Lipodystrophy is a problem with the way your body uses and stores fat. It's called acquired when you aren't born with it. It often affects the fat that’s just under your skin, so it can change the way you look. It also can cause other changes in your body.
Some people with HIV get lipodystrophy (LD-HIV). It may be related to the medicines they take or the disease itself.
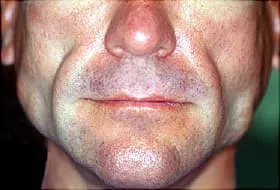
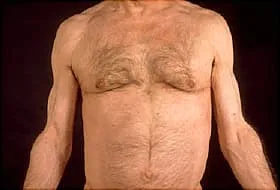
Other acquired lipodystrophies are:
- Acquired generalized lipodystrophy (AGL), or Lawrence syndrome
- Acquired partial lipodystrophy (APL), also called progressive lipodystrophy or Barraquer-Simons syndrome
- Localized lipodystrophy
AGL often shows up in children, but adults can get it, too. APL typically starts around ages 8-10. Both conditions affect girls 3 times more often than boys. Both cause a person to lose fat from their face, so they may look sick or much older than they are.
Localized lipodystrophy can happen to anyone at any age. A small dimple of localized lipodystrophy may look odd, but it probably won't cause any other trouble.
However, because fat tissue makes the hormone leptin, people with larger areas of acquired lipodystrophy might not have enough of this chemical in their bodies. Leptin tells your body you've eaten enough and to make insulin. Fat could also build up in places it shouldn't, like the blood, heart, liver, and kidneys. Depending on which type of lipodystrophy a person has, it may cause other problems, including diabetes, high cholesterol and triglycerides, liver disease, and kidney failure.
Doctors can help you manage these complications. And cosmetic surgery might be an option if looks are a concern.
Causes
Often, doctors don't know what causes acquired lipodystrophy, but some triggers are:
- An infection, such as measles, pneumonia, infectious mononucleosis, or hepatitis
- A disease where your immune system attacks your body (called an autoimmune disease)
- Repeated injections in or pressure on the same place on your body
- An injury
For example, people with diabetes who have to inject insulin daily tend to get localized lipodystrophy where they keep giving themselves shots. That's a good reason to change your injection site often.
Symptoms
While all kinds of acquired lipodystrophy cause a loss of body fat, exactly what that means for each person is different. The type your child has will affect:
- Where it happens
- How much fat is lost
- Other effects on their body
AGL. They'll lose fat from under the skin all over their body, including their face, arms, legs, palms, and sometimes the soles of their feet. They could look very muscular, and you’ll be able to see veins under their skin.
Kids with AGL are very hungry all the time and grow fast. Adults may have large hands and feet and a strong, square jawbone if their hormone balance is off and they've kept growing. They could have larger than usual sex organs (clitoris and ovaries, penis and testicles).
A woman might have irregular periods or none at all. They could have polycystic ovary syndrome (PCOS). They'll probably have extra hair on their upper lip and chin.
Some people with AGL have patches of dark, velvety skin in their underarms, on their neck, around their belly button or nipples, or on their hands and feet.
Because of the fat loss, a person may have problems using sugar in their body or controlling their blood sugar and triglyceride levels. They could have a large liver or spleen.
APL. This type affects just the upper body, on both sides. It usually starts with their face and moves to their neck, arms, and chest.
Localized. This looks like a dent in the skin, but the skin itself seems fine. The size can vary. It could be in one spot or many. There might also be tender or painful bumps.
Getting a Diagnosis
When you go to the doctor, they'll do a full exam and ask questions about your child’s health:
- What symptoms have you noticed?
- When did you first see them?
- Are changes in how they looks only in certain areas, or all over?
- Have they had panniculitis -- swollen bumps under their skin or a bumpy red rash?
- Do they have diabetes?
- What other health problems or recent injuries have they had?
- Have you had their blood sugar, cholesterol, and triglyceride levels checked?
Tests of body fat can confirm the diagnosis.
