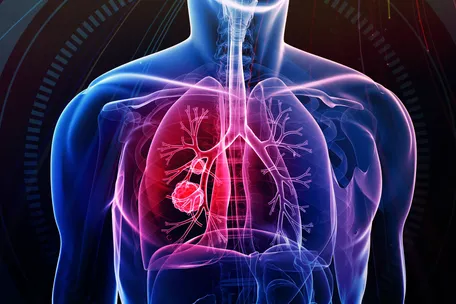
SPEAKER 1: There are two
major types of lung cancers,
which can affect smokers
and non-smokers alike,
small-cell lung cancer
and non-small-cell lung cancer.
JAMIE CHAFT: I would say,
interestingly, despite all of us
using "non-small-cell lung
cancer" in our everyday lingo,
it actually isn't a thing.
So, "non-small-cell lung cancer"
is a historic term, and it
really meant just that, not
small-cell lung cancer.
SPEAKER 1: Doctors now recognize
it's a group of cancer
diagnoses,
including adenocarcinoma,
squamous cell carcinoma,
and a host of rare subtypes.
As researchers have moved
beyond the historic lingo
and narrowed in on these more
specific conditions, they've
started making advances
on this biological chessboard.
But doctors still haven't found
their checkmate.
JAMIE CHAFT: It's very exciting.
As a field, it is constantly
changing.
And it certainly keeps us
on our toes.
SPEAKER 1: While people may
still be diagnosed
with non-small-cell lung cancer,
how they're treated
depends on what their cancer
actually looks
like under a microscope.
Old-school chemotherapy can help
some people live longer,
healthier lives.
But scientists have made
big advances
in targeted therapies,
including immunotherapies, which
help the body's
own immune system attack cancer
cells,
and a class of drugs called
"small molecule inhibitors."
Researchers have found
that some people's tumors can
have just one genetic change
that can lead
to cancerous cells.
These powerful mutations are
called "drivers."
JAMIE CHAFT: And we have found
that, in the lab,
drugs have been developed
that are highly
specific at blocking
these abnormal proteins.
And it's like stepping
on the gas
and letting the car go,
where we now have medicines
that, not permanently,
but at least with some degree
of durability,
can step on the brake.
SPEAKER 1: The first
of these inhibitors targeted
a protein called
the "epidermal growth factor
receptor," or EGFR.
Researchers found that many lung
cancers had surfaces littered
with the excess product
of EGFR proteins,
so they developed
an EGFR inhibitor to suppress
these growth factors.
It worked, slowing the growth
of cancer cells.
JAMIE CHAFT: And that was pretty
revolutionary.
And since then, we've found
many different genes for which
targeted therapies can be
designed and prescribed
in the clinic.
SPEAKER 1: These include
inhibitors for genes like ELK,
MET, RET, KRAS, and more.
But there's still plenty of room
for improvement.
JAMIE CHAFT: I envision
that, in the future,
lung cancer care is going to be
exceptionally different.
SPEAKER 1: Right now,
targeted therapies are
slow to start, because doctors
need lots of data,
including tumor biopsies,
to make sure they're choosing
the right treatment.
The wait can be
hard on patients.
JAMIE CHAFT: And, as a provider,
we do our best to reassure
people that the best therapy is
usually far better
than a quick therapy,
and it's something that's often
really hard to wrap your head
around.
In 20 years, we will likely
be making our diagnoses based
on a blood test, not
on a biopsy, and we'll probably
be monitoring therapy based
on serial blood tests, where we
can track the tumor
and its evolution
through the blood,
and hopefully target and tailor
therapy to be maximally
effective in that setting.
SPEAKER 1: Researchers will also
continue to improve
on immunotherapies through
research on the patients who
respond well to the treatment
and those who don't.
JAMIE CHAFT: My personal wish
list is to improve cure rates,
and really to take all
of these interventions
that we've shown
to be
beneficial in stage-four disease
and move them into the earlier
stage.
SPEAKER 1: But here's one move
patients and providers can make
today.
JAMIE CHAFT: We still need
the primary care physicians
and the pulmonologists
across the country to believe
in lung cancer screening,
and to believe that we can
change outcomes if we screen
and identify these cancers
earlier.