Yes. You should plan to make regular eye doctor visits when you have diabetes. High blood sugar can lead to problems like blurry vision, cataracts, glaucoma, and retinopathy. In fact, diabetes is the primary cause of blindness in adults ages 20 to 74.
Blurry Vision
Don't buy new glasses as soon as you notice that things look blurry. It could just be a small problem caused by high blood sugar. Your lens could swell, which changes your ability to see.
To correct it, you need to get your blood sugar back into the target range (70-130 milligrams per deciliter, or mg/dL, before meals, and less than 180 mg/dL 1 to 2 hours after a meal). It may take as long as 3 months for your vision to fully get back to normal.
Do tell your eye doctor. They can let you know if this is a symptom of a more serious problem.
Cataracts
The natural internal lens of your eye allows your eye to see and focus on an image, just like a camera. When that lens gets cloudy, like a dirty or smudged window, that means a cataract has formed. Anyone can get them, but people with diabetes tend to get them earlier, and they get worse faster.
When part of your lens is cloudy, your eye can’t focus like it should. You won't see as well. Symptoms include blurred vision and glare.
You’ll need surgery to remove a cataract. The doctor replaces the cloudy lens with an artificial one.
Glaucoma
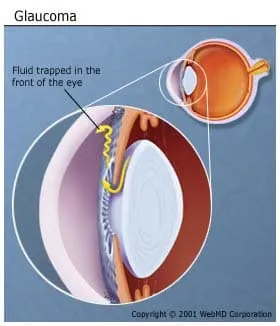
People with diabetes are more likely to have glaucoma, which can come in several forms or types.
Pressure builds up inside your eye when fluid can’t drain like it should. This can damage nerves and blood vessels, and cause changes in vision.
Medications can treat open-angle glaucoma, the most common form. They lower eye pressure, speed up drainage, and reduce the amount of liquid your eye makes. (Your doctor will call this aqueous humor.)
This type of glaucoma may not cause any symptoms until it’s further along and you have major vision loss. Your doctor can catch it earlier, during an annual exam.
With less common forms of the disease, you might notice:
- Headaches
- Eye aches or pain
- Blurred vision
- Watery eyes
- Halos around lights
- Vision loss
Treatment can include medicine and special eye drops. Surgery and laser treatments can help lower eye pressure.
If you have diabetes, you’re also more likely to get a rare condition called neovascular glaucoma. This makes new blood vessels grow on the iris, the colored part of your eye. They block the normal flow of fluid and raise eye pressure.
The primary treatment of neovascular glaucoma is to reverse the formation of new blood vessels. For this, your doctor may use a laser to reduce the number of blood vessels in the back of the eye, or they may use an anti-VEGF injection, while using other measures to quickly lower the eye pressure.
Diabetic Retinopathy
The retina is a group of cells on the back of your eye that take in light. They turn it into images that the optic nerve sends to your brain.
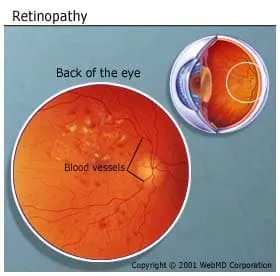
Damage to small blood vessels in your retina causes diabetic retinopathy. It's related to high blood sugar levels. If you don’t find and treat it early, you could go blind. The longer you have diabetes, the more likely you are to get it. If you keep your blood sugar under control, you lower your chances.
People with type 1 diabetes rarely develop the condition before puberty. In adults, it's rare to see unless you've had type 1 diabetes for at least 5 years. If you keep tight control of your blood sugar with either an insulin pump or multiple daily insulin injections, you’re far less likely to get this condition.
If you have type 2 diabetes, you may have signs of eye problems when you’re diagnosed. Control your blood sugar, blood pressure, and cholesterol to slow or prevent the disease. If you smoke, try to quit. It’ll improve your eyes and your overall health.
There are other types of this condition:
Background retinopathy. Your blood vessels are damaged, but you can still see OK. It can get worse if you don't manage your diabetes well.
Maculopathy. This occurs when diabetes affects the macula. The macula is the area of your retina that provides the best vision necessary for reading, driving, and other similar activities. The swelling that occurs may be easily reversible, or more serious and difficult to treat.
Proliferative retinopathy. It happens when cells at the back of your eye don’t get enough oxygen and new blood vessels start to grow. They’re fragile, so they can bleed and lead to a clot. This can cause scars and pull your retina away from the back of your eye. If it gets detached, you could have vision loss that can't be fixed. Sometimes this condition can be treated. Surgery is an option, so is a laser procedure that burns away the blood vessels. It can prevent blindness in up to half the people with early retinopathy.
The Need for Eye Exams
A full yearly checkup can help find problems early, when they're easier to treat. That could save your vision.
If you might get pregnant in the near future, get an eye exam to avoid possible problems. Keep them up while you’re pregnant, too.
When to Call the Doctor
These symptoms can signal an emergency:
- Black spots in your vision
- Flashes of light
- "Holes" in your vision
- Blurred vision

