- Overview & Types
- Symptoms & Diagnosis
- Treatment
- Living With
- Related Conditions
- Type 2 Diabetes
- Type 1 Diabetes
- Gestational Diabetes
- Appointment Prep
- View Full Guide
Chronic Conditions Common in Minorities


How Race and Ethnicity Affect Health
Racial and ethnic minorities in the U.S. are more likely to have ongoing health conditions. These differences are caused by several factors. They include:
- Less access to high-quality health care
- Fewer social and economic advantages
- Discrimination and racism
- Mistrust in the health care system
- Genetic, cultural, and lifestyle differences
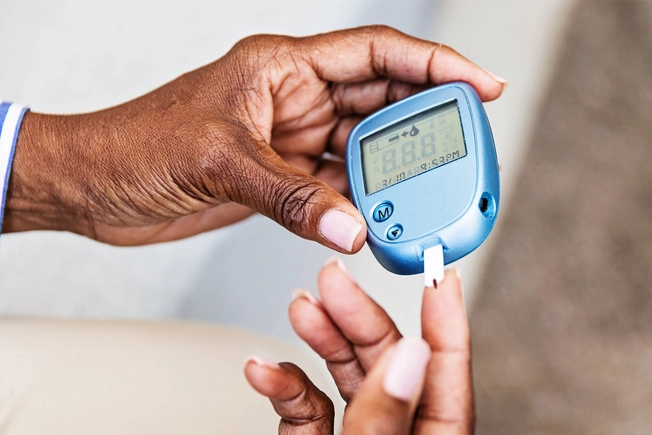
Diabetes
American Indians and Alaska Natives are most likely to be diagnosed with high blood sugar, followed by Black, Hispanic or Latino, and Asian Americans. Minorities also have more complications from diabetes, such as heart disease, eye damage, kidney disease, nerve problems, and even death. The Office of Minority Health and Healthy Equity is working to address these differences. One goal is to include more minorities in research that tests new diabetes drugs and treatments.
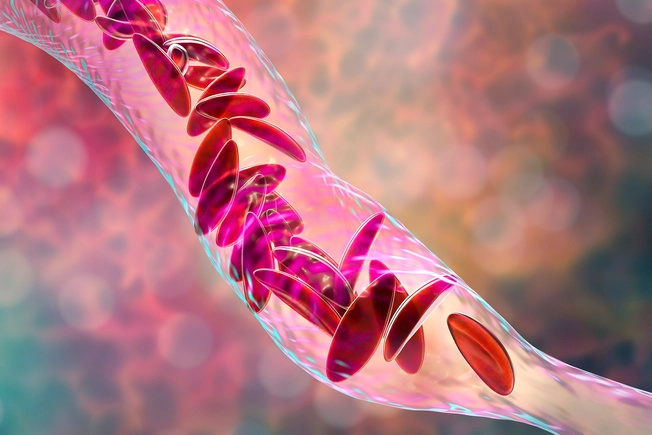
Sickle Cell Disease
This condition mainly affects Black people. Studies show those with this condition don’t always get fast or good treatment for their symptoms, including pain. That may be because some doctors believe Black people feel pain less than other races. Studies also show some doctors are more likely to believe people with sickle cell disease abuse pain medication. Sickle cell disease doesn’t get as much funding as other genetic disorders, like cystic fibrosis. That’s a condition that mostly affects white people. Experts think this might be why there aren’t as many new drug options for sickle cell disease.
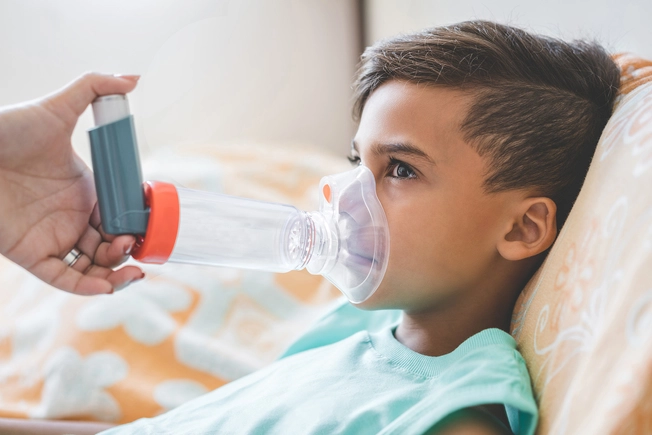
Asthma
This condition greatly affects Black and Hispanic people, particularly those from Puerto Rico. Black people are more likely to end up in the emergency room because of asthma. They’re also more likely to die from it. A large genetic study found that the most-used asthma inhaler, albuterol, doesn’t work as well in Black or Puerto Rican children. Studies also show air pollution hits communities of color -- especially Black ones -- harder. Bad air quality can lead to lung problems.

