Your doctor can choose from many imaging tests to help them diagnose and keep track of your Crohn’s disease. One of the most common is an abdominal X-ray. It helps them see parts of your digestive tract that other tests can’t show.
But these aren’t ordinary X-rays. They use a process called fluoroscopy. You’ll get either a drink or an enema that contains barium or iodine. Both of these substances stick to the walls of your intestines and make them easier to see than on a regular X-ray. The X-ray is beamed to a special machine that converts it to a video and sends it to a TV-like monitor. This lets your radiologist follow the barium or iodine through your GI tract.
Abdominal X-rays for Crohn’s
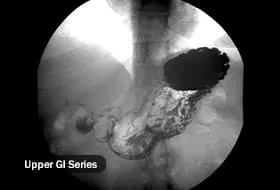
- Upper GI series or barium swallow: You might also hear this called a barium or contrast X-ray. This type of X-ray shows the doctor your esophagus, stomach, and the first part of your small intestine (they'll call this your duodenum). You’ll get a chalky-tasting drink made of barium and water. It coats the inner walls of your esophagus and intestines.
- Air contrast or double contrast GI studies: For an even more detailed image, the doctor might add baking soda crystals to the barium drink. They’ll make it fizz, like those tablets you dissolve in water when you have heartburn.
- Barium small-bowel follow through: Doctors usually do this test after an upper GI series to show details of your small intestine. You’ll drink a barium or iodine drink to coat your intestinal walls and help problem areas show up on the X-ray.
Lower GI series or barium enema: This helps the doctor see the right or ascending colon, the transverse colon, and the left or descending colon, all parts of your large intestine. It can also show your appendix and the end of your small intestine. Instead of drinking the mix of barium and water, you’ll get it as an enema. This means a radiologist or technologist will slide a small tube inside your bottom to get the liquid into your colon. Some doctors might use iodine and water instead. Doctors do this test in one of two ways: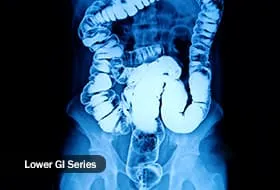
- Single contrast image: Your entire large intestine is filled with the barium liquid. This helps the doctor see large masses or major problems with the intestine.
- Double contrast image: You’ll get a smaller amount of barium in the enema, followed by air. This creates a thin film of barium on your intestinal wall and makes it easier for the doctor to spot problem areas.
Preparing for Upper and Lower GI Exams
Preparation for upper GI or lower GI tests usually includes following a low-fiber diet for 2 to 3 days before the test, not smoking for 12 to 24 hours before the test, not taking certain medications for up to 24 hours before the test, and not eating anything for 12 hours before the test. Your doctor will give you specific instructions. Never stop taking any medications without first discussing it with your doctor.
Additional preparation for the lower GI test usually includes taking oral laxatives and an enema the night before the test. Carefully follow the pre-test directions given to you by your doctor.
What Happens During an Upper GI Test?
- The technologist will help you get into position on an exam table. Some places may use an X-ray table that tilts.
- You’ll take the baking soda crystals, if you’re having that test, then drink the barium. Although the barium solution doesn’t taste good, there’s no pain and little discomfort during the procedure.
- If you’re on an adjustable table, it usually starts in a vertical position, with you standing. For a regular table you’ll get on the table and lie in different positions. This helps spread the barium around. Most of the X-rays will be taken with you lying down. You’ll be asked to hold your breath before each.
- The process usually takes 30 minutes.
What Happens During a Lower GI Test?
- The technologist will help you get into position on an exam table. Some places may have an adjustable table, but they’ll probably start with it in the horizontal position.
- A technologist or radiologist will give you the enema. If you’re getting a double contrast X-ray, they’ll follow it up with air.
- You’ll move from side to side to help the liquid coat your intestine or the technologist will tilt the table at various angles. During the test, the radiologist may put pressure on your abdomen to get a clearer image.
- The test may cause some discomfort, including cramps and a strong urge to have a bowel movement.
- After the first set of X-rays, someone will help you to the bathroom (or give you a bedpan) so you can move your bowels to get rid of as much of the barium as possible. Then you’ll go back to the exam room for more X-rays of the barium solution that remains on your intestinal wall. The technologist may inject more air into your colon for more contrast on the images.
- The test should take between 30 minutes to an hour.
What Happens After the Tests?
You should be able to go back to your usual activities and normal diet immediately after your GI tests. Unless your doctor tells you to restrict fluids for another medical condition, drink plenty of water or juice -- eight to 10 glasses each day for 3 days -- to get the barium out of your colon.
It’s normal to have a white or light stool for up to 3 days after the test The barium enema you get during a lower GI test could leave you feeling weak or dizzy. Ask your doctor what else you might expect to feel after the test.
When Will I Get Results?
Probably within a day or two. It doesn’t take all that long to develop the X-ray film, but your doctor will have to look at it and decide what the results say, then contact you.
Are There Risks for GI Tests?
There’s almost no risk with the upper and lower GI tests, unless you have to repeat them several times within a few months. Although radiation exposure from these tests is minimal, it’s still more than for standard still X-rays. But the technologists will take steps to minimize your exposure.
Other risks include:
- Infection (very low risk with both the upper and lower GI tests)
- Tearing the intestinal wall during a lower GI test. This is rare, but if it happens, you may need surgery.
Who Shouldn’t Get GI Tests?
If you have an existing blockage or tear in the intestinal wall.
If you’re pregnant or think you might be pregnant. Talk to your doctor about other tests that can be more safely performed to diagnose your problem during pregnancy.
When to Call Your Doctor After GI Tests
Call the doctor if you have:
- A temperature of 101 degrees Fahrenheit or higher. This could be a sign of infection and should be treated right away.
- A marked change in bowel habits, like no bowel movement in 2 or 3 days after the test. It’s normal for your poop to be white or light colored for up to 3 days after the test.
- Worse pain
- Unusual drainage from your rectum
- Any symptoms that cause concern
- Questions about the test or the results

