- Overview & Types
- Symptoms & Diagnosis
- Treatment
- Living With
- Related Conditions
- Type 2 Diabetes
- Type 1 Diabetes
- Gestational Diabetes
- Appointment Prep
- View Full Guide
Slideshow: A Visual Guide to Type 1 Diabetes

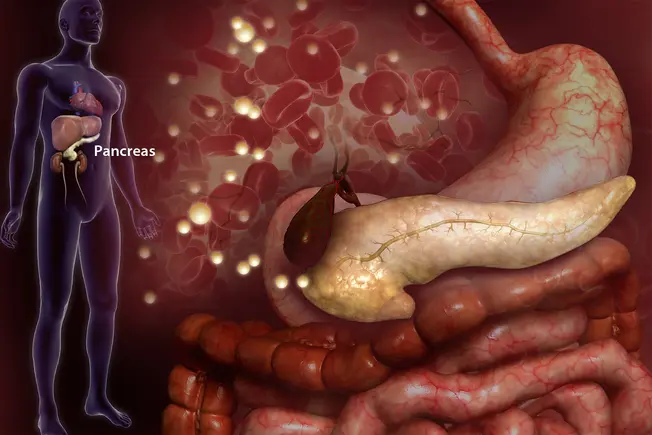
What Is It?
When you have type 1 diabetes, your pancreas can’t make insulin. This vital hormone helps your body's cells convert sugar into energy. Without it, sugar builds up in your blood and can reach dangerous levels. To avoid life-threatening complications, people with type 1 diabetes must take insulin for their entire lives.

Early Warning Signs
The symptoms of type 1 diabetes tend to come on suddenly and may include:
- Feeling more thirsty than usual
- Dry mouth
- Fruity breath
- Peeing a lot

Later Red Flags
As blood sugar levels remain high, type 1 diabetes often leads to:
- Weight loss
- Bigger appetite
- Lack of energy, drowsiness

Skin Problems
Many people with type 1 diabetes get uncomfortable skin conditions, including:
- Bacterial infections
- Fungal infections
- Itching, dry skin, poor circulation
Girls with type 1 diabetes are more likely to have genital yeast infections. Babies can get candidiasis, a severe form of diaper rash caused by yeast. It can easily spread from the diaper area to the thighs and stomach.

Dangerous Complications
When blood sugar isn't controlled, type 1 diabetes can cause more serious symptoms, like:
- Numbness or tingling in the feet
- Blurred vision
- Chest pain
- Passing out
If your blood sugar gets too high or too low, you could go into a diabetic coma. You may not have any warning signs before this happens. You will need to get emergency treatment.

Ketones and Ketoacidosis
Without treatment, type 1 diabetes deprives your cells of the sugar they need for energy. Your body starts burning fat instead, which causes ketones to build up in the blood. These are acids that can poison your body. This plus other changes in your blood can trigger a life-threatening condition called diabetic ketoacidosis. This is an emergency that must be treated quickly. You may need to go to the ER.
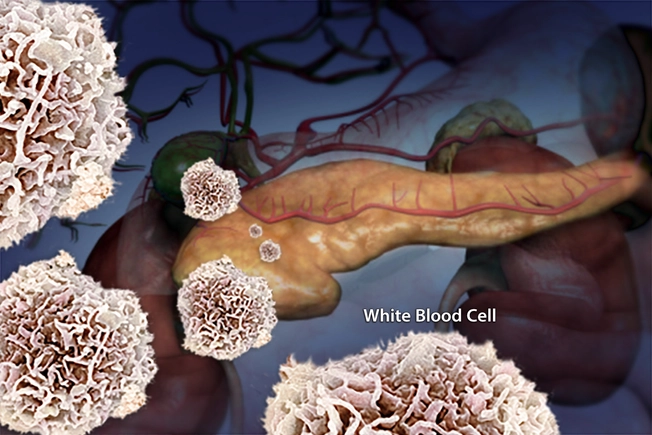
Type 1 vs. Type 2 Diabetes
In type 1 diabetes, your immune system destroys cells in your pancreas that make insulin. In type 2 diabetes, the pancreas isn’t under attack. It usually makes enough insulin. But your body doesn’t use it well. The symptoms of hyper and hypoglycemia are similar, but usually come on more quickly in people with type 1.

What Causes It?
Doctors aren't sure what makes your immune system attack the pancreas. Scientists have found 50 genes or gene regions that make you more likely to get type 1 diabetes. But that alone doesn’t mean you will. Some researchers believe that environmental triggers also play a role. These could include a virus or things that happen to your body during pregnancy.

Who Gets It?
Type 1 diabetes can happen at any point in life. But it's mostly diagnosed before the age of 19. It affects boys and girls equally, but it's more common in whites than in other ethnic groups. According to the World Health Organization, type 1 diabetes is rare in most African, Native American, and Asian people.