For a skin biopsy, the doctor will cut a small piece of skin and check the cells under a microscope.
Your doctor may also look for a pattern of fat loss with:
- Skinfold thickness measurements, checking how much skin they can pinch between their fingers at specific spots on their body
- A special X-ray that measures bone mineral density
- A special whole-body MRI (magnetic resonance imaging) that uses powerful magnets and radio waves to make pictures showing tissues with fat
Blood tests check:
- Blood sugar
- Kidney health
- Fats
- Liver enzymes
- Uric acid
If the doctor suspects APL, they'll check their blood for evidence of a specific way the body attacks fat cells.
Urine tests check for kidney problems.
Questions for Your Doctor
- What type of lipodystrophy is this?
- Do you know what caused it?
- Do we need any more tests?
- How many other people with this condition have you treated?
- What's the best way for us to treat it?
- What other symptoms should we watch for?
- Do we need to see any other doctors?
- Is there anything I can do that will help my child look and feel "normal"?
- Can we be part of a lipodystrophy research trial?
Treatment
Since you can't replace the missing body fat, your aim will be to avoid complications of the disease. A healthy lifestyle plays a big role.
Everyone with lipodystrophy should eat a low-fat diet. But children still need enough calories and good nutrition so they grow properly. Exercise will help your child stay healthy, too. Physical activity lowers blood sugar and can keep fat from building up dangerously.
People with AGL may be able to get metreleptin injections (Myalept) to replace the missing leptin and help prevent other diseases. Statins and omega-3 fatty acids, found in some fish, can help control high cholesterol or triglycerides, too.
If your child has or gets diabetes, they'll need to take insulin or other drugs to control their blood sugar.
Women with AGL shouldn't use oral birth control or hormone replacement therapy for menopause because they can make levels of certain fats worse.
Your doctor may prescribe a lotion or cream to lighten and soften dark skin patches. Over-the-counter bleaches and skin scrubs probably won't work and could irritate the skin.
As your child gets older, they may be able to get plastic surgery to help fill out their face with skin grafts from their thighs, belly, or scalp. Doctors can also use implants and injections of fillers to help reshape facial features. People with APL who have extra fat deposits can use liposuction to get rid of some, but fat may build up again. Talk to your doctor about what approach for their appearance makes sense and when.
Taking Care of Your Child
Because this condition affects how you look, care and compassion are as important as medicine. Focus on keeping your child healthy and being supportive.
Set the tone for others. Be positive and open-minded. People may not know how to react or what to say to keep from prying, or offending or embarrassing you and your child. When someone asks about them, be matter-of-fact about their condition.
Do what you can to boost their self-esteem. Try to focus your praise on achievements, rather than appearance.
Encourage friendships. But kids will be kids, so prepare them for unkind looks and words. You can help them practice how they’ll react with role-play and humor.
Consider professional counseling. Someone with training can help your child and your family sort out their feelings as they deal with the challenges of this disease.
What to Expect
Over time, people with AGL can lose most or all of their body fat. With APL, it typically stops after a few years.
In general, the more fat you lose, the more serious the condition is. Yet many people with lipodystrophy live active, productive lives.
You'll need to work closely with your doctor to prevent complications. For example, people with AGL are likely to have heart and liver problems. Diabetes can be hard to control. They might develop autoimmune disorders such as vitiligo (light-colored spots of skin), rheumatoid arthritis, and a kind of hepatitis.
People with APL probably won't have the insulin-related problems that often come with AGL. But it can lead to kidneys that don't work well or at all, and drusen, tiny fat deposits in the back of the eyes that may be connected to age-related macular degeneration (AMD). Women may get extra fat on their hips and thighs. AGL and APL can be linked to autoimmune disorders, too, including rheumatoid arthritis and celiac disease.
Researchers are studying lipodystrophy, and they may find more ways to treat it.
Getting Support
If you're looking for a community, Lipodystrophy United is a good place to start. It has information about the disease as well as an online community for people with lipodystrophy and their families.

