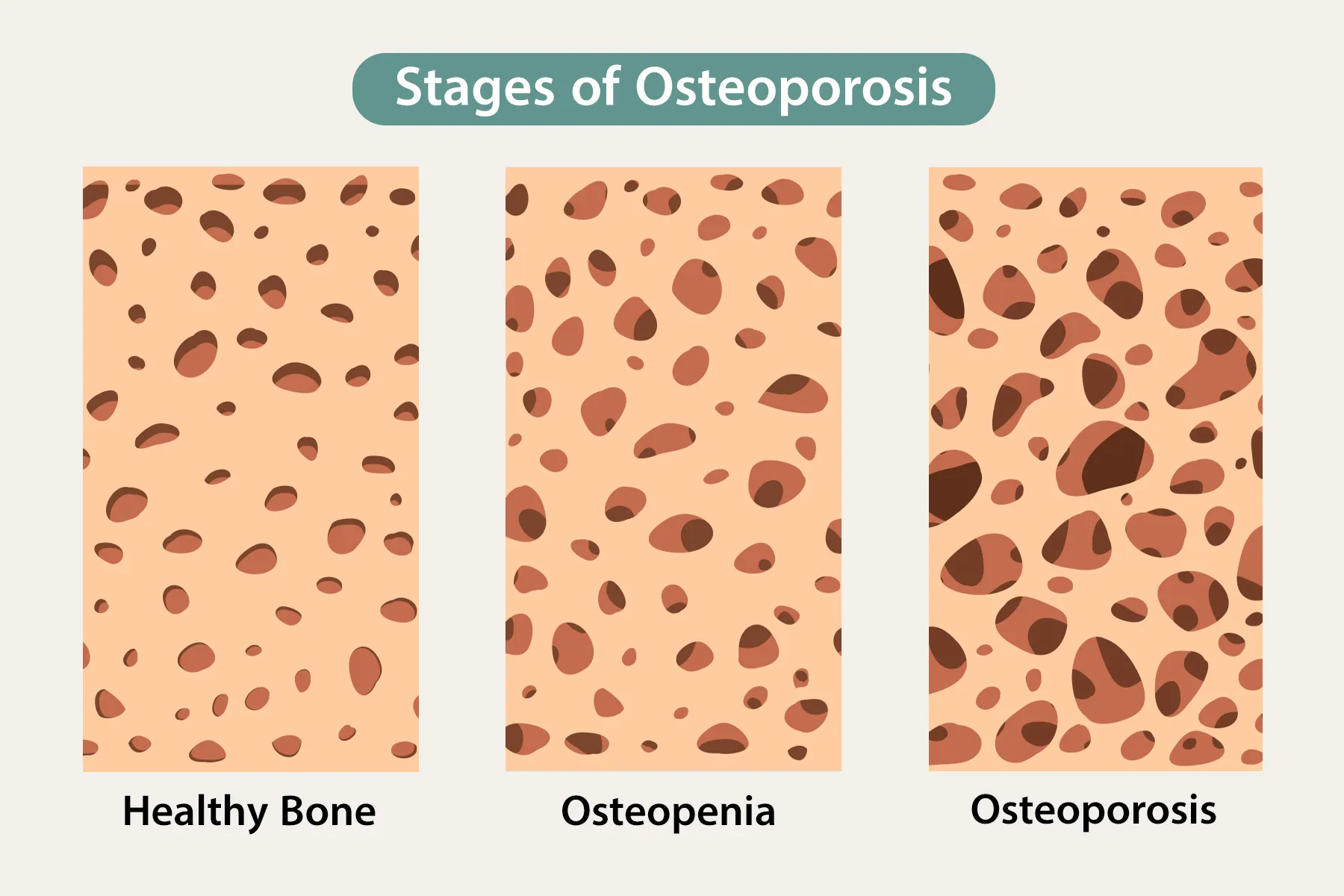
When you have osteopenia, your bones are weaker than they used to be, but they're not weak enough for you to be diagnosed with osteoporosis. That’s a condition in which your bones are so thin they break easily. If your bones keep getting thinner over time, osteopenia can turn into osteoporosis.
But it doesn’t have to. A range of osteopenia treatments and healthy habits can strengthen your bones, slow osteopenia, and prevent osteoporosis.
Osteopenia Self-Care
If you have strong bones, a healthy lifestyle can help keep them that way. If you already have osteopenia, those same lifestyle choices can lower the chances you’ll get osteoporosis. Consider the following tips to maintain the health of your bones:
Osteopenia and e xercise
Like muscles, bones get stronger when you use them. The best moves for bones are weight-bearing exercises that force your body to work against gravity. That includes walking, stair climbing, dancing, and lifting weights.