How Is It Diagnosed?
Your doctor will probably check your fasting blood sugar or they may do a random blood sugar test. They could also get your A1c level, which shows average blood sugar readings for the past 2-3 months. The tests should be repeated on 2 separate days. A more complex glucose tolerance test could also help them make the call. In type 1, checking a c-peptide can be helpful because it is a breakdown product of insulin and will be absent in type 1 diabetes.
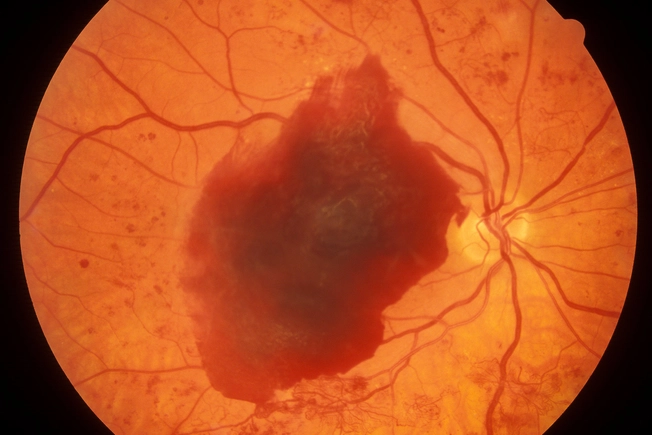
Long-Term Problems
Having high blood sugar for a long time can damage many of your body's systems. Type 1 diabetes can make you more likely to have:
- Heart disease and stroke
- Kidney failure
- Blindness or other problems seeing
- Gum disease and tooth loss
- Nerve damage in the hands, feet, and organs

Check Your Blood Sugar
The first step toward preventing complications is to keep track of your blood sugar (also called blood glucose). You'll prick a finger, put a drop of blood onto a test strip, and slide the strip into a meter. The results will help you make the most of your treatment plan. When your levels are near the normal range, you'll have more energy, fewer skin problems, and a lower risk of heart disease and kidney damage.
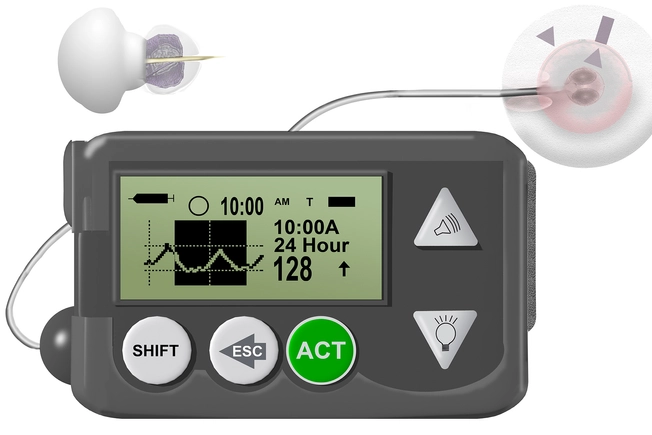
Could a Continuous Glucose Monitor Help?
This tool can be used for daily management. It uses a sensor to measure the level of glucose in your body every 10 seconds. It sends the information to a cell phone-sized device called a "monitor" that you wear. The system has alarms for high and lows so they are safer for folks at risk for hypoglycemia while sleeping. They automatically records your average reading for up to 72 hours.
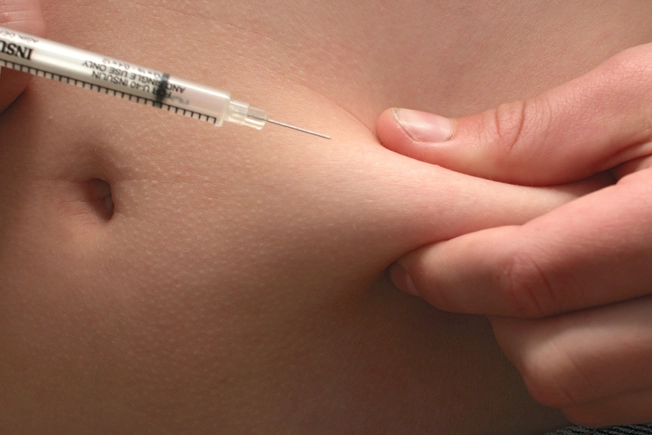
Treatment With Insulin Shots
Everyone with type 1 diabetes must take insulin. Most people take it as an injection and need multiple shots per day. Your doctor will explain how to adjust the amounts based on the results of your blood sugar tests. The goal is to keep your levels in the normal range as often as possible.

