- Overview & Types
- Symptoms & Diagnosis
- Treatment
- Living With
- Related Conditions
- Type 2 Diabetes
- Type 1 Diabetes
- Gestational Diabetes
- Appointment Prep
- View Full Guide
14 Things to Know If Your Kid Has Type 1 Diabetes


You’re in This Together
Close to 20,000 new cases of type 1 diabetes are diagnosed every year. It’s a lifelong condition that can lead to serious complications, especially if it’s not managed well. With careful monitoring and proper use of insulin, you can set your child on the path to a long, healthy life.

Insulin
Type 1 diabetes means your child's body isn’t making enough insulin, a hormone that helps turn sugar into energy. They’ll need to get it several times a day in order to process sugar. They can take it through injections or a pump. You’ll go over the options with your kid’s health care team. Together you’ll craft a plan specific to your child.
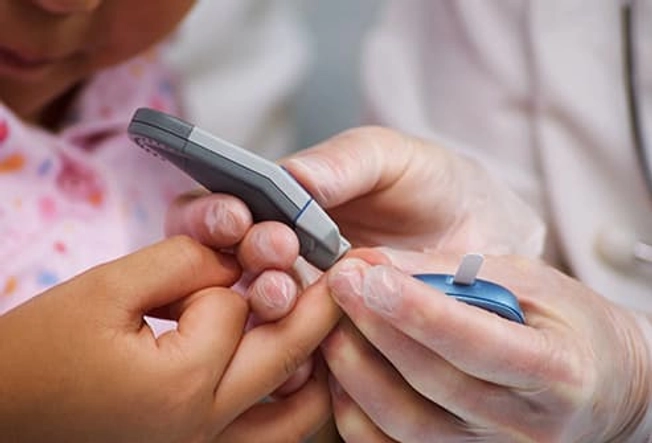
Glucose Level
When your body doesn’t make enough insulin, your blood sugar (or blood glucose) levels can rise too high. You’ll need to carefully monitor your child’s levels all the time. (And when they’re old enough, they’ll need to do it themselves.)
Their doctor and health care team will help you find the right blood-glucose meter for your child and show you how to use it.

Too High, Too Low
If blood sugar levels are too high, it’s called hyperglycemia. The symptoms include dry skin, more thirst, and having to pee often. When levels are too low, it’s called hypoglycemia, or insulin shock. Your child’s symptoms might include headaches, fatigue, chills, and hunger. It’s important to treat it quickly.

Work With a Medical Team
Your child will need to see the doctor at least four times a year. If you’re having trouble controlling their glucose levels, it might be even more than that. If your doctor is making changes in your kid’s care plan, you may need to talk once a week or more.
Having type 1 puts your child at higher risk of other health concerns such as foot, eye, or kidney problems. Your child will need regular eye exams, and you may want to meet with a dietitian, too. You may also want to see a diabetes educator, a professional who helps people understand and manage diabetes.

Eat Well
Diet is also a critical part of managing your kid’s diabetes. You’ll need to read food labels, count carbs, and learn how different foods affect glucose levels. The American Diabetes Association lists some diabetes superfoods -- healthy foods that have a low impact on levels. It includes beans, dark green leafy veggies, some fish, nuts, fruits, and berries. Make sure to have plenty of these in your family's diet.

No Need to Ban Sweets
It’s OK for your kid to have a cookie, some cake, or some ice cream once in a while, as long as you’re monitoring levels and making adjustments.
If your child has a treat, make it a smaller portion, then subtract a sugar-producing carbohydrate (say, potatoes or a roll) from a meal to make up for it.

Meal Timing
When a child eats can affect glucose levels, too. If a meal is later than normal, have your child eat a healthy snack beforehand to maintain a good glucose level. If it’s earlier, monitor to make sure levels don’t get too high.

Keep Moving
Being active -- whether it’s in the back yard or with the local Little League team -- is an essential part of a healthy lifestyle for all kids. Exercise can lower blood glucose levels, which is great -- unless they get too low. Check levels before and after your child plays or exercises.
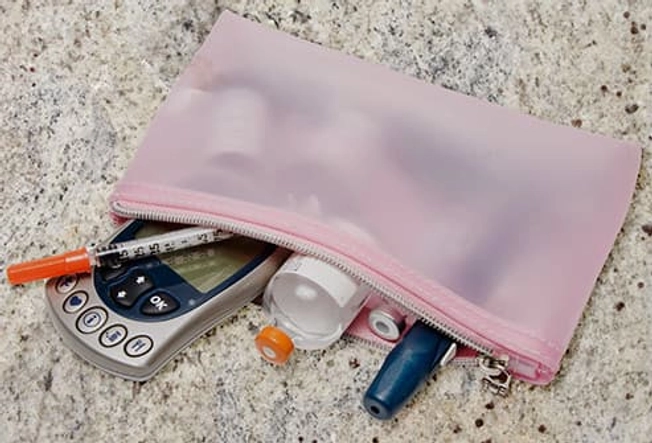
Be Prepared
If your child’s blood sugar gets too high, they’ll need to drink water, take an insulin shot, or exercise.
If they drop too low, they’ll need some fruit juice, hard candy, or glucose tablets.
Your child should have a kit with them at all times. It should include insulin and needles, contact numbers, extra batteries for a meter or pump, test strips and lancets, and a quick-acting source of glucose (like glucose tablets).
They should wear a medical ID at all times that lets people know they have type 1 diabetes.

Let Caregivers Know
Tell people about your child’s diabetes. You can’t be with your child at all times. School principals, nurses, coaches, babysitters, neighbors -- all need to be informed. Make sure they know what to do in case of an emergency. And make sure they know where to find the emergency kit.

Emotional Support
Dealing with a chronic condition that needs to be monitored at all times is a lot for your kid to take on. Along with blood sugar levels, you’ll need to pay attention to your child’s feelings, too. At times, they may feel worried, overwhelmed, and even depressed. Many families find getting a mental health expert involved early on helps.

Growing Up With Diabetes
As your child gets older, you may notice their levels change. And what worked before doesn’t anymore. Hormones and puberty can have an impact. Work with their doctor to keep levels where they need to be. As your child gets older, they’ll learn to manage their diabetes on their own.

Responsible Teenager
When your child gets old enough to drive, they should understand their added responsibilities around driving. Along with taking every other safety precaution, they need to make sure their levels are good before taking the wheel. They’ll need to check them every time and make sure they bring their kit with them.
Your teen also needs to know that alcohol can have dangerous effects on glucose levels. It can make it hard to recognize signs that they’re off and can lead to poor decision-making about correcting levels.