it sound as if there's ringing or hissing in your ear. For some people, the problem may only get really bad when they have a migraine. It's not clear why this happens, but it could be that neurons send abnormal signals during an attack.
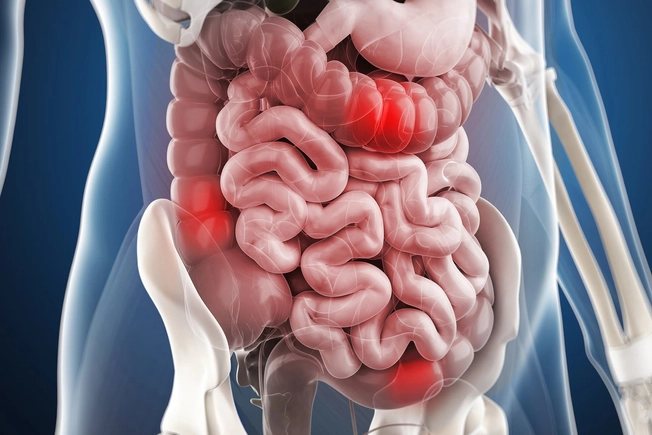
Irritable Bowel Syndrome
People who have symptoms of irritable bowel syndrome, like belly pain, bloating, diarrhea, and constipation, are more likely to get migraines. And new research links them to some of the same genes. More study is needed to figure out what treatments might work together to help these conditions.
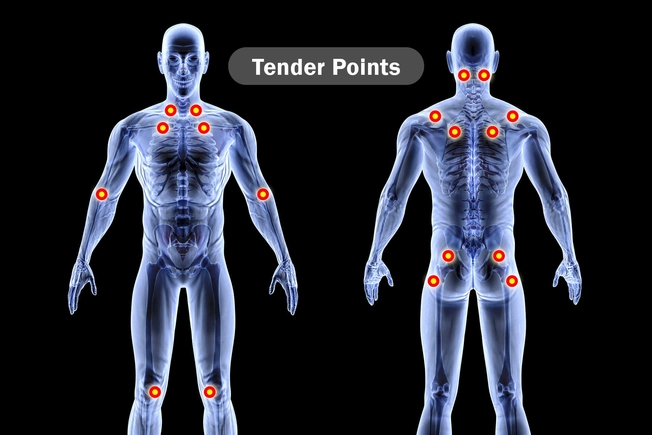
Fibromyalgia
When you have this condition, you could have all-over body pain, anxiety, depression, and be oversensitive to light, sound, and even pressure at specific "tender points." You might also be more likely to get migraines. Preventing migraines with treatment may help keep away fibromyalgia flares, too. Talk to your doctor about the best therapy options for you.

PTSD
It stands for posttraumatic stress disorder. It's a response to a traumatic event like abuse or a bad car accident. When you have PTSD, you "relive" it, including the intense emotions. You're more likely to have migraine if you have this problem. In people with both conditions, almost 70% have PTSD symptoms before they get a headache. Your doctor may be able to help you manage your symptoms with therapy and medication.

Low Blood Sugar
When your blood sugar levels are too low, you have a problem called hypoglycemia. This can trigger a migraine in some people. But a headache caused by fasting is not always due to low blood sugar. It could happen for many reasons, such as you didn't drink enough water, you cut back on your regular amount of caffeine, or your body released stress hormones because you haven't eaten.