How to Spot an Insulin Reaction
This happens when insulin lowers your blood sugar to dangerous levels. It can be mild, moderate, or severe. Warning signs include:
- Exhaustion or yawning too much
- Being unable to speak or think clearly
- Loss of muscle coordination
- Sweating, twitching, turning pale
- Seizures
- Loss of consciousness

How to Treat an Insulin Reaction
Carry at least 15 grams of a quick-acting carbs at all times. They bring your blood sugar up quickly to fight the reaction. Some examples are:
- 1/2 cup of fruit juice or non-diet soda
- 1 cup of skim or 1% milk
- 2 tablespoons of raisins
- 3 glucose tablets or 5 hard candies
If your blood sugar is still too low after 15 minutes, have another 15 grams.
If you pass out, you'll need help from those around you. Wear an ID bracelet that says you're a diabetic, and carry a glucagon kit. This drug can be injected under your skin. Tell a friend or family member how to spot the signs of a reaction and show them how to give you the shot.
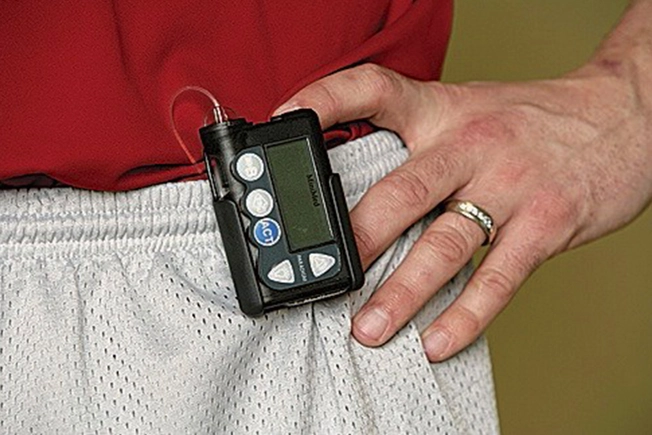
Insulin Pumps: Safer Than Shots?
This device can lower the odds of a reaction. It provides insulin around the clock through a tiny tube inserted into your skin. You no longer need to take shots. It can help keep your blood sugar stable and may allow more freedom in planning meals. There are some drawbacks, so ask your doctor if this option is right for you.

Is Your Treatment Working?
Your doctor will probably suggest you have an A1c blood test every 3 to 6 months. It shows how well your blood sugar has been controlled over the past 2 to 3 months. If the results aren’t good, you may need to adjust your insulin dose, meal planning, or physical activity.
If Insulin Doesn't Work
This is a last resort. Insulin always works, but it may be that the side effects are not tolerable or the end-stage disease is already too great. Your doctor might suggest a pancreatic islet cell transplant. In this experimental procedure, a surgeon transfers healthy insulin-making cells from a donor into your pancreas. There’s a downside: The results may last only a few years. And you’ll have to take drugs to prevent rejection. These can have serious side effects.
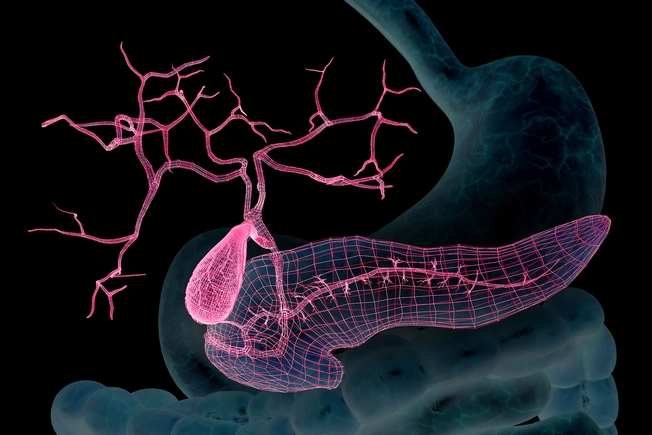
Hope for an Artificial Pancreas
Researchers are working on a system called the artificial pancreas. This combination of an insulin pump and continuous glucose monitor is controlled by a complex computer program. The goal is for it to work like the real thing. That means it will adjust the insulin it puts out in response to rising or falling blood sugar levels. Early trials suggest it can improve blood sugar control.

Exercise With Caution
You need to get some physical activity, but be careful when you do it. To prevent a sudden drop in blood sugar, your doctor may tell you to do these things before you exercise:
- Check your blood sugar
- Adjust your insulin dose
- Eat a snack
They may also suggest checking your pee for ketones, a sign that your blood sugar is too high. Avoid hard exercise when they are present.

What Can You Eat?
There are many myths about what people with diabetes can and can't eat. The reality is there are no "off-limits" foods. You can have sweets as part of a well-balanced diet and treatment plan. The key is to work with your health care team to balance your insulin shots, meals, and physical activity.
Should You Get Pregnant?
Let your doctor know if you plan to have a baby. If your diabetes isn’t well controlled, it can cause complications, including birth defects. Good control of blood sugar before you get pregnant lowers your odds for these problems and for miscarriage. Your risk of eye damage and dangerous spikes in blood pressure will go down, too.
Children and Diabetes
When a child is diagnosed with diabetes, it affects the whole family. Parents must help children check blood sugar, plan meals, and adjust insulin doses around the clock. The disease requires 24-hour maintenance, so you also have to make plans for treatment during school and activities afterward. Check with your child's school to see who can give insulin if they need it.