Osteopenia and diet
For strong bones, you need a diet rich in calcium and vitamin D. High-calcium foods include:
Your body makes its own vitamin D when sunlight hits your skin. If you spend a few minutes outdoors in the sunshine each day, you get at least some of the vitamin D you need. Don’t spend too much time in the sun, though -- that raises your risk of skin cancer. A few foods naturally have vitamin D, while others such as grains and dairy foods are fortified with it. Good sources include:
- Fish such as salmon, tuna, and mackerel
- Fish liver oils
- Beef liver
- Cheese
- Egg yolks
- Fortified breakfast cereals, juices, milk products, yogurt, and margarine
Don’t smoke, and drink less. If you smoke, try to quit. Studies show a strong link between cigarette smoking and lower bone density.
If you drink alcohol, do it in moderation. That means no more than one drink per day for women and two daily drinks for men. Too much beer, wine, or liquor can mess with the balance of calcium in your body and change how your body makes hormones and vitamins for healthy bones. Having too much to drink can also make you more likely to fall, which means you could break a bone.
Cut back on salt and caffeine. Both may make your body lose more calcium and bone. Caffeinated coffee and sodas have been linked to osteopenia, so try to cut back or switch to the decaf kinds. Check labels of packaged foods to see how much salt (or sodium) is in a serving.
Other ways to manage osteopenia at home
Falls are much more likely to cause fractures when you have osteopenia. Lower your risk of falls by:
- Getting rid of obstacles in your home that may cause you to trip, such as loose rugs or electronic cords
- Adding railings to your shower or bathtub walls
- Limiting your use of sleep medications
- Wearing your glasses or contacts if you need them
Osteopenia Medications
In some cases, especially if you’ve already broken a bone, your doctor may prescribe medicine to lower your chances for osteoporosis and prevent more fractures. Medications that can treat osteopenia or prevent osteoporosis include:
Bisphosphonates. These meds slow your body’s natural process of breaking down bones. You may keep the level of bone you have or even get a small boost of bone density. Bisphosphonates are the main drugs doctors use to prevent and treat osteoporosis in postmenopausal women. They include alendronic acid (Fosamax), ibandronic acid (Boniva), risedronic acid (Actonel), and zoledronic acid (Reclast). Most bisphosphonates are pills you take usually once a week or once a month. But Reclast comes as an injection, usually once a year.
Hormone replacement therapy. Once a popular treatment to prevent bone loss, doctors rarely use it now because studies found that it made people more likely to get blood clots in their legs and lungs, along with other health problems. Sometimes, if hormone replacement helps someone with menopause symptoms, their doctor may recommend that they keep taking it for bone loss too. Talk to your doctor to see if you should consider this therapy.
Teriparatide (Forteo). It acts like a hormone made by your parathyroid glands. It's the first medicine to help the body make new bone tissue. You take it daily as a shot beneath your skin.
Raloxifene (Evista). This drug can prevent and treat osteoporosis. It may also lower your chances of getting breast cancer, but scientists need more research to know that for sure. It’s a pill you take once a day.
Each of these drugs has its own risks and possible side effects, so make sure you talk with your doctor about how they will affect you before you take them.
Natural Treatments for Osteopenia
Your doctor may recommend medications if you’ve already broken a bone. But many people try several nutritional supplements and herbs before they have a fracture to build stronger bones. The main ones are calcium and vitamin D supplements.
Osteopenia supplements
Most adults should get 1,000-1,200 milligrams of calcium and 600-800 international units (IU) of vitamin D every day. Vitamin D helps your body absorb more calcium, and both nutrients support your overall bone health. If you aren't getting enough of either in your diet and you don't spend much time in the sun, ask your doctor if you should take a supplement. Many are available over the counter, though your doctor may prescribe you one if necessary.
Other nutritional supplements may help strengthen bones, but so far, there’s little research showing how well they work. These include:
- Boron
- Copper
- Dehydroepiandrosterone (DHEA)
- Eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA) -- the two omega-3 fatty acids found in fish
- Folic acid, vitamin B6, and vitamin B12
- Manganese
- Silicon
- Strontium
- Zinc
Herbs that might be helpful include:
- Black cohosh
- Horsetail
- Red clover
Before you take any herbal or nutritional supplements, talk to your doctor about them.
Takeaways
Everyone loses some bone density as they age, but without treatment, osteopenia could progress into osteoporosis. If you're not getting enough calcium and vitamin D through your diet, your doctor may recommend supplements to boost your intake of these bone-strengthening nutrients. But if you've already broken a bone, your health care provider may recommend a prescription to help prevent further bone loss and lower your risk of future fractures.
Osteopenia FAQs
How do you stop osteopenia from progressing?
Keep active and get enough calcium and vitamin D through your diet and supplements to keep your osteopenia symptoms from getting worse.