High Blood Pressure
Close to half of Black adults have hypertension. That’s the medical term for high blood pressure. Compared to other groups in the U.S., high blood pressure is more likely to show up at an earlier age in Black people and lead to serious complications. Experts aren’t sure why. It’s likely that genetic, lifestyle, and social factors -- including a lifetime of discrimination -- all play a role.

Obesity
Experts aren’t sure why it’s slightly higher in Black and Hispanic adults. The social and economic disadvantages some face may play a role. For instance, depending on where they live, some may not have easy access to a grocery store with fresh fruits and vegetables. They also may not have sidewalks and other things that make exercise easier. Obesity also raises the chance you’ll have other health problems. These include heart disease, stroke, type 2 diabetes, and certain kinds of cancer.

Cardiovascular Disease
Non-Hispanic Black adults are more likely to die from heart disease. They also have a much higher chance of having a serious or fatal stroke. That’s likely because heart and blood vessel problems are linked to other diseases high among minorities.
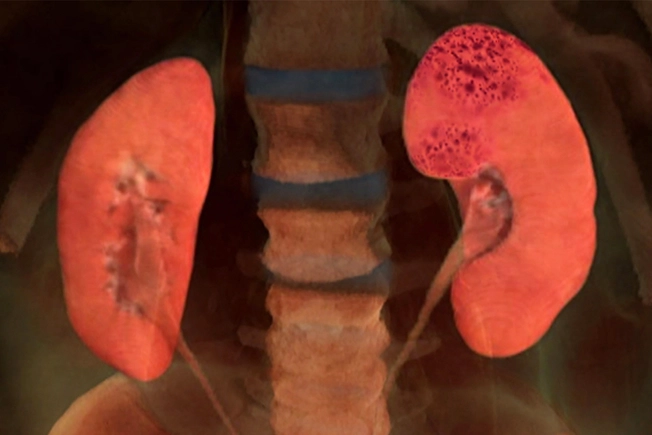
Kidney Disease
This condition affects Black people more than any other group. They’re almost four times more likely to die of kidney failure. Hispanic and American Indian people also are more at risk. Diabetes and high blood pressure are the main causes.

HIV/AIDS
Black people are 13% of the U.S. population, but they make up about 42% of HIV diagnoses. The rate of infection is highest for Black males at 31%. Black females are more than 18 times as likely as white females to have AIDS. Some researchers think the mass incarceration of Black men in America worsens these HIV-related health disparities.

Cancer
Black males are more likely to be diagnosed with and die from common cancers. These include prostate, lung, and colon cancers. Black females are less likely to be diagnosed than white females, but they’re more likely to die from cancer if they do get it. Rates of kidney cancer and deaths are highest among American Indians and Alaska Natives. Liver cancer rates are greatest for people who are American Indian, Alaska Native, Asian, or Pacific Islander.

Breast Cancer
Studies show doctors tend to find breast cancer earlier in white women, when it’s easier to treat. Black women are more likely to get triple-negative breast cancer. That’s a fast-growing form of cancer that often comes back after treatment.

Lupus
Lupus happens more often in Black females than non-Hispanic white females. It’s also more likely to show up in Black females at a younger age and cause serious kidney damage. Rates of lupus are also higher among Hispanic and Native American women.
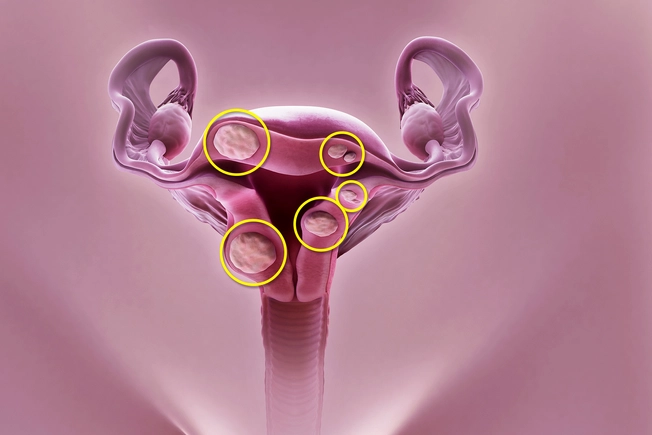
Uterine Fibroids
These noncancerous growths show up in Black women at a higher rate and younger age. They’re also more severe. Doctors can do a surgery called a myomectomy to take out fibroids, but new ones may grow. A hysterectomy is the only cure. That’s surgery to remove the uterus. Studies show Black females are more likely to end up in the hospital for fibroids and get a hysterectomy.

The All of Us Research Program
One organization that is working to find out why certain diseases affect some groups differently than others is the All of Us Research Program. All of Us wants to empower researchers with information to help them better understand what makes us unique. To do that, they’re asking 1 million or more people to share their health data. The program aims to reflect the diversity of the U.S. and to include participants from groups underrepresented in health research in the past. The program is developing custom tools and software to help researchers analyze participant data while keeping information secure.