Alternative medicine is a term that describes medical treatments that are used instead of traditional (mainstream) therapies. Some people also refer to it as “integrative,” or “complementary” medicine.
More than half of adults in the United States say they use some form of alternative medicine. But exactly what types of therapies are considered alternative? The definition changes as doctors test and move more of them into the mainstream.
This article examines some popular alternative medical treatments and their potential risks and benefits.
Acupuncture
This is a traditional Chinese medicine technique that uses needles to stimulate specific points around the body. The person who performs this therapy (an acupuncturist) sticks thin, sterile needles into your skin. The goal is to help your body’s natural healing process kick in. Studies show that acupuncture can be effective in treating a number of conditions, like neck and back pain, nausea, anxiety, depression, insomnia, infertility, and more.
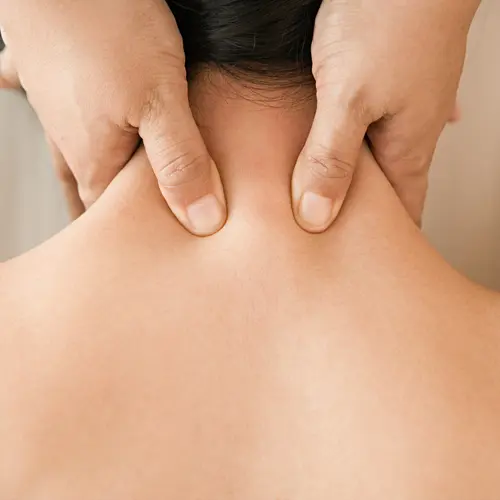
Chiropractic Medicine
This practice focuses on the body’s structure -- mainly the spine --and how it functions. A trained professional called a chiropractor uses different techniques to adjust (“manipulate”) your spine or other parts of your body so that they’re in proper form, or alignment.
The goal of chiropractic medicine is to ease pain, improve body function, and help your body to heal itself naturally.
Much of the research around it has focused on low back pain. But studies show chiropractic can also be helpful for a number of other ailments, like headaches, neck pain, joint problems in your upper and lower body, and disorders caused by whiplash.
Energy Therapies
These focus on the energy fields many people believe exist in and around the body. Included in this category are:
Magnetic Field Therapy. This uses magnetic or electrical fields to treat a number of musculoskeletal problems. Studies show that it may work for osteoarthritis and other pain conditions. Some studies have even shown that it may help fractures heal faster. Magnetic field therapy may not be safe if you’re pregnant, have an implanted cardiac device, use an insulin pump, or take a drug given by patch.
Reiki. Those who practice this alternative treatment believe it taps into the body's natural energy to speed healing. The practitioner hovers their hands over your body or places them lightly on your skin. The goal is to channel energy through their hands to your body to promote healing. There’s very little research to prove it works.
Therapeutic (“Healing”) Touch. Here, a therapist uses their healing energy to identify and repair imbalances in a person’s energy field. Unlike Reiki, the therapist doesn’t touch you. They simply move their hands back and forth over your body. Research shows healing touch can reduce anxiety in people who have cancers. It can also increase their sense of well-being. But it’s unclear if it works for other issues, as well.
Herbal Medicine
This alternative therapy uses parts of a plant -- its roots, leaves, berries, or flowers -- to heal the body.
According to the World Health Organization, an estimated 80% of people around the world use herbal medicine. Studies show certain herbs are effective in treating a number of health issues, like allergies, premenstrual syndrome, chronic fatigue, and more.
Unfortunately, herbal supplements can be sold without being proven to be safe or effective. Talk to your doctor if you’re thinking about using them.
Ayurvedic Medicine
Ayurveda is one of the world’s oldest medical systems. It started in India more than 3,000 years ago and is still widely used in that country today.
Those who use it rely on herbs, special diets, and unique practices to treat illnesses. But Ayurvedic products can also be dangerous. Researchers have found toxic minerals or metals, like lead, in some of the products.
There hasn’t been enough research or clinical trials to support that Ayurveda works.